Achilles tendinitis
Tendinitis of the heel; Heel pain - Achilles
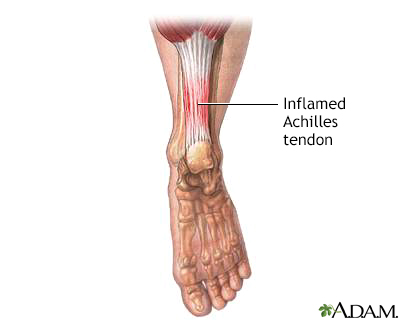
Achilles tendinitis occurs when the tendon that connects the back of your leg to your heel becomes swollen and painful near the bottom of the foot. This tendon is called the Achilles tendon. It allows you to push your foot down. You use your Achilles tendon when walking, running, and jumping.
Images
I Would Like to Learn About:
Causes
There are two large muscles in the calf. These create the power needed to push off with the foot or go up on the toes. The large Achilles tendon connects these muscles to the heel.
Heel pain is most often due to overuse of the foot. Rarely, it is caused by an injury.
Tendinitis due to overuse is most common in younger people. It can occur in walkers, runners, or other athletes.
Achilles tendinitis may be more likely to occur if:
- There is a sudden increase in the amount or intensity of an activity.
- Your calf muscles are very tight (not stretched out).
- You run on hard surfaces, such as concrete.
- You run too often.
- You jump a lot (such as when playing basketball).
- You do not wear shoes that give your feet proper support.
- Your foot suddenly turns in or out.
Tendinitis from arthritis is more common in middle-aged and older adults. A bone spur or growth may form in the back of the heel bone. This may irritate the Achilles tendon and cause pain and swelling. Flat feet will put more tension on the tendon.
Symptoms
Symptoms include pain in the heel and along the length of the tendon when walking or running. The area may feel painful and stiff in the morning.
The tendon may be painful to touch or move. The area may be swollen and warm. You may have trouble standing up on your toes. You may also have trouble finding shoes that fit comfortably due to pain in the back of your heel.
Exams and Tests
The health care provider will perform a physical exam. They will look for tenderness along the tendon and pain in the area of the tendon when you stand on your toes.
X-rays can help diagnose bone problems.
An magnetic resonance imaging (MRI) scan of the foot may be done if you are considering surgery or there is a chance that you have a tear in the Achilles tendon.
Treatment
The main treatments for Achilles tendinitis do not involve surgery. It is important to remember that it may take at least 2 to 3 months for the pain to go away.
Try putting ice on the Achilles tendon area for 15 to 20 minutes, 2 to 3 times per day. Remove the ice if the area gets numb.
Changes in activity may help manage the symptoms:
- Decrease or stop any activity that causes pain.
- Run or walk on smoother and softer surfaces.
- Switch to biking, swimming, or other activities that put less stress on the Achilles tendon.
Your provider or physical therapist can show you stretching exercises or eccentric loading exercises for the Achilles tendon.
You may also need to make changes in your footwear, such as:
- Using a brace, boot or cast to keep the heel and tendon still and allow the swelling to go down
- Placing heel lifts in the shoe under the heel
- Wearing shoes that are softer in the areas over and under the heel cushion
Nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin and ibuprofen, can help ease pain or swelling.
Other treatments include injections, such as platelet rich plasma or steroids, to reduce the inflammation. However, the tendon can become even weaker following injection and should be protected after the injections.
If these treatments do not improve symptoms, you may need surgery to remove inflamed tissue and abnormal areas of the tendon. If there is a bone spur irritating the tendon, surgery can be used to remove the spur.
Extracorporeal shock wave therapy (ESWT) may be an alternative to surgery for people who have not responded to other treatments. This treatment uses low-dose sound waves.
Outlook (Prognosis)
In most cases, lifestyle changes help improve symptoms. Keep in mind that symptoms may return if you do not limit activities that cause pain, or if you do not maintain the strength and flexibility of the tendon.
Possible Complications
Achilles tendinitis may make you more likely to have an Achilles rupture. This condition most often causes a sharp pain that feels as if you have been hit in the back of the heel with a stick. Surgical repair is often necessary. However, the surgery may not be as successful as usual because there is already damage to the tendon due to pre-existing tendonitis.
When to Contact a Medical Professional
Contact your provider if:
- You have pain in the heel around the Achilles tendon that is worse with activity.
- You have sharp pain and are unable to walk or push-off without extreme pain or weakness.
Prevention
Exercises to keep your calf muscles strong and flexible will help reduce the risk for tendinitis. Overusing a weak or tight Achilles tendon makes you more likely to develop tendinitis.
References
Biundo JJ, Canoso JJ. Bursitis, tendinitis, other periarticular disorders, and sports medicine. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 242.
Hogrefe C, Jones EM. Tendinopathy and bursitis. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 103.
Waldman SD. Achilles tendinitis. In: Waldman SD, ed. Atlas of Common Pain Syndromes. 5th ed. Philadelphia, PA: Elsevier; 2024:chap 138.
Waldman SD. The creak sign of Achilles tendinitis. In: Waldman SD, ed. Physical Diagnosis of Pain. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 322.
BACK TO TOPReview Date: 8/27/2024
Reviewed By: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
