Ruptured eardrum
Tympanic membrane perforation; Eardrum - ruptured or perforated; Perforated eardrum
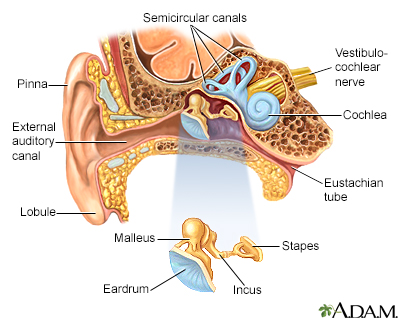
A ruptured eardrum is an opening or hole in the eardrum. The eardrum is a thin piece of tissue that separates the outer and middle ear. Damage to the eardrum may harm hearing.
Images
Presentation

Causes
Ear infections may cause a ruptured eardrum. This occurs more often in children. The infection causes pus or fluid to build up behind the eardrum. As the pressure increases, the eardrum may break open (rupture).
Damage to the eardrum can also occur from:
- A very loud noise close to the ear, such as a gunshot
- A rapid change in ear pressure, which may occur when flying, scuba diving, or driving in the mountains
- Foreign objects in the ear
- Injury to the ear (such as from a powerful slap or explosion)
- Inserting cotton-tipped swabs or small objects into the ears to clean them
Symptoms
Ear pain may suddenly decrease right after your eardrum ruptures.
After the rupture, you may have:
- Drainage from the ear (drainage may be clear, pus, or bloody)
- Ear noise/buzzing (tinnitus)
- Earache or ear discomfort
- Hearing loss in the involved ear (hearing loss may not be total)
- Weakness of the face, or dizziness (in severe cases)
Exams and Tests
The health care provider will look in your ear with an instrument called an otoscope. Sometimes they will need to use a microscope for a better view. If your eardrum is ruptured, the provider will see an opening in it. The bones of the middle ear may also be visible.
Pus draining from the ear may make it harder for the provider to see the eardrum. If pus is present and blocking the view of the eardrum, the provider may need to suction the ear to clear the pus.
Audiology testing can measure how much hearing has been lost.
Treatment
You can take steps at home to treat ear pain.
- Put warm compresses on the ear to help relieve discomfort.
- Use medicines such as ibuprofen or acetaminophen to ease pain.
Keep the ear clean and dry while it is healing.
- Place cotton balls in the ear while showering or shampooing to prevent water from entering the ear.
- Avoid swimming or putting your head underneath the water.
Your provider may prescribe antibiotics (oral or ear drops) to prevent or treat an infection.
Repair of the eardrum might be needed for larger holes or ruptures or if the eardrum does not heal on its own. This can be done either in the office or under anesthesia.
Options may include:
- Patch the eardrum with a piece of the person's own tissue taken (called tympanoplasty). This procedure will usually take 30 minutes to 2 hours.
- Repair smaller holes in the eardrum by placing either gel or a special paper over the eardrum (called myringoplasty). This procedure will usually take 10 to 30 minutes.
Outlook (Prognosis)
The opening in the eardrum most often heals by itself within 2 months if it is a small hole.
Hearing loss will be short-term if the rupture heals completely.
Rarely, other problems may occur, such as:
- Long-term hearing loss
- Spread of infection to the bone behind the ear (mastoiditis)
- Long-term vertigo and dizziness
- Chronic ear infection or ear drainage
When to Contact a Medical Professional
If your pain and symptoms improve after your eardrum ruptures, you may wait until the next day to see your provider.
Contact your provider right away after your eardrum ruptures if you:
- Are very dizzy
- Have a fever, general ill feeling, or hearing loss
- Have very bad pain or a loud ringing in your ear
- Have an object in your ear that does not come out
- Have any symptoms that last longer than 2 months after treatment
Prevention
DO NOT insert objects into the ear canal, even to clean it. Objects stuck in the ear should only be removed by a provider. Have ear infections treated right away.
Related Information
Acoustic traumaEar barotrauma
Otitis
References
Pelton SI. Otitis externa, otitis media, and mastoiditis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 61.
Player B. Otitis media. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 680.
Shaikh N. Otitis media. In: Long SS, Prober CG, Fischer M, Kimberlin DW, eds. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 29.
BACK TO TOPReview Date: 5/2/2024
Reviewed By: Josef Shargorodsky, MD, MPH, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
