Lymphedema - self-care
Breast cancer - self-care for lymphedema; Mastectomy - self-care for lymphedema
Images
Animation

Description
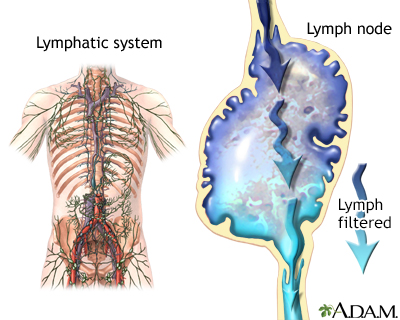
Lymphedema is the buildup of lymph in your body. Lymph is a fluid surrounding tissues. Lymph moves through vessels in the lymph system and into the bloodstream. The lymph system is a major part of the immune system.
What is Lymphedema
When lymph builds up, it can cause an arm, leg, or another area of your body to swell and become painful. The disorder can be lifelong.
What to Expect
Lymphedema may start 6 to 8 weeks after surgery or after radiation treatment for cancer.
It can also start very slowly after your cancer treatment is over. You may not notice symptoms until 18 to 24 months after treatment. Sometimes it can take years to develop.
Ways to Help Relieve Swelling
Use your arm that has lymphedema for everyday activities, such as combing your hair, bathing, dressing, and eating. Rest this arm above the level of your heart 2 or 3 times a day while you are lying down.
- Stay lying down for 45 minutes.
- Rest your arm on pillows to keep it raised.
- Open and close your hand 15 to 25 times while you are lying down.
Taking Care of Your Skin
Every day, clean the skin of your arm or leg that has lymphedema. Use lotion to keep your skin moist. Check your skin every day for any changes.
Protect your skin from injuries, even small ones:
- Use only an electric razor for shaving underarms or legs.
- Wear gardening gloves and cooking gloves.
- Wear gloves when doing work around the house.
- Use a thimble when you sew.
- Be careful in the sun. Use sunscreen with an SPF of 30 or higher.
- Use insect repellent.
- Avoid very hot or cold things, such as ice packs or heating pads.
- Stay out of hot tubs and saunas.
- Have blood draws, intravenous (IV) therapy, and shots in the non-affected arm or in another part of your body.
- Don't wear tight clothing or wrap anything tight on your arm or leg that has lymphedema.
Take care of your feet:
- Cut your toenails straight across. If needed, see a podiatrist to prevent ingrown nails and infections.
- Keep your feet covered when you are outdoors. Do not walk barefoot.
- Keep your feet clean and dry. Wear cotton socks.
Don't put too much pressure on your arm or leg with lymphedema:
- Don't sit in the same position for more than 30 minutes.
- Don't cross your legs while sitting.
- Wear loose jewelry. Wear clothes that do not have tight waistbands or cuffs.
- Where a bra that is supportive, but not too tight.
- If you carry a handbag, carry it with the unaffected arm.
- Don't use elastic support bandages or stockings with tight bands.
Taking care of cuts and scratches:
- Wash wounds gently with soap and water.
- Apply an antibiotic cream or ointment to the area.
- Cover wounds with dry gauze or bandages, but don't wrap them tightly.
- Contact your health care provider right away if you have an infection. Signs of infection include rash, red blotches, swelling, heat, pain, or fever.
Taking care of burns:
- Place a cold pack or run cold water on a burn for 15 minutes. Then wash gently with soap and water.
- Put a clean, dry bandage over the burn.
- Call your provider right away if you have an infection.
Living with lymphedema can be hard. Ask your provider about visiting a physical therapist who can teach you about:
- Ways to prevent lymphedema
- How diet and exercise affect lymphedema
- How to use massage techniques to decrease lymphedema
If you are prescribed a compression sleeve:
- Wear the sleeve during the day. Remove it at night. Make sure you get the right size.
- Wear the sleeve when traveling by air. If possible, keep your arm above the level of your heart during long flights.
When to Call the Doctor
Contact your provider if you have any of these symptoms:
- New rashes or skin breaks that do not heal
- Feelings of tightness in your arm or leg
- Rings or shoes that become tighter
- Weakness in your arm or leg
- Pain, aching, or heaviness in the arm or leg
- Swelling that lasts longer than 1 to 2 weeks
- Signs of infection, such as redness, swelling, or fever of 100.5°F (38°C) or higher
Related Information
Breast lump removalMastectomy
Breast cancer
Breast external beam radiation - discharge
Chest radiation - discharge
Surgical wound care - open
References
Doroshow JH. Approach to the patient with cancer. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 164.
National Cancer Institute website. Lymphedema (PDQ) - health professional version. www.cancer.gov/about-cancer/treatment/side-effects/lymphedema/lymphedema-hp-pdq. Updated April 30, 2024. Accessed May 29, 2024.
Spinelli BA. Clinical conditions in patients with breast cancer. In: Skirven TM, Osterman AL, Fedorczyk JM, eds. Rehabilitation of the Hand and Upper Extremity. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 115.
BACK TO TOPReview Date: 3/31/2024
Reviewed By: Todd Gersten, MD, Hematology/Oncology, Florida Cancer Specialists & Research Institute, Wellington, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
