Ringworm of the scalp
Fungal infection - scalp; Tinea of the scalp; Tinea - capitis
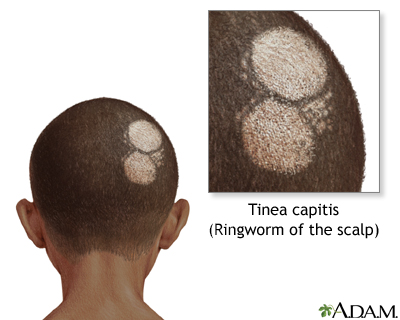
Ringworm of the scalp is a fungal infection that affects the scalp. It is also called tinea capitis.
Related ringworm infections may be found:
- In a man's beard
- In the groin (jock itch)
- Between the toes (athlete's foot)
- Other places on the skin
Images
I Would Like to Learn About:
Causes
Fungi are germs that can live on the dead tissue of the hair, nails, and outer skin layers. Ringworm of the scalp is caused by mold-like fungi called dermatophytes.
The fungi grow well in warm, moist areas. A tinea infection is more likely if you:
- Have minor skin or scalp injuries
- Do not bathe or wash your hair often
- Have wet skin for a long time (such as from sweating)
Ringworm can spread quickly. It most often affects children and goes away at puberty. However, it can occur at any age.
You can catch ringworm if you come into direct contact with an area of ringworm on someone else's body. You can also get it if you touch items such as combs, hats, or clothing that have been used by someone with ringworm. The infection can also be spread by pets, particularly cats.
Symptoms
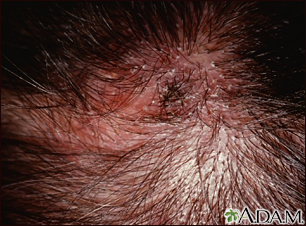
Ringworm may involve part or all of the scalp. The affected areas:
- Are bald with small black dots due to hair that has broken off
- Have round, scaly areas of skin that are red or swollen (inflamed)
- May have pus-filled sores called kerions
- May be very itchy
You may have a low-grade fever of around 100°F to 101°F (37.8°C to 38.3°C) or swollen lymph nodes in the neck.
Ringworm may cause permanent hair loss and lasting scars.
Exams and Tests
Your health care provider will look at your scalp for signs of ringworm.
You may also need the following tests:
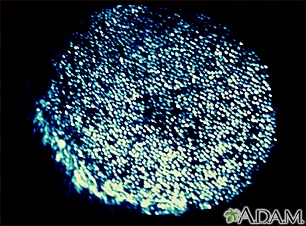
- Examination of a skin scraping from the rash under a microscope using a special test
- Skin culture for fungus
- Skin biopsy (rarely needed)
Treatment
Your provider will prescribe medicine you take by mouth to treat ringworm on the scalp. You will need to take the medicine for 4 to 8 weeks.
Steps you can do at home include:
- Keeping your scalp clean.
- Washing with a medicated shampoo, such as one that contains ketoconazole or selenium sulfide. Shampooing may slow or stop the spread of infection, but it does not get rid of ringworm.
Other family members and pets should be examined and treated, if necessary.
- Other children in the home may want to use the shampoo 2 to 3 times a week for about 6 weeks.
- Adults only need to wash with the shampoo if they have signs of tinea capitis or ringworm.
Once the shampoo has been started:
- Wash towels in hot, soapy water and dry them using the hottest heat recommended on the care label. This should be done each time the towels are used by someone who is infected.
- Soak combs and brushes for 1 hour a day in a mixture of 1 part bleach to 10 parts water. Do this for 3 days in a row.
No one in the home should share combs, hairbrushes, hats, towels, pillowcases, or helmets with other people.
Outlook (Prognosis)
It may be hard to get rid of ringworm. Also, the problem may come back after it is treated. In many cases, it gets better on its own after puberty.
When to Contact a Medical Professional
Contact your provider if you have symptoms of ringworm of the scalp and home care is not enough to get rid of the condition.
Related Information
RingwormReferences
Dinulos JGH. Superficial fungal infections. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 13.
Hay RJ. Dermatophytosis (ringworm) and other superficial mycoses. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 266.
Patterson JW. Mycoses and algal infections. In: Patterson JW, ed. Weedon's Skin Pathology. 5th ed. Philadelphia, PA: Elsevier Limited; 2021:chap 26.
BACK TO TOPReview Date: 10/13/2024
Reviewed By: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
