Hypercalcemia
Calcium - elevated; High calcium level; Hyperparathyroidism - hypercalcemia
Hypercalcemia means you have too much calcium in your blood.
Images
I Would Like to Learn About:
Causes
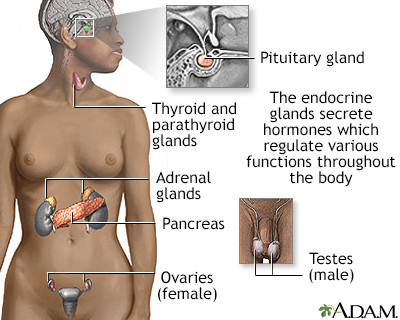
Parathyroid hormone (PTH) and Vitamin D help manage calcium balance in the body.
- PTH is made by the parathyroid glands. These are four small glands located in the neck behind the thyroid gland.
- Vitamin D is obtained when the skin is exposed to sunlight, and from food sources or supplements.
The most common cause of high calcium blood level is excess PTH released by the parathyroid glands. This excess occurs due to:
- An enlargement of one or more of the parathyroid glands.
- A growth on one of the glands. Most of the time, these growths are benign (not a cancer).
Calcium blood level may also be high if your body is low on fluids or water.
Other conditions can also cause hypercalcemia:
- Certain kinds of cancers, such as lung and breast cancer, or cancer that has spread to your organs.
- Too much vitamin D in your blood (hypervitaminosis D).
- Being immobile in bed for many days or weeks (mostly in children).
- Too much calcium in your diet. This is called milk-alkali syndrome. It most often occurs when a person is taking more than 2000 milligrams of calcium bicarbonate supplements a day along with high doses of Vitamin D.
- Overactive thyroid gland.
- Chronic kidney disease or kidney failure.
- Medicines such as thiazide diuretics (water pills) and lithium.
- Some infections or health problems such as, Paget disease, tuberculosis and sarcoidosis.
- An inherited condition that affects the body's ability to manage calcium.
Men and women of all ages can have a high blood calcium level. However, it is most common in women over age 50 (after menopause). In most cases, this is due to an overactive parathyroid gland.
Symptoms
The condition is most often diagnosed at an early stage using routine blood tests. Most people have no symptoms.
Symptoms due to high calcium level may vary, depending on the cause and how long the problem has been present. They may include:
- Digestive symptoms, such as nausea or vomiting, poor appetite, or constipation
- Increased thirst or more frequent urination, due to changes in the kidneys
- Muscle weakness or twitches
- Changes in how your brain works, such as feeling tired or fatigued or confused
- Bone pain and fragile bones that break more easily
Exams and Tests
An accurate diagnosis is needed when someone has hypercalcemia. People with kidney stones should have tests to evaluate for hypercalcemia.
- Serum calcium
- Serum PTH
- Serum PTHrP (PTH-related protein)
- Serum vitamin D level
- Urine calcium
Treatment
Treatment is aimed at the cause of hypercalcemia whenever possible. People with primary hyperparathyroidism (PHPT) may need surgery to remove the abnormal parathyroid gland. This will cure the hypercalcemia.
Severe hypercalcemia that causes symptoms and requires a hospital stay may be treated with the following:
- Fluids through a vein -- This is the most important therapy.
- Calcitonin.
- Dialysis, if kidney damage is involved.
- Diuretic medicine, such as furosemide.
- Drugs that stop bone breakdown and absorption by the body (bisphosphonates).
- Glucocorticoids (steroids).
Outlook (Prognosis)
How well you do depends on the cause of your high calcium level. The outlook is good for people with mild hyperparathyroidism or hypercalcemia that have a treatable cause. Most of the time, there are no complications.
People with hypercalcemia due to conditions such as cancer or sarcoidosis may not do well. This is most often because of the disease itself, rather than the high calcium level.
Possible Complications
GASTROINTESTINAL
- Pancreatitis
- Peptic ulcer disease
KIDNEY
- Calcium deposits in the kidney (nephrocalcinosis) that cause poor kidney function
- Dehydration
- High blood pressure
- Kidney failure
- Kidney stones
PSYCHOLOGICAL
- Depression
- Difficulty concentrating or thinking
SKELETAL
- Bone cysts
- Fractures
- Osteoporosis
These complications of long-term hypercalcemia are uncommon today in many countries.
When to Contact a Medical Professional
Contact your health care provider if you have:
- Family history of hypercalcemia
- Family history of hyperparathyroidism
- Symptoms of hypercalcemia
Prevention
Most causes of hypercalcemia cannot be prevented. Anyone with symptoms of hypercalcemia should have their blood calcium level checked.
Talk to your provider about the correct dose if you are taking calcium and vitamin D supplements.
Related Information
Acute kidney failureHyperthyroidism
Broken bone
Osteoporosis
Nephrocalcinosis
Kidney stones
Dehydration
Peptic ulcer
High blood pressure in adults - hypertension
Parathyroid cancer
Hypercalcemia - discharge
References
Coleman RE, Brown J, Holen I. Bone metastases. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 56.
Reid LM, Kamani D, Randolf GW. Management of parathyroid disorders. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 123.
Thakker RV. The parathyroid glands, hypercalcemia, and hypocalcemia. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 227.
BACK TO TOPReview Date: 2/28/2024
Reviewed By: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
