Headache
Pain - head; Rebound headaches; Medication overuse headaches; Medicine overuse headaches
A headache is pain or discomfort in the head, scalp, or neck. Serious causes of headaches are rare. Most people with headaches can feel much better by making lifestyle changes, learning ways to relax, and sometimes by taking medicines.
Images
I Would Like to Learn About:
Causes
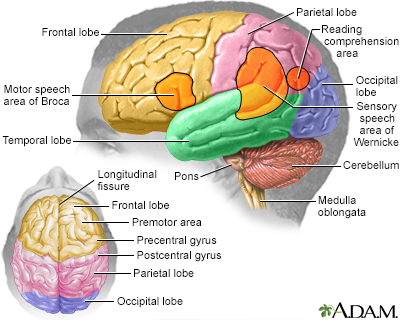
The most common type of headache is tension headache. It is likely caused by tight muscles in your shoulders, neck, scalp, and jaw. A tension headache:
- May be related to stress, depression, anxiety, a head injury, or holding your head and neck in an abnormal position.
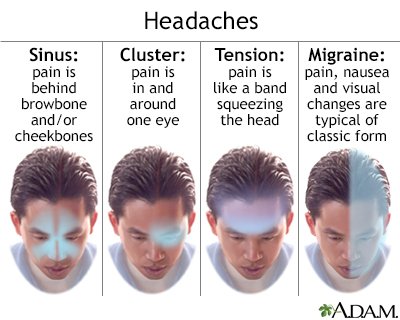
- Tends to be on both sides of your head. It often starts at the back of the head and spreads forward. The pain may feel dull or squeezing, like a tight band or vice. Your shoulders, neck, or jaw may feel tight or sore.
A migraine headache involves pain that is throbbing, pounding, or pulsating, and is on one side of your head. It often occurs with other symptoms, such as vision changes, sensitivity to sound or light, or nausea. With a migraine:
- The headache may be associated with an aura. This is a group of warning symptoms that start before your headache.
- The pain usually gets worse as you try to move around.
- Migraines may be triggered by foods, such as chocolate, certain cheeses, or monosodium glutamate (MSG). Caffeine withdrawal, lack of sleep, and alcohol may also be triggers.
Rebound headaches are headaches that keep coming back. They often occur from overuse of pain medicines for other headaches like migraine or tension headaches. For this reason, these headaches are also called medicine overuse headaches. People who take pain medicine more than 3 days a week on a regular basis can develop this type of headache.
Other types of headaches:
- Cluster headache is a sharp, very painful headache that occurs daily, sometimes up to several times a day for months. It then goes away for weeks to months. In some people, the headaches never come back. The headache usually lasts less than an hour. It tends to occur at the same times every day.
- Sinus headache causes pain in the front of the head and face. It is due to swelling in the sinus passages behind the cheeks, nose, and eyes. The pain is worse when you bend forward and when you first wake up in the morning.
- Headaches may occur if you have a cold, the flu, a fever, or premenstrual syndrome.
- Headache due to a disorder called temporal arteritis. This is a swollen, inflamed artery that supplies blood to part of the head, temple, and neck area.
In rare cases, a headache can be a sign of something more serious, such as:
- Bleeding in the area between the brain and the thin tissue that covers the brain (subarachnoid hemorrhage)
- Blood pressure that is very high (hypertension)
- Brain infection, such as meningitis or encephalitis, or abscess
- Brain tumor
- Buildup of fluid inside the skull that leads to brain swelling (hydrocephalus)
- Buildup of pressure inside the skull that appears to be, but is not a tumor (pseudotumor cerebri)
- Carbon monoxide poisoning
- Lack of oxygen during sleep (sleep apnea)
- Problems with the blood vessels and bleeding in the brain, such as arteriovenous malformation (AVM), brain aneurysm, or stroke
Home Care
There are things you can do to manage headaches at home, especially migraines or tension headaches. Try to treat the symptoms right away.
When migraine symptoms begin:
- Drink water to avoid getting dehydrated, especially if you have vomited.
- Rest in a quiet, dark room.
- Place a cool cloth on your head.
- Use any relaxation techniques you have learned.
A headache diary can help you identify your headache triggers. When you get a headache, write down the following:
- Day and time the pain began
- What you ate and drank over the past 24 hours
- How much you slept
- What you were doing and where you were right before the pain started
- How long the headache lasted and what made it stop
Review your diary with your health care provider to identify triggers or a pattern to your headaches. This can help you and your provider create a treatment plan. Knowing your triggers can help you avoid them.
Your provider may have already prescribed medicine to treat your type of headache. If so, take the medicine as instructed.
For tension headaches, try acetaminophen, aspirin, or ibuprofen. Talk to your provider if you are taking pain medicines 3 or more days a week.
When to Contact a Medical Professional
Some headaches may be a sign of a more serious illness. Seek medical help right away for any of the following:
- This is the first headache you have ever had in your life and it interferes with your daily activities.
- Your headache comes on suddenly and is explosive or violent. This kind of headache needs medical attention right away. It may be due to a ruptured blood vessel in the brain. Call 911 or the local emergency number or go to the nearest emergency room.
- Your headache is "the worst ever," even if you regularly get headaches.
- You also have slurred speech, a change in vision, problems moving your arms or legs, loss of balance, confusion, or memory loss with your headache.
- Your headache gets worse over 24 hours.
- You also have a fever, stiff neck, nausea, and vomiting with your headache.
- Your headache occurs with a head injury.
- Your headache is severe and just in one eye, with redness in that eye.
- You just started getting headaches, especially if you are older than 50.
- Your headaches are associated with vision problems, pain while chewing, or weight loss.
- You have a history of cancer or immune system problem (such as HIV/AIDS) and develop a new headache.
What to Expect at Your Office Visit
Your provider will take a medical history and will examine your head, eyes, ears, nose, throat, neck, and nervous system.
Your provider will ask many questions to learn about your headaches. Diagnosis is usually based on your history of symptoms.
Tests may include:
- Blood tests or a lumbar puncture if you may have an infection
- Head CT scan or MRI if you have any danger signs or you have been having headaches for a while
- Sinus x-rays
- CT or MR angiography
Related Information
Tension headacheCluster headache
Headache - what to ask your doctor
References
Digre KB. Headaches and other head pain. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 367.
Garza I, Robertson CE, Smith JH, Whealy MA. Headache and other craniofacial pain. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 102.
Rozental JM. Tension-type headache, chronic tension-type headache, and other chronic headache types. In: Benzon HT, Raja SN, Liu SS, Fishman SM, Cohen SP, eds. Essentials of Pain Medicine. 4th ed. Philadelphia, PA: Elsevier; 2018:chap 20.
BACK TO TOPReview Date: 12/31/2023
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
