Intracranial pressure monitoring
ICP monitoring; CSF pressure monitoring
Intracranial pressure (ICP) monitoring uses a device placed inside the head. The monitor senses the pressure inside the skull and sends measurements to a recording device.
Images
I Would Like to Learn About:
How the Test is Performed
There are three ways to monitor ICP. ICP is the pressure in the skull. These procedures are most often done on people with life-threatening neurological emergencies.
INTRAVENTRICULAR CATHETER
The intraventricular catheter is the most accurate monitoring method.
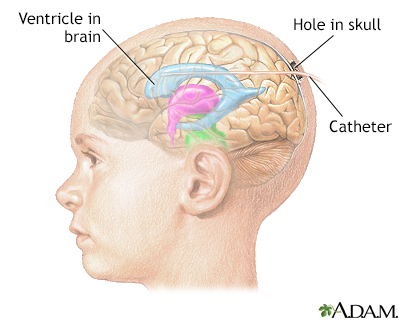
To insert an intraventricular catheter, a hole is drilled through the skull. The catheter is inserted through the brain into the lateral ventricle. This area of the brain contains cerebrospinal fluid (CSF). CSF is a liquid that protects the brain and spinal cord.
The intraventricular catheter can also be used to drain fluid out through the catheter.
The catheter may be hard to get into place when the intracranial pressure is high.
SUBDURAL SCREW (BOLT)
This method is used if monitoring needs to be done right away. A hollow screw is inserted through a hole drilled in the skull. It is placed through the membrane that protects the brain and spinal cord (dura mater). This allows the sensor to record from inside the subdural space.
EPIDURAL SENSOR
An epidural sensor is inserted between the skull and dural tissue. The epidural sensor is placed through a hole drilled in the skull. This procedure is less invasive than other methods, but it cannot remove excess CSF.
- First the area is shaved and cleansed with antiseptic.
- After the area is dry, a surgical cut is made. The skin is pulled back until the skull is seen.
- A drill is then used to cut through the bone.
How to Prepare for the Test
Most of the time, this procedure is done when a person is in the hospital intensive care unit. If you are awake and aware, your health care provider will explain the procedure and the risks. You will have to sign a consent form.
How the Test will Feel
If the procedure is done using general anesthesia, you will be asleep and pain-free. When you wake up, you will feel the normal side effects of anesthesia. You will also have some discomfort from the cut made in your skull.
If the procedure is done under local anesthesia, you will be awake. Numbing medicine will be injected to the place where the cut is to be made. This will feel like a prick on your scalp, like a bee sting. You may feel a tugging sensation as the skin is cut and pulled back. You will hear a drill sound as it cuts through the skull. The amount of time this takes will depend on the type of drill that is used. You will also feel a tugging as the surgeon sutures the skin back together after the procedure.
Your provider may give you mild pain medicines to ease your discomfort. You may not get strong pain medicines, because your provider will want to check for signs of brain function.
Why the Test is Performed
This test is most often done to measure ICP. It may be done when there is a severe head injury or brain/nervous system disease. It also may be done after surgery to remove a tumor or fix damage to a blood vessel if the surgeon is worried about brain swelling.
High ICP can be treated by draining CSF through the catheter. It can also be treated by:
- Changing the ventilator settings for people who are on a respirator
- Giving certain medicines through a vein (intravenously)
Normal Results
Normally, the ICP ranges from 1 to 20 mm Hg.
Talk to your provider about the meaning of your specific test results.
What Abnormal Results Mean
High ICP means that both nervous system and blood vessel tissues are under pressure. If not treated, this can lead to permanent damage. In some cases, it can be life threatening.
Risks
Risks from the procedure may include:
- Bleeding
- Brain herniation or injury from the increased pressure
- Damage to the brain tissue
- Inability to find the ventricle and place catheter
- Infection
- Risks of general anesthesia
References
DiGiorgio AM, Huang MC, Wang VY, Manley GT. Intracranial pressure monitoring. In: Winn HR, ed. Youmans and Winn Neurological Surgery. 8th ed. Philadelphia, PA: Elsevier; 2023:chap37.
Oddo M, Taccone F. Intracranial pressure monitoring. In: Vincent J-L, Abraham E, Moore FA, Kochanek PM, Fink MP, eds. Textbook of Critical Care. 8th ed. Philadelphia, PA: Elsevier; 2024:chap E20.
Rabinstein AA, Braksick SA. Neurointensive care. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 53.
Robba C. Intracranial pressure monitoring. In: Prabhakar H, ed. Neuromonitoring Techniques. Philadelphia, PA: Elsevier; 2018:chap 1.
BACK TO TOPReview Date: 4/29/2023
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School of Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
