Trigeminal neuralgia
Tic douloureux; Cranial neuralgia; Facial pain - trigeminal; Facial neuralgia; Trifacial neuralgia; Chronic pain - trigeminal; Microvascular decompression - trigeminal
Trigeminal neuralgia (TN) is a nerve disorder. It causes a stabbing or electric shock-like pain in parts of the face.
Images
I Would Like to Learn About:
Causes
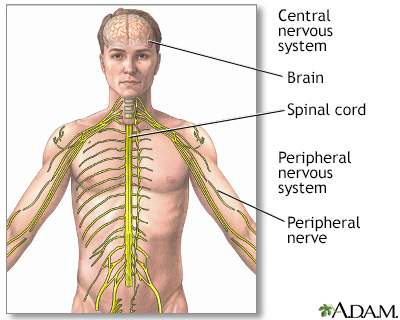
The pain of TN comes from the trigeminal nerve. This nerve carries the sensations of touch and pain from the face, eyes, sinuses, and mouth to the brain.
TN may be caused by:
- Multiple sclerosis (MS) or other diseases that damage the protective covering myelin of the nerves
- Pressure on the trigeminal nerve from a swollen blood vessel or tumor
- Injury to the trigeminal nerve, such as from trauma to the face or from oral or sinus surgery
Often, no exact cause is found. TN usually affects adults above age 50 years, but it can occur at any age. Women are affected more often than men. When TN affects people younger than 40, it is often due to MS or a tumor.
Symptoms
Symptoms may include any of the following:
- Very painful, sharp electric-like spasms that are usually brief. The spasms may occur close together such that it feels like they last from several seconds to minutes. Pain can become constant.
- Pain is usually only on one side of the face, often around the eye, cheek, and lower part of the face.
- There is usually no loss of sensation or movement of the affected part of the face.
- Pain may be triggered by touch or sounds.
Painful attacks of TN can be triggered by common, everyday activities, such as:
- Talking
- Smiling
- Brushing teeth
- Chewing
- Drinking
- Eating
- Exposure to hot or cold temperature
- Touching the face
- Shaving
- Wind
- Applying make-up
The right side of the face is mostly affected. In some cases, TN goes away on its own.
Exams and Tests
A brain and nervous system (neurologic) exam is often normal. Tests that are done to look for the cause may include:
- Complete blood count
- Erythrocyte sedimentation rate (ESR)
- MRI of the head
- MRA (angiography) of brain or CTA
- Eye examination (to rule out intraocular disease)
- Spinal tap (lumbar puncture)
- CT scan of head (who cannot undergo MRI)
- Trigeminal reflex testing (in rare cases)
Treatment
Your primary care provider, a neurologist, or a pain specialist may be involved in your care.
Certain medicines sometimes help reduce pain and the rate of attacks. These medicines include:
- Anti-seizure medicines, such as carbamazepine
- Muscle relaxants, such as baclofen
- Tricyclic antidepressants
If you are found to have MS as a cause of TN, your health care provider will discuss medicines that can treat the underlying MS.
Short-term pain relief occurs through surgery, but is associated with risk of complications. One surgery is called microvascular decompression (MVD) or the Jannetta procedure. During surgery, a sponge-like material is placed between the nerve and the blood vessel that is pressing on the nerve.
Trigeminal nerve block (injection) with local anesthetic and steroid is an excellent treatment option to rapidly relieve pain while waiting for medicines to take effect.
Other techniques involve destroying or cutting parts of the trigeminal nerve root. Methods used include:
- Radiofrequency ablation (uses high-frequency heat)
- Injection of glycerol or alcohol
- Balloon microcompression
- Radiosurgery (uses high power energy)
If a tumor is the cause of TN, surgery is done to remove it.
Outlook (Prognosis)
How well you do depends on the cause of the problem. If there is no disease causing the problem, treatment can provide some relief.
In some people, the pain becomes constant and severe.
Possible Complications
Complications may include:
- Side effects of medicines used to treat TN
- Problems caused by procedures, such as loss of feeling in the treated area
- Weight loss from not eating to avoid triggering pain
- Avoiding other people if talking triggers pain
- Depression, suicide
- High levels of anxiety during acute attacks
When to Contact a Medical Professional
Contact your provider if you have symptoms of TN, or your TN symptoms get worse.
Related Information
Face painReferences
Bendtsen L, Zakrzewska JM, Heinskou TB, et al. Advances in diagnosis, classification, pathophysiology, and management of trigeminal neuralgia. Lancet Neurol. 2020;19(9):784-796. PMID: 32822636 pubmed.ncbi.nlm.nih.gov/32822636/.
Dinakar P. Pain management. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 52.
Smith AG, Shy ME. Peripheral neuropathies. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 388.
Waldman SD. Trigeminal neuralgia. In: Waldman SD, ed. Atlas of Common Pain Syndromes. 5th ed. Philadelphia, PA: Elsevier; 2024:chap 10.
Westmark NLW. Facial pain and neuromuscular diseases. In: Neville BW, Damm DD, Allen CM, Chi AC, eds. Oral and Maxillofacial Pathology. 5th ed. St Louis, MO: Elsevier; 2024:chap 18.
BACK TO TOPReview Date: 6/13/2024
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
