Sinusitis
Acute sinusitis; Sinus infection; Sinusitis - acute; Sinusitis - chronic; Rhinosinusitis
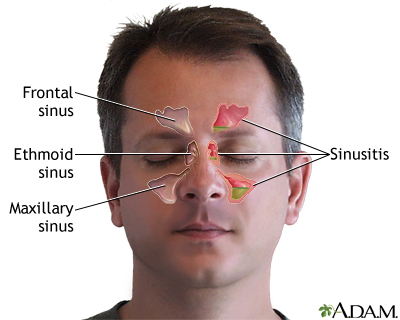
Sinusitis is present when the tissue lining the sinuses become swollen or inflamed. It occurs as the result of an inflammatory reaction or an infection from a virus, bacteria, or fungus.
Images
I Would Like to Learn About:
Causes
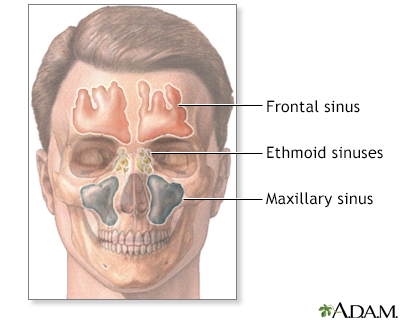
The sinuses are air-filled spaces in the skull. They are located behind the forehead, nasal bones, cheeks, and eyes. Most of the time, mucus is able to drain out and air is able to flow through the sinuses.
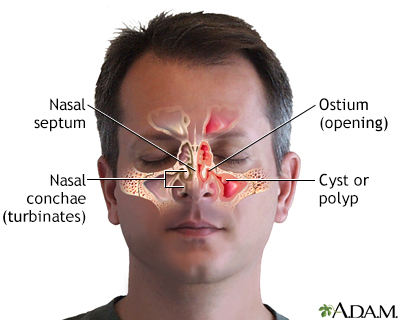
When the sinus openings become blocked or too much mucus builds up, bacteria and other germs can grow more easily.
Sinusitis can occur from one of these conditions:
- Small hairs (cilia) in the sinuses fail to properly move mucus out. This may be due to some medical conditions.
- Colds and allergies may cause too much mucus to be made or the associated inflammation may block the opening of the sinuses.
- A deviated nasal septum, nasal bone spur, or nasal polyps may block the opening of the sinuses.
- Chronic infection can cause mucosal swelling and inflammation.
There are three types of sinusitis:
- Acute sinusitis is when symptoms are present for 4 weeks or less. It is caused by viruses or bacteria growing in the sinuses.
- Chronic sinusitis is when the symptoms and swelling of the sinuses is present for longer than 3 months. It may be caused by bacteria or a fungus.
- Subacute sinusitis is when the symptoms and swelling is present from 1 to 3 months.
The following may increase the risk that an adult or child will develop sinusitis:
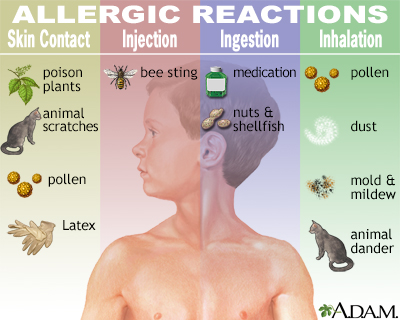
- Allergic rhinitis or hay fever
- Cystic fibrosis
- Going to day care
- Diseases that prevent the cilia from working properly
- Changes in altitude (flying or scuba diving)
- Large adenoids
- Smoking
- Weakened immune system from HIV or chemotherapy
- Abnormal sinus structures
Symptoms
The symptoms of acute sinusitis in adults very often follow a cold that does not get better or that gets worse after 7 to 10 days. Symptoms include:
- Bad breath or loss of smell
- Cough, often worse at night
- Fatigue and general feeling of being ill
- Fever
- Headache
- Pressure-like pain, pain behind the eyes, toothache, or tenderness of the face
- Nasal stuffiness and discharge
- Sore throat and postnasal drip
Symptoms of chronic sinusitis are the same as those of acute sinusitis. However, the symptoms tend to be milder and last longer than 12 weeks.
Symptoms of sinusitis in children include:
- Cold or respiratory illness that has been getting better and then begins to get worse
- High fever, along with a darkened nasal discharge, that lasts for at least 3 days
- Nasal discharge, with or without a cough, that has been present for more than 10 days and is not improving
Exams and Tests
The health care provider will examine you or your child for sinusitis by:
- Looking in the nose for signs of polyps
- Shining a light against the sinus (transillumination) for signs of inflammation
- Tapping over a sinus area to find tenderness that may be due to infection
The provider may view the sinuses through a fiberoptic scope (called nasal endoscopy or rhinoscopy) to diagnose sinusitis. This is often done by doctors who specialize in ear, nose, and throat problems (ENTs).
Imaging tests that may be used to decide on treatment are:
- A CT scan of the sinuses to help diagnose sinusitis or view the bones and tissues of the sinuses more closely
- An MRI of the sinuses if there might be a tumor or fungal infection
Most of the time, regular x-rays of the sinuses do not diagnose sinusitis well.
If you or your child has sinusitis that does not go away or keeps returning, other tests may include:
- Allergy testing
- Blood tests for HIV or other tests for poor immune function
- Ciliary function test
- Nasal culture
- Nasal cytology
- Sweat chloride tests for cystic fibrosis
Treatment
SELF-CARE
Try the following steps to reduce stuffiness in your sinuses:
- Apply a warm, moist washcloth to your face several times a day.
- Drink plenty of fluids to thin the mucus.
- Inhale steam 2 to 4 times per day (for example, while sitting in the bathroom with the shower running).
- Spray with nasal saline several times per day.
- Use a humidifier.
- Use a Neti pot or saline squeeze bottle to flush the sinuses.
Be careful with use of over-the-counter spray nasal decongestants such as oxymetazoline (Afrin) or phenylephrine (Neosynephrine). They may help at first, but using them for more than 3 to 5 days can make nasal stuffiness worse and lead to dependence.
To help ease sinus pain or pressure:
- Avoid flying when you are congested.
- Avoid temperature extremes, sudden changes in temperature, and bending forward with your head down.
- Try acetaminophen, ibuprofen, or naproxen.
MEDICINE AND OTHER TREATMENTS
Most of the time, antibiotics are not needed for acute sinusitis. Most of these infections go away on their own. Even when antibiotics do help, they may only slightly reduce the time it takes for the infection to go away. Antibiotics are more likely to be prescribed sooner for:
- Children with nasal discharge, possibly with a cough, that is not getting better after 2 to 3 weeks
- Fever higher than 102.2°F (39°C)
- Headache or pain in the face
- Severe swelling around the eyes
Acute sinusitis should be treated for 5 to 10 days. Chronic sinusitis should be treated for 3 to 4 weeks.
At some point, your provider will consider:
- Other prescription medicines
- More testing
- Referral to an ear, nose, and throat or allergy specialist
Other treatments for sinusitis include:
- Allergy shots (immunotherapy) to help prevent the disease from returning
- Avoiding allergy triggers
- Nasal corticosteroid sprays and antihistamines to decrease swelling, especially if there are nasal polyps or allergies
- Oral corticosteroids
Surgery to enlarge the sinus opening and drain the sinuses may also be needed. You may consider this procedure if:
- Your symptoms do not go away after 3 months of treatment.
- You have more than 2 or 3 episodes of acute sinusitis each year.
Most fungal sinus infections need surgery. Surgery to repair a deviated septum or nasal polyps may prevent the condition from returning.
Outlook (Prognosis)
Most sinus infections can be cured with self-care measures and medical treatment. If you are having repeated attacks, you should be checked for causes such as nasal polyps or other problems, such as allergies.
Possible Complications
Although very rare, complications may include:
- Abscess
- Bone infection (osteomyelitis)
- Meningitis
- Skin infection around the eye (orbital cellulitis)
When to Contact a Medical Professional
Contact your provider if:
- Your symptoms last longer than 10 to 14 days or you have a cold that gets worse after 7 days.
- You have a severe headache that is not relieved by over-the-counter pain medicine.
- You have a fever.
- You still have symptoms after taking all of your antibiotics properly.
- You have any changes in your vision during a sinus infection.
A green or yellow discharge does not mean that you definitely have a sinus infection or need antibiotics. Many people with this symptom recover fully without taking antibiotics.
Prevention
The best way to prevent sinusitis is to avoid colds and flu or treat problems quickly.
- Control your allergies if you have them.
- Get an influenza vaccine each year.
- Reduce stress.
- Wash your hands often, particularly after shaking hands with others.
Other tips for preventing sinusitis:
- Avoid smoke and pollutants.
- Drink plenty of fluids to increase moisture in your body.
- Take decongestants during an upper respiratory infection.
- Treat allergies quickly and appropriately.
- Use a humidifier to increase moisture in your nose and sinuses.
Related Information
Common coldCystic fibrosis
References
DeMuri GP, Wald ER. Sinusitis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 62.
Murr AH, Pletcher SD. Approach to the patient with nose, sinus, and ear disorders. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 394.
Pappas DE, Boggs SR. Sinusitis. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 429.
Rosenfeld RM, Piccirillo JF, Chandrasekhar SS, et al. Clinical practice guideline (update): adult sinusitis. Otolaryngol Head Neck Surg. 2015;152(2 Suppl):S1-S39. PMID: 25832968 pubmed.ncbi.nlm.nih.gov/25832968/.
BACK TO TOPReview Date: 5/2/2024
Reviewed By: Josef Shargorodsky, MD, MPH, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
