Melanoma of the eye
Malignant melanoma - choroid; Malignant melanoma - eye; Eye tumor; Ocular melanoma
Melanoma of the eye is cancer that occurs in various parts of the eye.
Images
I Would Like to Learn About:
Causes
Melanoma is a very aggressive type of cancer that can spread rapidly. It usually is a type of skin cancer.
Melanoma of the eye can affect several parts of the eye, including the:
- Choroid
- Ciliary body
- Conjunctiva
- Eyelid
- Iris
- Orbit
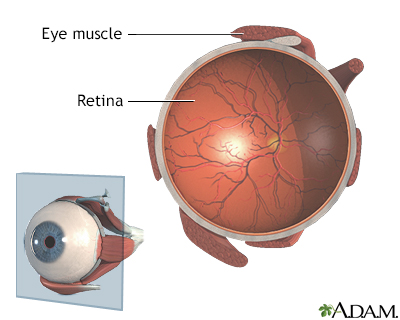
The choroid layer is the most likely site of melanoma in the eye. This is the layer of blood vessels and connective tissue between the white of the eye and retina (back of the eye).
The cancer may only be in the eye. Or, it may spread (metastasize) to another location in the body, most commonly the liver. Melanoma can also begin on the skin or other organs in the body and spread to the eye.
Melanoma is the most common type of eye tumor in adults. Even so, melanoma that starts in the eye is rare.
Too much exposure to sunlight is an important risk factor for melanoma. People who have fair skin and blue eyes are most affected.
Symptoms
Symptoms of melanoma of the eye may include any of the following:
- Bulging eyes
- Change in iris color
- Poor vision in one eye
- Red, painful eye
- Small defect on the iris or conjunctiva
In some cases, there may be no symptoms.
Exams and Tests
An eye examination with an ophthalmoscope may reveal a single round or oval lump (tumor) in the eye.
Tests that may be ordered include:
- Brain CT or MRI scan to look for spread (metastasis) to the brain
- Eye ultrasound
- Skin biopsy if there is an affected area on the skin
Treatment
Small melanomas may be treated with:
- Surgery
- Laser
- Radiation therapy (such as Gamma Knife, CyberKnife, brachytherapy)
Surgery to remove the eye (enucleation) may be needed.
Other treatments that may be used include:
- Chemotherapy, if the cancer has spread beyond the eye
- Immunotherapy, which uses medicines to help your immune system fight the melanoma
Support Groups
You can ease the stress of illness by joining a cancer support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
The outcome for melanoma of the eye depends on the size of the cancer when it is diagnosed. Most people survive at least 5 years from the time of diagnosis if the cancer has not spread outside the eye.
If the cancer has spread outside the eye, the chance of long-term survival is much lower.
Possible Complications
Problems that may develop due to melanoma of the eye include:
- Distortion or loss of vision
- Retinal detachment
- Spread of the tumor to other areas of the body
When to Contact a Medical Professional
Contact your health care provider for an appointment if you have symptoms of melanoma of the eye.
Prevention
The most important way to prevent melanoma of the eye is to protect the eyes from sunlight, especially between 10 a.m. and 4 p.m., when the sun's rays are most intense. Wear sunglasses that have ultraviolet protection.
A yearly eye exam is recommended.
Related Information
TumorChoroid
Melanoma
Retinal detachment
Proton therapy
References
Dalvin LA, Shields CL. Tumors of the uvea. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 8.2.
McCannel TA. Epidemiology of posterior uveal melanoma. In: Sadda SVR, Sarraf D, Freund KB, et al, eds. Ryan's Retina. 7th ed. Philadelphia, PA: Elsevier; 2023:chap 140.
National Cancer Institute website. Intraocular (uveal) melanoma treatment (PDQ) -- health professional version. www.cancer.gov/types/eye/hp/intraocular-melanoma-treatment-pdq. Updated May 12, 2023. Accessed September 12, 2023.
Shields CL, Shields JA. Overview of management of posterior uveal melanoma. In: Sadda SVR, Sarraf D, Freund KB, et al, eds. Ryan's Retina. 7th ed. Philadelphia, PA: Elsevier; 2023:chap 144.
BACK TO TOPReview Date: 8/28/2023
Reviewed By: Todd Gersten, MD, Hematology/Oncology, Florida Cancer Specialists & Research Institute, Wellington, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
