Snake bites
Bites - snakes; Venomous snake bites
Snake bites occur when a snake bites the skin. They are medical emergencies if the snake is venomous.
Venomous animals account for a large number of deaths and injuries worldwide. Snakes alone are estimated to inflict 2.5 million venomous bites each year, resulting in about 150,000 deaths. The actual number may be much larger. Southeast Asia, India, Brazil, and areas of Africa have the most deaths due to snakebite.
Images
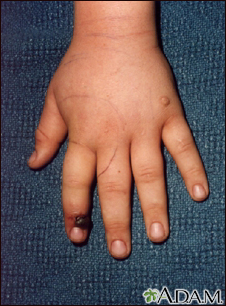
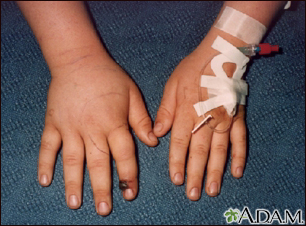
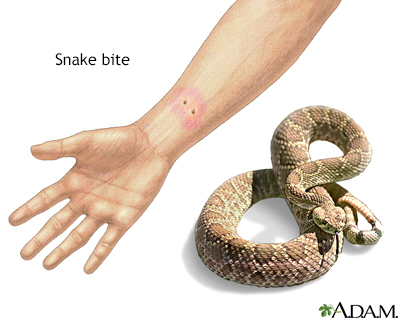
Presentation


Considerations
Snake bites can be deadly if not treated quickly. Because of their smaller body size, children are at higher risk for death or serious complications due to snake bites.
The right antivenom can save a person's life. Getting to an emergency room as quickly as possible is very important. If properly treated, many snake bites will not have serious effects.
Even the bite of a non-venomous snake can sometimes cause significant injury, particularly to children.
Causes
Most species of snake are harmless and their bites are not life threatening.
Venomous snake bites include bites by any of the following:
- Cobra
- Copperhead
- Coral snake
- Cottonmouth (water moccasin)
- Rattlesnake
- Various snakes found at zoos
Most snakes will avoid people if possible, but all snakes will bite as a last resort when threatened or surprised. If you are bitten by any snake, consider it a serious event.
Symptoms
Symptoms depend on the type of snake, but may include:
- Bleeding from wound
- Blurred vision
- Burning of the skin
- Seizures (convulsions)
- Diarrhea
- Dizziness
- Excessive sweating
- Fainting
- Fang marks in the skin
- Fever
- Increased thirst
- Loss of muscle coordination
- Nausea and vomiting
- Numbness and tingling
- Rapid pulse
- Tissue death
- Severe pain
- Skin discoloration
- Swelling at the site of the bite
- Weakness
Rattlesnake bites are painful when they occur. Symptoms usually begin right away and may include:
- Bleeding
- Breathing difficulty
- Blurred vision
- Eyelid drooping
- Low blood pressure
- Nausea and vomiting
- Numbness
- Pain at site of bite
- Paralysis
- Rapid pulse
- Skin color changes
- Swelling
- Tingling
- Tissue damage
- Thirst
- Tiredness
- Weakness
- Weak pulse
Cottonmouth and copperhead bites are painful right when they occur. Symptoms, which usually begin right away, may include:
- Bleeding
- Breathing difficulty
- Low blood pressure
- Nausea and vomiting
- Numbness and tingling
- Pain at site of bite
- Shock
- Skin color changes
- Swelling
- Thirst
- Tiredness
- Tissue damage
- Weakness
- Weak pulse
Coral snake bites may be painless at first. Major symptoms may not develop for hours. Do not make the mistake of thinking you will be fine if the bite area looks good and you are not in a lot of pain. Untreated coral snake bites can be deadly. Symptoms may include:
- Blurred vision
- Breathing difficulty
- Convulsions
- Drowsiness
- Eyelid drooping
- Headache
- Low blood pressure
- Mouth watering (excessive salivation)
- Nausea and vomiting
- Numbness
- Pain and swelling at site of bite
- Paralysis
- Shock
- Slurred speech
- Swallowing difficulty
- Swelling of tongue and throat
- Weakness
- Skin color changes
- Skin tissue damage
- Stomach or abdominal pain
- Weak pulse
First Aid
Follow these steps to provide first aid:
- Keep the person calm. Reassure them that bites can be effectively treated in an emergency room. Restrict movement, and keep the affected area at heart level if bitten by a pit viper (rattlesnake, copperhead, cottonmouth) in North America, or below heart level if bitten by a coral snake, cobra, or exotic snake, to reduce the flow of venom.
- Remove any rings or constricting items of clothing, because the affected area may swell. Create a loose splint to help restrict movement of the area. Loosely splint and/or sling the affected area. Do not use a tourniquet.
- If the area of the bite begins to swell and change color, the snake was probably venomous.
- Monitor the person's vital signs -- temperature, pulse, rate of breathing, and blood pressure -- if possible. If there are signs of shock (such as paleness), lay the person flat, raise the feet about a foot (30 centimeters), and cover the person with a blanket.
- Get medical help right away.
- If it is safe to do so, take a picture of the snake from a safe distance, or quickly make note of the color, shape, and size of the snake. This may help with treatment of the bite. Do not waste time hunting for the snake, and do not trap it or pick it up. If the snake is dead, be careful of the head -- a snake can actually bite (from a reflex) for several hours after it's dead.
Do Not
Follow these precautions:
- Do not pick up the snake or try to trap it.
- Do not wait for symptoms to appear if bitten. Seek immediate medical attention.
- Do not allow the person to become over-exerted. If necessary, carry the person to safety.
- Do not apply a tourniquet.
- Do not apply cold compresses to a snake bite.
- Do not apply ice or soak the wound in water.
- Do not cut into a snake bite with a knife or razor.
- Do not try to suck out the venom by mouth.
- Do not give the person stimulants or pain medicines unless your health care provider tells you to do so.
- Do not give the person anything by mouth.
- Do not raise the site of the bite above the level of the person's heart.
When to Contact a Medical Professional
Call 911 or the local emergency number if someone has been bitten by a snake. If possible, call ahead to the emergency room so that antivenom can be ready when the person arrives.
Your local poison control center can be reached directly by calling the national toll-free Poison Help hotline (1-800-222-1222) from anywhere in the United States. This national hotline number will let you talk to experts in poisoning. They will give you further instructions.
This is a free and confidential service. All local poison control centers in the United States use this national number. You should call if you have any questions about poisoning or poison prevention. It does NOT need to be an emergency. You can call for any reason, 24 hours a day, 7 days a week.
Prevention
To prevent snake bites:
- Avoid areas where snakes may be hiding, such as under rocks and logs.
- Even though most snakes are not venomous, avoid picking up or playing with any snake unless you have been properly trained.
- Don't provoke a snake. That is when many serious snake bites occur.
- Tap ahead of you with a walking stick before entering an area where you can't see your feet. Snakes will try to avoid you if given enough warning.
- When hiking in an area known to have snakes, wear long pants and boots if possible.
References
Centers for Disease Control and Prevention website. Venomous Snakes at Work. www.cdc.gov/niosh/outdoor-workers/about/venomous-snakes.html. Updated August 28, 2024. Accessed September 26, 2024.
Curtis AM, Erickson TB. Venomous animal injuries. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 53.
Seifert SA, Dart RC, White J. Envenomation, bites, and stings. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 98.
Tibballs J. Envenomation. In: Bersten AD, Handy JM, eds. Oh's Intensive Care Manual. 8th ed. Philadelphia, PA: Elsevier; 2019:chap 86.
BACK TO TOPReview Date: 11/2/2023
Reviewed By: Jesse Borke, MD, CPE, FAAEM, FACEP, Attending Physician at Kaiser Permanente, Orange County, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. Editorial update 09/26/2024.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
