Friedreich ataxia
Friedreich's ataxia; Spinocerebellar degeneration
Friedreich ataxia is a rare disease passed down through families (inherited). It affects the muscles and heart.
Images
Causes
Friedreich ataxia is caused by a defect in a gene called frataxin (FXN). Changes in this gene cause the body to make too much of a part of DNA called trinucleotide repeat (GAA). Normally, the body contains about 8 to 30 copies of GAA. People with Friedreich ataxia have as many as 1,000 copies. The more copies of GAA a person has, the earlier in life the disease starts and the faster it gets worse.
Friedreich ataxia is an autosomal recessive genetic disorder. This means you must get a copy of the defective gene from both your mother and father.
Symptoms
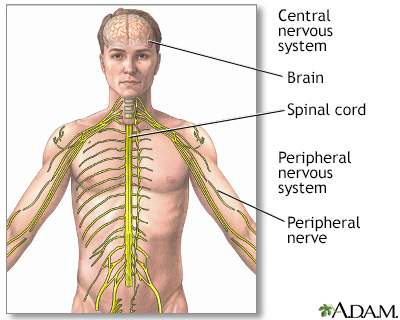
Symptoms are caused by the wearing away of structures in areas of the brain and spinal cord that control coordination, muscle movement, and other functions. Symptoms most often begin before puberty. Symptoms may include:
- Abnormal speech
- Changes in vision, particularly color vision
- Decrease in ability to feel vibrations in lower limbs
- Foot problems, such as hammer toe and high arches
- Hearing loss, this occurs in about 10% of people
- Jerky eye movements
- Loss of coordination and balance, which leads to frequent falls
- Muscle weakness
- No reflexes in the legs
- Unsteady gait and uncoordinated movements (ataxia), which gets worse with time
Muscle problems lead to changes in the spine. This may result in scoliosis or kyphoscoliosis.
Heart disease commonly develops and may lead to heart failure. Heart failure or dysrhythmias that do not respond to treatment may result in death. Diabetes may develop in later stages of the disease.
Exams and Tests
The following tests may be done:
- ECG
- Electrophysiological studies
- Electromyography (EMG)
- Genetic testing
- Nerve conduction tests
- Muscle biopsy
- X-ray, CT scan, or MRI of the head
- X-ray of the chest
- X-ray of the spine
Blood sugar (glucose) tests may show diabetes or glucose intolerance. An eye exam may show damage to the optic nerve, which most often occurs without symptoms.
Treatment
Treatment for Friedreich ataxia includes:
- Counseling
- Speech therapy
- Physical therapy
- Walking aids or wheelchairs
A new medicine, omaveloxolone (Skyclarys), was approved by FDA in 2023 to slow disease progression. Orthopedic devices (braces) may be needed for scoliosis and foot problems. Treating heart disease and diabetes help people live longer and improve their quality of life.
Outlook (Prognosis)
Friedreich ataxia slowly gets worse and causes problems doing everyday activities. Most people need to use a wheelchair within 15 years of the disease's start. The disease may lead to early death.
Possible Complications
Complications may include:
- Diabetes
- Heart failure or heart disease
- Loss of ability to move around
When to Contact a Medical Professional
Contact your health care provider if symptoms of Friedreich ataxia occur, especially if there is a family history of the disorder.
Prevention
People with a family history of Friedreich ataxia who intend to have children may want to consider genetic screening to determine their risk.
Related Information
Autosomal recessiveReferences
Mink JW. Movement disorders. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 637.
Okun MS, Ostrem JL. Other movement disorders. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 379.
BACK TO TOPReview Date: 11/6/2024
Reviewed By: Anna C. Edens Hurst, MD, MS, Associate Professor in Medical Genetics, The University of Alabama at Birmingham, Birmingham, AL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
