Asherman syndrome
Uterine synechiae; Intrauterine adhesions; Infertility - Asherman; Asherman's syndrome
Asherman syndrome is the formation of scar tissue in the uterine cavity. The problem most often develops after uterine surgery.
Images
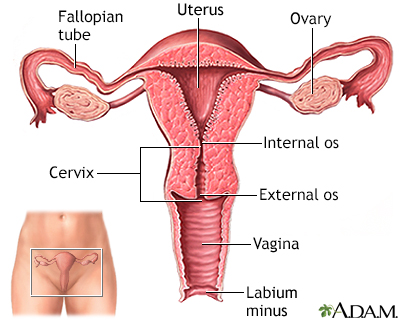
Causes
Asherman syndrome is a rare condition. In most cases, it occurs in women who have had several dilatation and curettage (D&C) procedures.
A severe pelvic infection unrelated to surgery may also lead to Asherman syndrome.
Adhesions in the uterine cavity can also form after infection with tuberculosis or schistosomiasis. These infections are rare in the United States. Uterine complications related to these infections are even less common.
Symptoms
The adhesions may cause:
- Amenorrhea (lack of menstrual periods)
- Repeated miscarriages
- Infertility
However, such symptoms could be related to several conditions. They are more likely to indicate Asherman syndrome if they occur suddenly after a D&C or other uterine surgery.
Exams and Tests
A pelvic exam does not reveal problems in most cases.
Tests may include:
- Hysterosalpingography
- Hysterosonogram
- Transvaginal ultrasound examination
- Hysteroscopy
- Blood tests or other laboratory examinations to detect tuberculosis or schistosomiasis
Treatment
Treatment involves surgery to cut and remove the adhesions or scar tissue. This can most often be done with hysteroscopy. This uses small instruments and a camera placed into the uterus through the cervix.
After scar tissue is removed, the uterine cavity must be kept open while it heals to prevent adhesions from returning. Your health care provider may place a small balloon inside the uterus for several days. You may also need to take estrogen while the uterine lining heals.
You may need to take antibiotics if there is an infection.
Support Groups
The stress of illness can often be helped by joining a support group. In such groups, members share common experiences and problems.
Outlook (Prognosis)
Asherman syndrome can often be cured with surgery. Sometimes more than one procedure will be necessary.
Women who are infertile because of Asherman syndrome may be able to have a baby after treatment. Successful pregnancy depends on the severity of Asherman syndrome and the difficulty of the treatment. Other factors that affect fertility and pregnancy may also be involved.
Possible Complications
Complications of hysteroscopic surgery are uncommon. When they occur, they may include bleeding, perforation of the uterus, and pelvic infection.
In some cases, treatment of Asherman syndrome will not cure infertility.
When to Contact a Medical Professional
Contact your provider if:
- Your menstrual periods do not return after a gynecologic or obstetrical surgery.
- You cannot get pregnant after 6 to 12 months of trying (your provider may ask you to see a specialist for an infertility evaluation).
Prevention
Most cases of Asherman syndrome cannot be predicted or prevented.
Related Information
AdhesionD and C
References
Dolan MS, Hill CC, Valea FA. Benign gynecologic lesions: vulva, vagina, cervix, uterus, oviduct, ovary, ultrasound imaging of pelvic structures. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 18.
Humphreys MA, Branch DW. Recurrent pregnancy loss. In: Lockwood CJ, Copel JA, Dugoff L, et al, eds. Creasy and Resnik's Maternal-Fetal Medicine: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2023:chap 41.
Turocy J, Williams Z. Early and recurrent pregnancy loss: etiology, diagnosis, treatment. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 16.
Wei PK, Savicke AM, Levine D. The uterus. In: Rumack CM, Levine D, eds. Diagnostic Ultrasound. 6th ed. Philadelphia, PA: Elsevier; 2024:chap 28.
BACK TO TOPReview Date: 4/16/2024
Reviewed By: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
