Preeclampsia - self-care
Toxemia - self-care; PIH - self-care; Pregnancy-induced hypertension - self-care
Images
Animation

Description
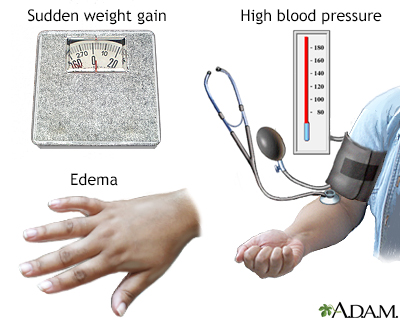
Pregnant women with preeclampsia have high blood pressure and signs of liver or kidney damage. Kidney damage results in the presence of protein in the urine. Preeclampsia that occurs in women after the 20th week of pregnancy can be mild or severe. Preeclampsia usually resolves after the baby is born and the placenta is delivered. However, it may persist or even begin after delivery, most often within 48 hours. This is called postpartum preeclampsia.
What to Expect
Treatment decisions are made based on the gestational age of the pregnancy and the severity of the preeclampsia.
If you are past 37 weeks and have been diagnosed with preeclampsia, your health care provider will likely advise you to deliver early. This may involve receiving medicines to start (induce) labor or delivering your baby by cesarean delivery (C-section).
If you are less than 37 weeks pregnant, the goal is to prolong your pregnancy as long as it is safe. Doing so allows your baby to develop longer inside you.
- How quickly you should deliver depends on how high your blood pressure is, any signs of liver or kidney problems, and the condition of your baby.
- If your preeclampsia is severe, you may need to stay in the hospital to be monitored closely. If the preeclampsia remains severe, your baby may need to be delivered.
- If your preeclampsia is mild, you may be able to stay at home on bed rest. You will need to have frequent checkups and tests. The severity of preeclampsia may change quickly, so you'll need very careful follow-up.
Complete bed rest is no longer recommended. Your provider will recommend an activity level for you.
Self-care at Home
When you are at home, your provider will tell you what changes you may need to make in your diet.
You may need to take medicines to lower your blood pressure. Take these medicines the way your provider tells you to.
Do not take any extra vitamins, calcium, aspirin, or other medicines without talking with your provider first.
Often, women who have preeclampsia do not feel sick or have any symptoms. Still, both you and your baby may be in danger. To protect yourself and your baby, it's important to go to all of your prenatal visits. If you notice any symptoms of preeclampsia (listed below), tell your provider right away.
Risks of Preeclampsia
There are risks to both you and your baby if you develop preeclampsia:
- The mother can have kidney damage, seizures, stroke, or bleeding in the liver.
- There is a higher risk for the placenta to detach from the uterus (abruption) and for stillbirth.
- Your baby may fail to grow properly (growth restriction).
Monitoring You and Your Baby
While you are home, your provider may ask you to:
- Measure your blood pressure
- Check your urine for protein
- Monitor how much fluid you drink
- Check your weight
- Monitor how often your baby moves and kicks
Your provider will teach you how to do these things.
You will need frequent visits with your provider to make sure you and your baby are doing well. You will likely have:
- Visits with your provider once a week or more. You may be referred to a high risk specialist.
- Ultrasounds to monitor the size and movement of your baby and the amount of fluid around your baby.
- A nonstress test to check your baby's condition.
- Blood or urine tests.
Sign and symptoms of preeclampsia most often go away within 6 weeks after delivery. However, the high blood pressure sometimes gets worse the first few days after delivery. You are still at risk for preeclampsia up to 6 weeks after delivery. This postpartum preeclampsia carries a higher risk of death. It's important to continue monitoring yourself during this time. If you notice any symptoms of preeclampsia, before or after delivery, contact your provider right away.
When to Call the Doctor
Contact your provider right away if you:
- Have swelling in your hands, face, or eyes (edema)
- Suddenly gain weight over 1 or 2 days, or you gain more than 2 pounds (1 kilogram) in a week
- Have a headache that does not go away or becomes worse
- Are not urinating very often
- Have nausea and vomiting
- Have vision changes, such as you cannot see for a short time, see flashing lights or spots, are sensitive to light, or have blurry vision
- Feel lightheaded or faint
- Have pain in your belly below your ribs, more often on the right side
- Have pain in your right shoulder
- Have problems breathing
- Bruise easily
- Notice the baby is moving less
- Have vaginal bleeding
References
American College of Obstetricians and Gynecologists website. Gestational hypertension and preeclampsia: ACOG Practice Bulletin, Number 222. Obstet Gynecol. 2020;135(6):e237-e260. PMID: 32443079 pubmed.ncbi.nlm.nih.gov/32443079/.
Harper LM, Tita A, Karumanchi SA. Pregnancy-related hypertension. In: Lockwood CJ, Copel JA, Dugoff L, et al, eds. Creasy and Resnik's Maternal-Fetal Medicine: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2023:chap 45.
Jeyabalan A. Hypertensive disorders of pregnancy. In: Martin RJ, Fanaroff AA, eds. Fanaroff and Martin's Neonatal-Perinatal Medicine. 12th ed. Philadelphia, PA: Elsevier; 2025:chap 16.
Sibai BM. Preeclampsia and hypertensive disorders. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics: Normal and Problem Pregnancies. 8th ed. Philadelphia, PA: Elsevier; 2021:chap 38.
BACK TO TOPReview Date: 10/15/2024
Reviewed By: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
