Tick bite
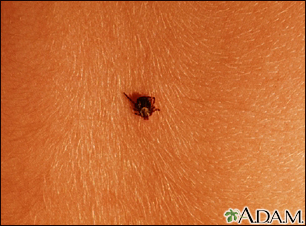
Ticks are bugs that can attach to you as you brush past bushes, plants, and grass. Once on you, ticks often move to a warm, moist place on your body, like the armpits, groin, and hair. There, they typically attach firmly to your skin and begin to draw blood. Avoiding ticks is important because they can infect you with bacteria and other organisms that cause illness.
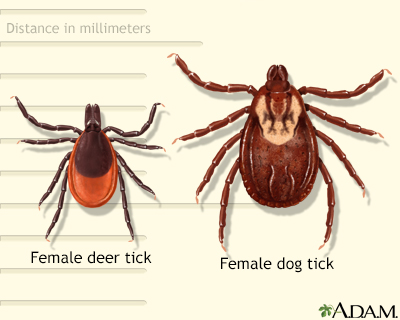
Ticks can be fairly large, about the size of a pencil eraser, or so small that they are almost impossible to see. There are about 850 different types of ticks. Most tick bites are harmless, but some can cause mild to serious health conditions.
This article describes the effects of a tick bite.
This article is for information only. DO NOT use it to treat or manage a tick bite. If you or someone you are with is bitten by a tick, call the local emergency number (such as 911), or the local poison control center can be reached directly by calling the national toll-free Poison Help hotline (1-800-222-1222) from anywhere in the United States.
Images



I Would Like to Learn About:
Poisonous Ingredient
Hard- and soft-bodied female ticks are believed to make a poison that can cause tick paralysis in children.
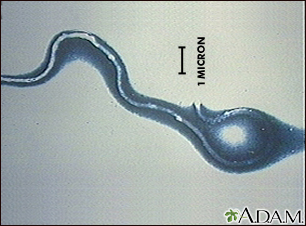
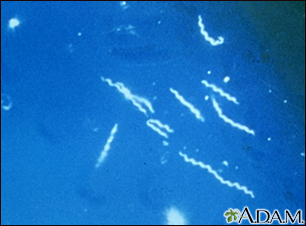
Most ticks do not carry diseases, but some carry bacteria or other organisms that can cause:
These and other illnesses may cause heart, nervous system, kidney, adrenal gland, and liver damage, and may cause death.
Where Found
Ticks live in wooded areas or grassy fields.
Symptoms
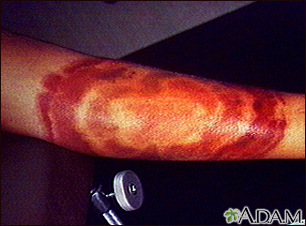
Watch for symptoms of tick-borne diseases in the weeks after a tick bite. These include muscle or joint aches, stiff neck, headache, weakness, fever, swollen lymph nodes, and other flu-like symptoms. Watch for a red spot or rash starting at the site of the bite (called "erythema migrans").
The symptoms below are from the bite itself, not from the diseases a bite may cause. Some of the symptoms are caused by one variety of tick or another, but may not be common to all ticks.
- Stopped breathing
- Difficulty breathing
- Blisters
- Rash
- Severe pain at site, lasting several weeks (from some kinds of ticks)
- Swelling at site (from some kinds of ticks)
- Weakness
- Uncoordinated movement
Home Care
Below is the proper way to remove an attached tick:
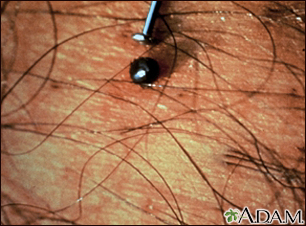
- Use tweezers to grasp the tick as close to the skin surface as possible. Gloved or protected fingers may be used if no tweezers are available.
- Pull straight up gently but firmly, using steady pressure. Do not jerk or twist. Do not squeeze or crush the body of the tick. Fluids from the tick may contain infectious agents.
- Clean the skin thoroughly with soap and water after removing the tick.
- Wash your hands with soap and water.
If possible, place the tick in a closed container and take it to the emergency room.
If the mouthparts or any parts of the tick remain in the skin, they will usually grow out without causing any problems, but local infection is possible.
Before Calling Emergency
Have this information ready:
- Person's age, weight, and condition
- Time the tick bite occurred
- Part of the body affected
Poison Control
Your local poison control center can be reached directly by calling the national toll-free Poison Help hotline (1-800-222-1222) from anywhere in the United States. This national hotline will let you talk to experts in poisoning. They will give you further instructions.
This is a free and confidential service. All local poison control centers in the United States use this national number. You should call if you have any questions about poisoning or poison prevention. It does NOT need to be an emergency. You can call for any reason, 24 hours a day, 7 days a week.
What to Expect at the Emergency Room
The symptoms will be treated. Long-term treatment may be needed if complications develop. Preventive antibiotics are often given to people who live in areas where Lyme disease is common.
The person may receive:
- Blood and urine tests
- Breathing support, including oxygen, a tube down the throat and a breathing machine (ventilator) in serious cases
- Chest x-ray
- ECG (electrocardiogram, or heart tracing)
- Intravenous fluids (through a vein)
- Medicines to treat symptoms
Outlook (Prognosis)
After tick removal and skin cleansing, observe the area for the development of a circular rash called "erythema migrans" for up to 30 days following a tick bite. Contact your health care provider right away if a rash develops.
A tick usually has to be attached for 2 to 3 days before transmitting Lyme disease, so removal of the tick within that time often prevents Lyme transmission. Other infections may occur earlier from a tick bite.
Most tick bites are harmless. The outcome will depend on what type of infection the tick may have been carrying and how soon appropriate treatment was started. If you are bitten by a tick that carried a disease, long-term health effects may occur months or even years later.
Personal protection against bites may be achieved by avoiding areas where ticks are known to be present and applying insect repellents.
To protect yourself against ticks, try to stay away from areas where ticks are known to live. If you are in an area that harbors ticks, apply insect repellant to your body and wear protective clothing. Examine your skin for signs of tick bites or ticks after your travels.
References
Cummins GA, Traub SJ. Tick-borne diseases. In: Auerbach PS, Cushing TA, Harris NS, eds. Auerbach's Wilderness Medicine. 7th ed. Philadelphia, PA: Elsevier; 2017:chap 42.
Curtis AM, Erickson TB. Venomous animal injuries. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 53.
James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM. Parasitic infestations, stings, and bites. In: James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM, eds. Andrews' Diseases of the Skin: Clinical Dermatology. 13th ed. Philadelphia, PA: Elsevier; 2020:chap 20.
Needham GR. Evaluation of five popular methods for tick removal. Pediatrics. 1985;75(6):997-1002. PMID: 4000801 pubmed.ncbi.nlm.nih.gov/4000801/.
Statler VA, Bryant KP. Tickborne infections. In: Long SS, ed. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 89.
BACK TO TOPReview Date: 7/1/2023
Reviewed By: Jesse Borke, MD, CPE, FAAEM, FACEP, Attending Physician at Kaiser Permanente, Orange County, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
