Skin graft
Skin transplant; Skin autografting; FTSG; STSG; Split thickness skin graft; Full thickness skin graft
A skin graft is a patch of skin that is removed by surgery from one area of the body and transplanted, or attached, to another area.
Images
Presentation
I Would Like to Learn About:
Description
This surgery is usually done while you are under general anesthesia. That means you will be asleep and pain-free.
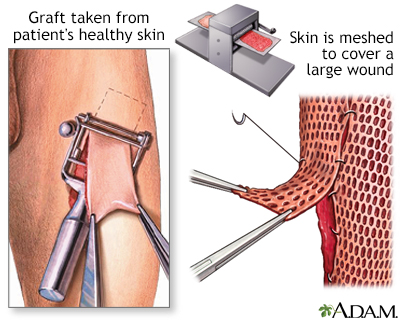
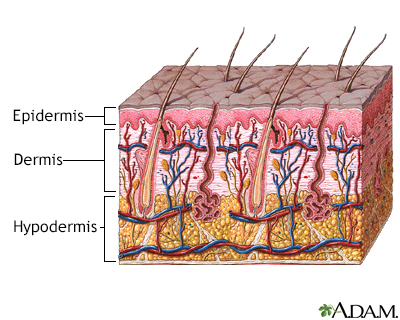
Healthy skin is taken from a place on your body called the donor site. Most people who are having a skin graft have a split-thickness skin graft. This takes the two top layers of skin from the donor site (the epidermis) and the layer under the epidermis (the dermis).
The donor site can be any area of the body. Most times, it is an area that is hidden by clothes, such as the buttock, back, or inner thigh.
The graft is carefully spread on the bare area where it is being transplanted. It is held in place either by gentle pressure from a well-padded dressing that covers it, or by staples or a few small stitches. The donor-site area is covered with a sterile dressing for 3 to 5 days.
People with deeper tissue loss, or in a cosmetic area such as the face, may need a full-thickness skin graft. This requires the entire thickness of skin from the donor site, not just the top two layers.
A full-thickness skin graft is a more complicated procedure. Common donor sites for full-thickness skin grafts include the chest wall, neck, back, or abdominal wall.
Why the Procedure Is Performed
Skin grafts may be recommended for:
- Areas where there has been infection that caused a large amount of skin loss
- Burns
- Cosmetic reasons or reconstructive surgeries where there has been skin damage or skin loss
- Skin cancer surgery
- Surgeries that need skin grafts to heal
- Venous ulcers, pressure ulcers, or diabetic ulcers that do not heal
- Very large wounds
- A wound that the surgeon has not been able to close properly
Full-thickness grafts are sometimes done when a lot of tissue is lost. This can happen with open fractures of the lower leg, or after severe infections.
Risks
Risks for anesthesia and surgery in general are:
- Allergic reactions to medicines
- Nausea and vomiting
- Problems with breathing
- Bleeding, blood clots, or infection
Risks for this surgery are:
- Bleeding
- Chronic pain (rarely)
- Infection
- Loss of grafted skin (the graft not healing, or the graft healing slowly)
- Reduced or lost skin sensation, or increased sensitivity
- Scarring
- Skin discoloration
- Uneven skin surface
- Poor wound healing and scarring at the donor site
Before the Procedure
Tell your surgeon or nurse if:
- You are or could be pregnant
- You are taking any medicines, including medicines, drugs, supplements, or herbs you bought without a prescription
Planning for your surgery:
- If you have diabetes, heart disease, or other medical conditions, your surgeon may ask you to see the health care provider who treats you for these conditions.
- If you smoke, it's important to cut back or quit. Smoking can slow healing and increase the risk for blood clots. Ask your provider for help quitting smoking.
- If needed, prepare your home to make it easier to recover after surgery.
- Ask your surgeon if you need to arrange to have someone drive you home after your surgery
During the week before your surgery:
- You may be asked to temporarily stop taking medicines that keep your blood from clotting. These medicines are called blood thinners. This includes over-the-counter medicines and supplements such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), and vitamin E. Many prescription medicines are also blood thinners.
- Ask your surgeon which medicines you should still take on the day of surgery.
- Let your surgeon know about any illness you may have before your surgery. This includes COVID-19, cold, flu, fever, herpes breakout, or other illness. If you do get sick, your surgery may need to be postponed.
On the day of surgery:
- Follow instructions about when to stop eating and drinking.
- Take the medicines your surgeon told you to take with a small sip of water.
- Arrive at the hospital on time.
After the Procedure
You should recover quickly after split-thickness skin grafting. Full-thickness grafts need a longer recovery time. If you received this kind of graft, you may need to stay in the hospital for recovery.
After you are discharged from the hospital, follow instructions on how to care for your skin graft, including:
- Wearing a dressing for 1 to 2 weeks. Ask your provider how you should care for the dressing, such as protecting it from getting wet.
- Protecting the graft from trauma for 3 to 4 weeks. This includes avoiding being hit or doing any exercise that might injure or dislodge the graft.
- Getting physical therapy, if your surgeon recommends it.
Outlook (Prognosis)
Most skin grafts are successful, but some do not heal well. You may need additional procedures to get the desired result.
Related Information
BurnsSurgical wound care - open
Preventing pressure ulcers
References
Loder S, Levi B, Clark A. Skin grafting. In: Gurtner GC, Pusic AL, eds. Plastic Surgery, Volume 1: Principles. 5th ed. Philadelphia, PA: Elsevier; 2024:chap 17.
Padilla PL, Khoo KH, Ho T, Cole EL, Sirvent RZ, Phillips LG. Plastic surgery. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. St Louis, MO: Elsevier; 2022:chap 69.
Ratner D, Nayyar PM. Grafts. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 148.
BACK TO TOPReview Date: 1/21/2025
Reviewed By: Jonas DeMuro, MD, Diplomate of the American Board of Surgery with added Qualifications in Surgical Critical Care, Assistant Professor of Surgery, Renaissance School of Medicine, Stony Brook, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
