Vitamin D
Cholecalciferol; Vitamin D3; Ergocalciferol; Vitamin D2
Vitamin D is a fat-soluble vitamin. Fat-soluble vitamins are stored in the body's fatty tissue and liver.
Images

I Would Like to Learn About:
Function
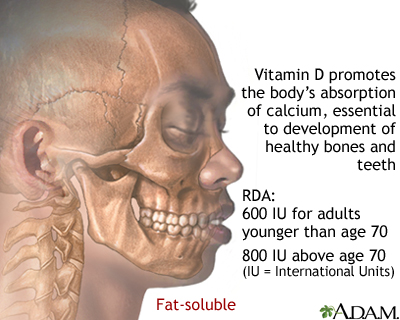
Vitamin D helps the body absorb calcium. Calcium is a mineral that you must have for normal bone formation.
If you do not consume enough calcium in your diet, or if your body does not absorb enough calcium due to low vitamin D, bone production and bone tissues may suffer.
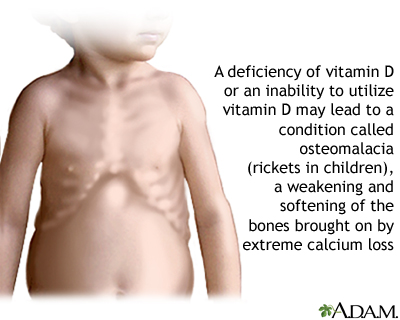
Vitamin D deficiency can lead to weakened bones (osteoporosis in adults or rickets in children).
Food Sources
The body makes vitamin D when the skin is directly exposed to the sun. That is why it is often called the "sunshine" vitamin. Most people meet at least some of their vitamin D needs this way.
Very few foods naturally contain vitamin D. As a result, many foods are fortified with vitamin D. Fortified means that vitamins have been added to the food.
Fatty fish (such as tuna, salmon, and mackerel) are among the best sources of vitamin D.
Beef liver, cheese, and egg yolks provide small amounts.
Mushrooms provide some vitamin D. Some mushrooms you buy in the store have higher vitamin D content because they have been exposed to ultraviolet light.
Most milk in the United States is fortified with 400 IU vitamin D per quart. Most of the time, foods made from milk, such as cheese and ice cream, are not fortified.
Vitamin D is added to many breakfast cereals. It is also added to some brands of soy beverages, orange juice, yogurt, and margarine. Check the nutrition fact panel on the food label.
SUPPLEMENTS
It can be hard to get enough vitamin D from food sources alone. As a result, some people may need to take a vitamin D supplement. Vitamin D found in supplements and fortified foods comes in two different forms:
- D2 (ergocalciferol)
- D3 (cholecalciferol)
Follow a diet that provides the proper amount of calcium and vitamin D. Your provider may recommend higher doses of vitamin D if you have risk factors for osteoporosis or a low level of this vitamin.
Side Effects
Too much vitamin D can make the intestines absorb too much calcium. This may cause high levels of calcium in the blood. High blood calcium can lead to:
- Calcium deposits in soft tissues such as the heart and lungs
- Confusion and disorientation
- Damage to the kidneys
- Kidney stones
- Nausea, vomiting, constipation, poor appetite, weakness, and weight loss
Recommendations
Some experts have suggested that a few minutes of sunlight directly on the skin of your face, arms, back, or legs (without sunscreen) every day can produce the body's requirement of vitamin D. However, the amount of vitamin D produced by sunlight exposure can vary greatly from person to person.
- People who do not live in sunny places may not make enough vitamin D within a limited time in the sun. Cloudy days, shade, and having dark-colored skin also cut down on the amount of vitamin D the skin makes.
- Because exposure to sunlight is a risk for skin cancer, exposure for more than a few minutes without sunscreen is not recommended.
The best measure of your vitamin D status is to look at blood levels of a form known as 25-hydroxyvitamin D (25(OH)D). Blood levels are described either as nanograms per milliliter (ng/mL) or nanomoles per liter (nmol/L), where 0.4 ng/mL = 1 nmol/L.
Levels below 50 nmol/L (20 ng/mL) are too low for bone or overall health, and levels above 125 nmol/L (50 ng/mL) are probably too high. Levels of 75 nmol/L or above (30 ng/mL or above) are enough for most people.
Recommendations for vitamin D, as well as other nutrients, are provided in the Dietary Reference Intakes (DRIs) developed by the Food and Nutrition Board at the National Academies of Sciences, Engineering, and Medicine. DRI is a term for a set of reference intakes that are used to plan and assess the nutrient intakes of healthy people. These values, which vary by age and sex, include:
Recommended Dietary Allowance (RDA): The average daily level of intake that is enough to meet the nutrient needs of nearly all (97% to 98%) healthy people. An RDA is an intake level based on scientific research evidence.
Adequate Intake (AI): This level is established when there is not enough scientific research evidence to develop an RDA. It is set at a level that is thought to ensure enough nutrition.
Dietary Reference Intakes for vitamin D:
Infants (AI)
- 0 to 12 months: 400 IU (10 micrograms [mcg]) per day
Children (RDA)
- 1 to 13 years: 600 IU (15 mcg) per day
- 14 to 18 years: 600 IU (15 mcg) per day
Adults (RDA)
- 19 to 70 years: 600 IU (15 mcg) per day
- Adults over 70 years: 800 IU (20 mcg) per day
- Pregnancy and breastfeeding: 600 IU (15 mcg) per day
The National Osteoporosis Foundation (NOF) recommends a higher dose for people age 50 and older, 800 to 1,000 IU of vitamin D daily. Ask your health care provider which amount is best for you.
Vitamin D toxicity almost always occurs from using too many supplements. The safe upper limit for vitamin D is:
- 1,000 IU/day (25 mcg/day) for infants 0 to 6 months
- 1,500 IU/day (38 mcg/day) for babies 7 to 12 months
- 2,500 IU/day (63 mcg/day) for children 1 to 3years
- 3,000 IU/day (75 mcg/day) for children 4 to 8 years
- 4,000 IU/day (100 mcg/day) for children and adults 9 years and older
One microgram of cholecalciferol (D3) is the same as 40 IU of vitamin D.
Related Information
Calcium in dietPhosphorus in diet
References
Cosman F, de Beur SJ, LeBoff MS, et al. Clinician's Guide to Prevention and Treatment of Osteoporosis. Osteoporos Int. 2014;25(10):2359-2381. PMID: 25182228 pubmed.ncbi.nlm.nih.gov/25182228/.
Mason JB, Booth SL. Vitamins, trace minerals, and other micronutrients. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 205.
Markell M, Siddiqi HA. Vitamins and trace elements. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 27.
National Institutes of Health website. Vitamin D: fact sheet for health professionals. ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Updated August 12, 2022. Accessed February 21, 2023.
BACK TO TOPReview Date: 1/19/2023
Reviewed By: Stefania Manetti, RD/N, CDCES, RYT200, My Vita Sana LLC - Nourish and heal through food, San Jose, CA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
