Trypsinogen test
Serum trypsin; Trypsin-like immunoreactivity; Serum trypsinogen; Immunoreactive trypsin
Trypsinogen is a substance that is normally produced in the pancreas and released into the small intestine. Trypsinogen is converted to trypsin. Then it starts the process needed to break down proteins into their building blocks (called amino acids).
A test can be done to measure the amount of trypsinogen in your blood.
Images
I Would Like to Learn About:
How the Test is Performed
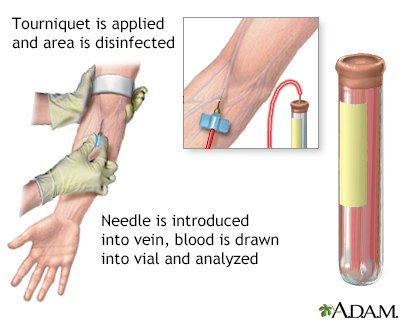
A blood sample is taken from a vein. The blood sample is sent to a lab for testing.
How to Prepare for the Test
There are no special preparations. You may be asked to not eat or drink for 8 hours before the test.
How the Test will Feel
You may feel slight pain or a sting when the needle is inserted to draw blood. Afterward, there may be some throbbing.
Why the Test is Performed
This test is done to detect diseases of the pancreas.
The test is also used to screen newborn babies for cystic fibrosis.
Normal Results
Normal value ranges may vary slightly among different laboratories. Talk to your health care provider about the meaning of your specific test results.
What Abnormal Results Mean
Increased levels of trypsinogen may be due to:
- Abnormal production of pancreatic enzymes
- Acute pancreatitis
- Cystic fibrosis
- Pancreatic cancer
Very low levels may be seen in people with chronic pancreatitis.
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight, but may include:
- Fainting or feeling lightheaded
- Multiple punctures to locate veins
- Hematoma (blood buildup under the skin)
- Excessive bleeding
- Infection (a slight risk any time the skin is broken)
Considerations
Other tests used to detect pancreas diseases may include:
- Serum amylase
- Serum lipase
Related Information
EnzymeProtein in diet
Duodenum
Pancreatic cancer
Acute
Chronic pancreatitis
References
Chernecky CC, Berger BJ. Trypsin- plasma or serum. In: Chernecky CC, Berger BJ, eds. Laboratory Tests and Diagnostic Procedures. 6th ed. St Louis, MO: Elsevier Saunders; 2013:1125-1126.
Forsmark CE. Chronic pancreatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 59.
Siddiqi HA, Rabinowitz S, Axiotis CA. Laboratory diagnosis of gastrointestinal and pancreatic disorders. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 23.
BACK TO TOPReview Date: 1/30/2023
Reviewed By: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
