Leydig cell testicular tumor
Tumor - Leydig cell; Testicular tumor - Leydig
A Leydig cell tumor is a tumor of the testicle. It develops from Leydig cells. These are the cells in the testicles that release the male hormone, testosterone.
Images
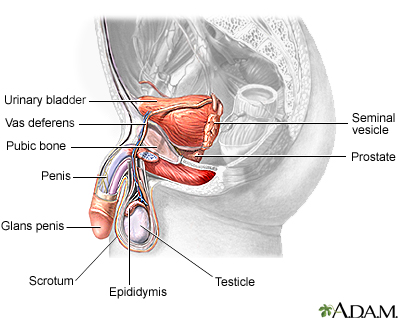
Causes
The cause of this tumor is unknown. There are no known risk factors for this tumor. Unlike germ cell tumors of the testicles, this tumor does not seem to be linked to undescended testes.
Leydig cell tumors make up a very small number of all testicular tumors. They are most often found in men between 30 and 60 years of age. This tumor is not common in children before puberty, but it may cause early puberty.
Symptoms
There may be no symptoms.
When symptoms do occur, they can include:
- Discomfort or pain in the testicle
- Enlargement of a testicle or change in the way it feels
- Excess growth of breast tissue (gynecomastia) -- however, this can occur normally in adolescent boys who do not have testicular cancer
- Heaviness in the scrotum
- Lump or swelling in either testicle
- Pain in the lower abdomen or back
- Not able to father children (infertility)
Symptoms in other parts of the body, such as the lungs, abdomen, pelvis, back, or brain may also occur if the cancer has spread.
Exams and Tests
A physical examination typically reveals a firm lump in one of the testicles. When your health care provider holds a flashlight up to your scrotum, the light does not pass through the lump. This test is called transillumination.
Other tests include:
- Blood tests for tumor markers: alpha fetoprotein (AFP), human chorionic gonadotropin (beta HCG), and lactate dehydrogenase (LDH)
- CT scan of the chest, abdomen and pelvis to check if the cancer has spread
- Ultrasound of the scrotum
An examination of the tissue is usually done after the entire testicle is surgically removed (orchiectomy).
Treatment
Treatment of a Leydig cell tumor depends on its stage.
- Stage I cancer has not spread beyond the testicle.
- Stage II cancer has spread to lymph nodes in the abdomen.
- Stage III cancer has spread beyond the lymph nodes (possibly as far as the liver, lungs, or brain).
Surgery is done to remove the testicle (orchiectomy). Nearby lymph nodes may also be removed (lymphadenectomy).
Chemotherapy may be used to treat this tumor. As Leydig cell tumors are rare, these treatments have not been studied as much as treatments for other, more common testicular cancers.
Support Groups
Joining a support group where members share common experiences and problems can often help ease the stress of illness.
Outlook (Prognosis)
Testicular cancer is one of the most treatable and curable cancers. The outlook is worse if the tumor is not found early.
Possible Complications
The cancer may spread to other parts of the body. The most common sites include the:
- Abdomen
- Lungs
- Retroperitoneal area (the area near the kidneys behind the other organs in the belly area)
- Spine
Complications of surgery can include:
- Bleeding and infection
- Infertility (if both testicles are removed)
If you are of childbearing age, ask your provider about methods to save your sperm for use at a later date.
When to Contact a Medical Professional
Contact your provider if you have symptoms of testicular cancer.
Prevention
Performing testicular self-examination (TSE) each month may help detect testicular cancer at an early stage, before it spreads. Finding testicular cancer early is important for successful treatment and survival.
Related Information
TumorTestosterone
References
Friedlander TW, Small E. Testicular cancer. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 83.
National Cancer Institute website. Testicular cancer treatment (PDQ) – health professional version. www.cancer.gov/types/testicular/hp/testicular-treatment-pdq. Updated March 15, 2024. Accessed July 9, 2024.
Stephenson AJ, Gilligan TD. Neoplasms of the testis. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 76.
BACK TO TOPReview Date: 6/17/2024
Reviewed By: Todd Gersten, MD, Hematology/Oncology, Florida Cancer Specialists & Research Institute, Wellington, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
