Heart pacemaker
Cardiac pacemaker implantation; Artificial pacemaker; Permanent pacemaker; Internal pacemaker; Cardiac resynchronization therapy; CRT; Biventricular pacemaker; Arrhythmia - pacemaker; Abnormal heart rhythm - pacemaker; Bradycardia - pacemaker; Heart block - pacemaker; Mobitz - pacemaker; Heart failure - pacemaker; HF - pacemaker; CHF- pacemaker
A pacemaker is a small, battery-operated device. This device senses when your heart is beating too slowly. It sends a signal to your heart that makes your heart beat at the correct pace.
Images
Animation
I Would Like to Learn About:
Description
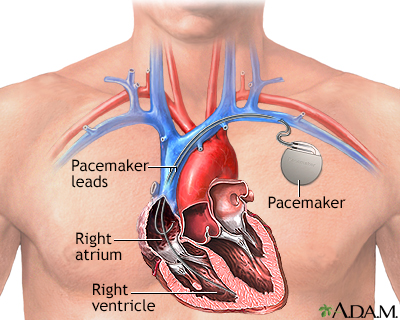
Newer pacemakers weigh as little as 1 ounce (28 grams). Most pacemakers have 2 parts:
- The generator contains the battery and the information to control the heartbeat.
- The leads which are wires that connect the heart to the generator and carry the electrical messages to the heart.
A pacemaker is implanted under the skin. This procedure takes about 1 hour in most cases. You will be given a sedative to help you relax. You will be awake during the procedure.
A small incision (cut) is made. Most often, the cut is on the left side (if you are right handed) of the chest below your collarbone. The pacemaker generator is then placed under the skin at this location. The generator may also be placed in the abdomen, but this is less common. A new "leadless" pacemaker is a self-contained unit that is implanted in the right ventricle of the heart.
Using live x-rays to see the area, the doctor (most often a heart specialist called a cardiologist) puts the leads through the cut, into a vein, and then into the heart. The leads are connected to the generator. The skin is closed with stitches. Most people go home within 1 day of the procedure.
There are 2 kinds of pacemakers used only in medical emergencies. They are:
- Transcutaneous pacemakers
- Transvenous pacemakers
They are not permanent pacemakers.
Why the Procedure Is Performed
Pacemakers may be used for people who have heart problems that cause their heart to beat too slowly. A slow heartbeat is called bradycardia. Two common problems that cause a slow heartbeat are sinus node disease and heart block.
When your heart beats too slowly, your body and brain may not get enough oxygen. Symptoms may be
Some pacemakers can be used to stop a heart rate that is too fast (tachycardia) or that is irregular.
Other types of pacemakers can be used in severe heart failure. These are called biventricular pacemakers. They help coordinate the beating of the heart chambers.
Most biventricular pacemakers implanted today can also work as implantable cardioverter defibrillators (ICD). ICD restore a normal heartbeat by delivering a larger shock when a potentially deadly fast heart rhythm occurs.
Risks
Possible complications of pacemaker surgery are:
- Abnormal heart rhythms
- Bleeding
- Punctured lung. This is rare.
- Infection
- Puncture of the heart, which can lead to bleeding around the heart. This is rare.
A pacemaker senses if the heartbeat is above a certain rate. When it is above that rate, the pacemaker will stop sending signals to the heart. The pacemaker can also sense when the heartbeat slows down too much. It will automatically start pacing the heart again.
Before the Procedure
Always tell your health care provider about all the medicines you are taking, even medicines or herbs you bought without a prescription.
The day before your surgery:
- Shower and shampoo well.
- You may be asked to wash your whole body below your neck with a special soap.
On the day of the surgery:
- You may be asked not to drink or eat anything after midnight the night before your procedure. This includes chewing gum and breath mints. Rinse your mouth with water if it feels dry, but be careful not to swallow.
- Take the medicines you have been told to take with a small sip of water.
Your cardiologist will tell you when to arrive at the hospital.
After the Procedure
You will probably be able to go home after 1 day or even the same day in some cases. You should be able to return to your normal activity level quickly.
Ask your cardiologist how much you can use the arm on the side of your body where the pacemaker was placed. You may be advised not to:
- Lift anything heavier than 10 to 15 pounds (4.5 to 6.75 kilograms)
- Push, pull, and twist your arm for 2 to 3 weeks.
- Raise your arm above your shoulder for several weeks.
When you leave the hospital, you will be given a card to keep in your wallet. This card lists the details of your pacemaker and has contact information for emergencies. You should always carry this wallet card with you. You should try to remember the name of the pacemaker manufacturer if you can in case you lose your card.
Outlook (Prognosis)
Pacemakers can help keep your heart rhythm and heart rate at a safe level for you. The pacemaker battery lasts about 6 to 15 years. Your provider will check the battery regularly and replace it when necessary.
Related Information
Cardiac ablation proceduresImplantable cardioverter-defibrillator
Wolff-Parkinson-White syndrome (WPW)
Heart failure
Sick sinus syndrome
Atrial fibrillation and atrial flutter
Arrhythmias
Implantable cardioverter defibrillator - discharge
Surgical wound care - open
Angina - when you have chest pain
Angina - discharge
Heart attack – discharge
Aspirin and heart disease
Butter, margarine, and cooking oils
Cholesterol and lifestyle
Antiplatelet medicines - P2Y12 inhibitors
Controlling your high blood pressure
Dietary fats explained
Fast food tips
Heart disease - risk factors
How to read food labels
Low-salt diet
Mediterranean diet
Heart failure - discharge
Angina - what to ask your doctor
Heart attack - what to ask your provider
Atrial fibrillation - discharge
References
American College of Cardiology website. The leadless pacemaker. www.acc.org/latest-in-cardiology/ten-points-to-remember/2019/06/10/13/49/the-leadless-pacemaker. Updated June 10, 2019. Accessed July 29, 2024.
Chung MK, Daubert JP. Pacemakers and implantable cardioverter-defibrillators. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 69.
Chung MK, Patton KK, Lau C-P, et al. 2023 HRS/APHRS/LAHRS guideline on cardiac physiologic pacing for the avoidance and mitigation of heart failure. Heart Rhythm. 2023;20(9):e17-e91. PMID: 37283271 pubmed.ncbi.nlm.nih.gov/37283271/.
Glikson M, Nielsen JC, Kronborg MB, et al. 2021 ESC Guidelines on cardiac pacing and cardiac resynchronization therapy: Developed by the Task Force on cardiac pacing and cardiac resynchronization therapy of the European Society of Cardiology (ESC) With the special contribution of the European Heart Rhythm Association (EHRA). European Heart Journal. 2021;42(35):3427-3520. PMID: 34455430 pubmed.ncbi.nlm.nih.gov/34455430/.
Miller JM, Ellenbogen KA. Therapy for cardiac arrhythmias. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 64.
Pfaff JA, Gerhardt RT. Assessment of implantable devices. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 13.
Santucci PA, Wilber DJ. Electrophysiologic procedures and surgery. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 54.
BACK TO TOPReview Date: 7/14/2024
Reviewed By: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
