Pancreatic neuroendocrine tumors
Cancer - pancreas; Cancer - pancreatic; Pancreatic cancer; Islet cell tumors; Islet of Langerhans tumor; Neuroendocrine tumors; Peptic ulcer - islet cell tumor; Hypoglycemia - islet cell tumor; Zollinger-Ellison syndrome; Verner-Morrison syndrome; Gastrinoma; Insulinoma; VIPoma; Somatostatinoma; Glucagonoma; Pancreatic islet cell tumor
Pancreatic neuroendocrine tumors (NET) are rare tumors of the pancreas that start from a type of cell called the islet cell.
Images
I Would Like to Learn About:
Causes
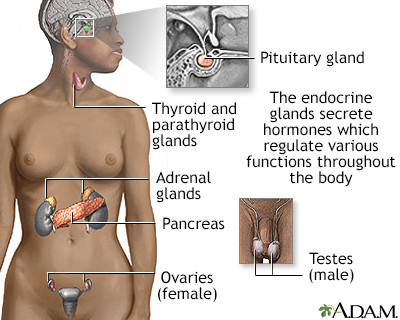
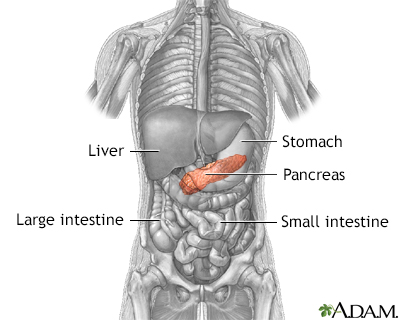
In the healthy pancreas, cells called islet cells produce hormones that regulate several bodily functions. These include blood sugar level and the production of stomach acid.
Tumors that arise from islet cells of the pancreas can also produce a variety of hormones, which can lead to specific symptoms.
Pancreatic NETs can be noncancerous (benign) or cancerous (malignant).
NETs include:
- Gastrinoma (Zollinger-Ellison syndrome)
- Glucagonoma
- Insulinoma
- Somatostatinoma
- VIPoma (Verner-Morrison syndrome)
A family history of multiple endocrine neoplasia, type I (MEN I) is a risk factor for the development of NETs.
Symptoms
Symptoms depend on which hormone is made by the tumor.
For example, insulinomas produce insulin, which lowers blood sugar level. Symptoms may include:
- Feeling tired or weak
- Shaking or sweating
- Headache
- Hunger
- Nervousness, anxiety, or feeling irritable
- Unclear thinking or feeling uneasy
- Double or blurry vision
- Fast or pounding heartbeat
If your blood sugar level gets too low, you may faint, have a seizure, or even go into a coma.
Gastrinomas make the hormone gastrin, which tells the body to make stomach acid. Symptoms may include:
- Abdominal pain
- Diarrhea
- Ulcers in the stomach and small bowel
- Vomiting blood (occasionally)
Glucagonomas make the hormone glucagon, which helps the body raise blood sugar level. Symptoms can include:
- Diabetes
- Red, blistery rash in the groin or buttocks
- Weight loss
- Frequent urination and thirst
Somatostatinomas make the hormone somatostatin. Symptoms may include:
- High blood sugar
- Gallstones
- Yellowish appearance to skin, and eyes
- Weight loss
- Diarrhea with foul smelling stools
VIPomas make the hormone vasoactive intestinal peptide (VIP) which is involved in maintaining the balance of sodium, potassium and other minerals in the GI tract. VIPomas may cause:
- Severe diarrhea that may lead to dehydration
- Low blood potassium levels, and high calcium levels
- Abdominal cramps
- Weight loss
Exams and Tests
Your health care provider will take your medical history and perform a physical exam.
Blood tests may vary, depending upon the symptoms, but may include:
- Fasting glucose level
- Gastrin level
- Glucose tolerance test
- Secretin stimulation test for pancreas
- Blood glucagon level
- Blood insulin C-peptide level
- Blood insulin level
- Fasting serum somatostatin level
- Serum vasoactive intestinal peptide (VIP) level
Imaging tests may be done:
A blood sample may also be taken from a vein in the pancreas for testing.
Sometimes, surgery is needed to diagnose and treat this condition. During this procedure, the surgeon examines the pancreas by hand and with ultrasound.
Treatment
Treatment depends on the type of tumor and if it is cancerous.
Cancerous tumors can grow quickly and spread to other organs. They may not be treatable. Tumors are often removed with surgery, if possible.
If cancer cells spread to the liver, a part of the liver may also be removed, if possible. If the cancer is widespread, chemotherapy may be used to try to shrink the tumors.
If the abnormal production of hormones is causing symptoms, you may receive medicines to counteract their effects. For example, with gastrinomas, the overproduction of gastrin leads to too much acid in the stomach. Medicines that block stomach acid release can reduce symptoms.
Support Groups
You can ease the stress of illness by joining a cancer support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
You may be cured if the tumors are surgically removed before they have spread to other organs. If tumors are cancerous, chemotherapy may be used, but it usually cannot cure people.
Life-threatening problems (such as very low blood sugar) can occur due to excess hormone production, or if the cancer spreads throughout the body.
Possible Complications
Complications of these tumors include:
- Diabetes
- Hormone crises (if the tumor releases certain types of hormones)
- Severe low blood sugar (from insulinomas)
- Severe ulcers in the stomach and small intestine (from gastrinomas)
- Spread of the tumor to the liver
When to Contact a Medical Professional
Contact your provider if you develop symptoms of these tumors, especially if you have a family history of MEN I.
Prevention
There is no known prevention for these tumors.
Related Information
TumorBenign
Zollinger-Ellison syndrome
Endocrine glands
Multiple endocrine neoplasia (MEN) I
References
Khreiss MR, Riall TS. Pancreatic neuroendocrine tumors of the pancreas excluding gastrinoma. In: Cameron JL, Cameron AM, eds. Current Surgical Therapy. 14th ed. Philadelphia, PA: Elsevier; 2023:632-638.
National Cancer Institute website. Pancreatic neuroendocrine tumors (islet cell tumors) treatment (PDQ) - health professional version. www.cancer.gov/types/pancreatic/hp/pnet-treatment-pdq. Updated August 19, 2022. Accessed May 6, 2024.
National Comprehensive Cancer Network website. NCCN clinical practice guidelines in oncology (NCCN guidelines). Neuroendocrine and adrenal tumors. Version 1. 2023. www.nccn.org/professionals/physician_gls/pdf/neuroendocrine.pdf. Updated August 2, 2023. Accessed May 6, 2024.
National Comprehensive Cancer Network website. NCCN guidelines for patients. Neuroendocrine tumors. 2022. www.nccn.org/patients/guidelines/content/PDF/neuroendocrine-patient.pdf. Accessed May 6, 2024.
BACK TO TOPReview Date: 3/31/2024
Reviewed By: Todd Gersten, MD, Hematology/Oncology, Florida Cancer Specialists & Research Institute, Wellington, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
