Diabetes and exercise
Exercise - diabetes; Exercise - type 1 diabetes; Exercise - type 2 diabetes
Images

Description
Exercise is an important part of managing your diabetes. If you are obese or overweight, exercise can help you manage your weight.
Exercise will Help Your Diabetes
Exercise can help lower your blood sugar without medicines. It reduces your risk of heart disease. Exercise can also lessen the symptoms of depression and reduce stress.
But be patient. It may take several months of regular exercising before you see changes in your health. It is important to understand that exercise can benefit your health even if it does not cause much weight loss.
Talk to Your Doctor First
Your health care provider should make sure your exercise program is safe for you. An exercise program is safe for most people with diabetes. Your provider may ask about symptoms, such as shortness of breath, chest pain, or leg pain that you may get when you walk upstairs or up a hill. In rare cases, your provider will order tests to make sure that you can exercise safely without damaging your heart.
If you take medicines that lower your blood sugar, exercise can make your blood sugar go too low. Talk to your provider or nurse about how to take your medicines when you exercise or how to adjust the doses to prevent low blood sugars.
Some types of vigorous exercise can make your eyes worse if you already have diabetic eye disease. Get an eye exam before starting a new exercise program.
After you start your exercise program, contact your provider if you have any of the following:
- Feel faint, have chest pain, or feel short of breath when you exercise
- Feel pain or numbness in your feet. Also contact your provider if you have sores or blisters on your feet
- Your blood sugar gets too low or too high during or after exercising
Getting Started
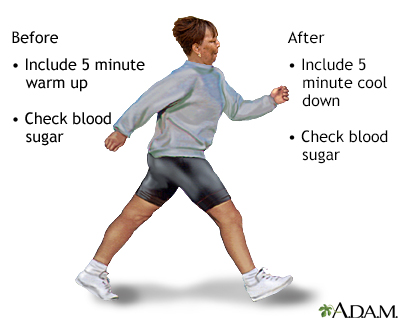
Start with walking. If you are out of shape, start by walking for 5 to 10 minutes a day.
Try to set a goal of fast walking. You should do this for 30 to 45 minutes, at least 5 days a week. In order to lose weight, the amount of exercise may need to be greater. So do more if you can. Swimming or exercise classes are also good.
If you don't have a safe place to walk, or have pain when walking, you can start with body weight exercises in your home. Talk to your provider about which exercises are right for you.
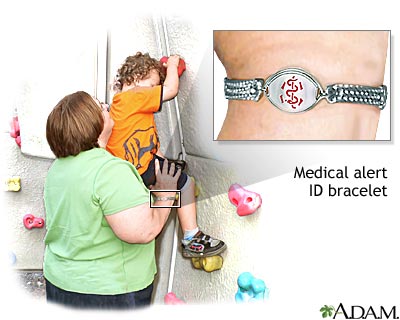
Wear a bracelet or necklace that says you have diabetes. Tell coaches and exercise partners that you have diabetes. Always have fast-acting sources of sugar with you, such as juice or hard candy. Carry a cell phone with emergency phone numbers with you, as well.
Drink plenty of water. Do this before, during, and after exercising. Try to exercise at the same time of day, for the same amount of time, and at the same level. This will make your blood sugar easier to control. If your schedule is less regular, exercising at different times of the day is still better than not exercising at all.
Try to avoid sitting for more than 30 minutes at a time. Get up and stretch. Walk or do some quick exercises like lunges, squats, or wall push-ups.
Your Blood Sugar and Exercise
The blood sugar response to exercise is not always easy to predict. Different types of exercises can make blood sugar go up or down. Most of the time, your response to any specific exercise will be the same. Testing your blood sugar more often is the safest plan.
Check your blood sugar before you exercise. Also, check it during exercise if you are working out for more than 45 minutes, especially if this is an exercise you have not done regularly.
Check your blood sugar again right after exercise, and later on. Exercise can cause your blood sugar to decrease for up to 12 hours after you are done.
If you use insulin, ask your provider when and what you should eat before you exercise. Also, find out how to adjust your insulin dose when you exercise.
Do not inject insulin in a part of your body that you are exercising, such as the shoulders or thighs.
Keep a snack nearby that can raise your blood sugar quickly. Examples are:
- Five or six small soft candies
- One tablespoon (tbsp), or 15 grams, of sugar, plain or dissolved in water
- One tbsp, or 15 milliliters (mL) of honey or syrup
- Three or four glucose tablets
- One half of a 12-ounce can (355 mL) of regular, non-diet soda or sports drink
- One half cup (4 ounces or 118 mL) of fruit juice
Have a larger snack if you will be exercising more than usual. You can also have more frequent snacks. You may need to adjust your medicine if you are planning unusual exercise.
If exercise frequently causes your blood sugar to be low, talk with your provider. You may need to lower the dose of your medicine.
Your Feet and Exercise
Always check your feet and shoes for any problems before and after exercise. You might not feel pain in your feet because of your diabetes. You may not notice a sore or blister on your foot. Contact your provider if you notice any changes on your feet. Small problems can become serious if they go untreated.
Wear socks that keep moisture away from your feet. Also, wear comfortable, well-fitting shoes.
If you have redness, swelling and warmth across the middle of your foot or ankle after exercise let your provider know right away. This can be a sign of a joint problem that is more common in people with diabetes, called Charcot foot.
Related Information
Type 1 diabetesType 2 diabetes
Diabetes - foot ulcers
Diabetes eye care
Diabetes - when you are sick
Diabetes - preventing heart attack and stroke
Diabetes - taking care of your feet
Diabetes tests and checkups
Diabetes - keeping active
Low blood sugar - self-care
Managing your blood sugar
ACE inhibitors
Type 2 diabetes - what to ask your doctor
References
American Diabetes Association Professional Practice Committee. 5. Facilitating positive health behaviors and well-being to improve health outcomes: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Suppl 1):S77-S110. Erratum in: Diabetes Care. 2024;47(4):761-762. PMID: 38078584 pubmed.ncbi.nlm.nih.gov/38078584/.
Dhatariya KK, Umpierrez GE, Crandall JP. Diabetes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 210.
Eckel RH, Jakicic JM, Ard JD, et al. 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines. Circulation. 2014;129(25 Suppl 2):S76-S99. PMID: 24222015 pubmed.ncbi.nlm.nih.gov/24222015/.
Lundgren JA, Kirk SE. The athlete with diabetes. In: Miller MD, Thompson SR, eds. DeLee, Drez, & Miller's Orthopaedic Sports Medicine. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 18.
BACK TO TOPReview Date: 5/20/2024
Reviewed By: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
