Lymph node biopsy
Biopsy - lymph nodes; Open lymph node biopsy; Fine needle aspiration biopsy; Sentinel lymph node biopsy
A lymph node biopsy is the removal of lymph node tissue for examination under a microscope.
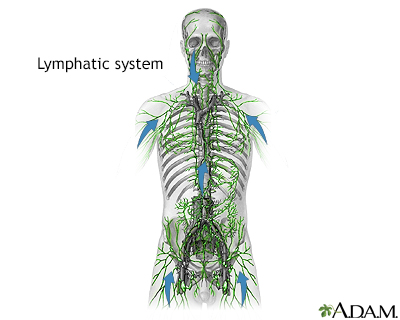
The lymph nodes are small glands that make white blood cells (lymphocytes), which fight infection. Lymph nodes may trap the germs that are causing an infection. Cancer can spread to lymph nodes.
Images
I Would Like to Learn About:
How the Test is Performed
A lymph node biopsy is often done in an operating room in a hospital or at an outpatient surgical center. The biopsy may be done in different ways.
An open biopsy is surgery to remove all or part of the lymph node. This is usually done if there is a lymph node that can be felt on exam. This can be done with local anesthesia (numbing medicine) injected into the area, or under general anesthesia. The procedure is typically done in the following way:
- You lie on the exam table. You may be given medicine to calm you and make you sleepy or you may have general anesthesia, which means you are asleep and pain-free.
- The biopsy site is cleansed.
- A small surgical cut (incision) is made. The lymph node or part of the node is removed.
- The incision is closed with stitches and a bandage or liquid adhesive is applied.
- An open biopsy may take 30 to 45 minutes.
For some cancers, a special way of finding the best lymph node to biopsy is used. This is called sentinel lymph node biopsy, and it involves:
A tiny amount of a tracer, either a radioactive tracer (radioisotope) or a blue dye or both, is injected at the tumor site or in the area of the tumor.
The tracer or dye flows into the nearest (local) node or nodes. These nodes are called the sentinel nodes. The sentinel nodes are the first lymph nodes to which a cancer may spread.
The sentinel node or nodes are removed.
Lymph node biopsies in the belly may be performed with a laparoscope. This is a small tube with a light and camera that is inserted through a small incision in the abdomen. One or more incisions will be made and tools will be inserted to help remove the node. The lymph node is located and part or all of it is removed. This is usually performed under general anesthesia, which means the person having this procedure will be asleep and pain-free.
After the sample is removed, it is sent to the laboratory for examination.
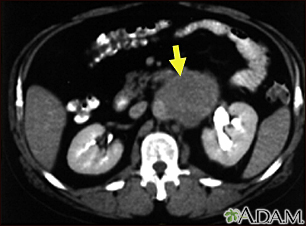
A needle biopsy involves inserting a needle into a lymph node. This type of biopsy can be performed by a radiologist with local anesthesia, using ultrasound or CT scan to find the node. It can also be performed by a surgeon without imaging if the lymph node can be felt.
How to Prepare for the Test
Tell your surgeon:
- If you are pregnant
- If you have any allergies to medicines
- If you have bleeding problems
- What medicines you are taking (including any supplements or herbal remedies)
Your surgeon may ask you to:
- Stop taking any blood thinners, such as aspirin, heparin, warfarin (Coumadin), or clopidogrel (Plavix) as directed
- Not eat or drink anything after a certain period of time before the biopsy
- Arrive at a certain time for the procedure
How the Test will Feel
When the local anesthetic is injected, you will feel a prick and a mild stinging. The biopsy site will be sore for a few days after the test.
After an open or laparoscopic biopsy, the pain is usually mild and you can easily control it with an over-the-counter pain medicine. You may also notice some bruising or fluid leaking for a few days. Follow instructions for taking care of the incision. While the incision is healing, avoid any type of intense exercise or heavy lifting that causes pain or discomfort. Ask your surgeon for specific instructions about what activities you can do.
Why the Test is Performed
The test is used to diagnose cancer, sarcoidosis, or an infection (such as tuberculosis):
- When you or your health care provider feel swollen lymph glands and they do not go away
- When abnormal lymph nodes are present on a mammogram, ultrasound, CT, or MRI scan
- For some people with cancer, such as breast cancer or melanoma, to see if the cancer has spread (sentinel lymph node biopsy or needle biopsy by a radiologist)
The results of the biopsy help your provider decide on further tests and treatments.
Normal Results
If a lymph node biopsy does not show any signs of cancer, it is more likely that other lymph nodes nearby are also cancer-free. This information can help the provider decide about further tests and treatments.
What Abnormal Results Mean
Abnormal results may be due to many different conditions, from very mild infections to cancer.
For example, enlarged lymph nodes may be due to:
- Cancers (breast, lung, oral)
- HIV
- Cancer of the lymph tissue (Hodgkin or non-Hodgkin lymphoma)
- Infection (tuberculosis, cat scratch disease)
- Inflammation of lymph nodes and other organs and tissues (sarcoidosis)
Risks
Lymph node biopsy may result in any of the following:
- Bleeding
- Infection (in rare cases, the wound may get infected and you may need to take antibiotics)
- Nerve injury if the biopsy is done on a lymph node close to nerves (the numbness usually goes away in a few months)
Related Information
CancerSwollen lymph nodes
Hodgkin lymphoma
Non-Hodgkin lymphoma
Sarcoidosis
References
Dinulos JGH. Nevi and malignant melanoma. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 22.
National Cancer Institute website. Sentinel lymph node biopsy. www.cancer.gov/about-cancer/diagnosis-staging/staging/sentinel-node-biopsy-fact-sheet. Updated June 25, 2019. Accessed June 6, 2024.
BACK TO TOPReview Date: 5/29/2024
Reviewed By: Debra G. Wechter, MD, FACS, General Surgery Practice Specializing in Breast Cancer, Virginia Mason Medical Center, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
