Premature ovarian failure
Ovarian hypofunction; Ovarian insufficiency
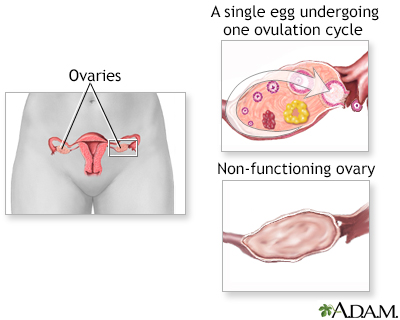
Premature ovarian failure is reduced function of the ovaries (including decreased production of hormones). Ovarian failure that occurs before the age of 40 is considered premature ovarian failure.
Images
I Would Like to Learn About:
Causes
Premature ovarian failure may be caused by genetic factors such as chromosome abnormalities. It may also occur with certain autoimmune disorders that disrupt the normal function of the ovaries. Most often there is no obvious cause, although a family history of the condition may play a role.
Chemotherapy and radiation therapy can also cause premature ovarian failure.
Symptoms
Women with premature ovarian failure may develop symptoms of menopause, which include:
- Hot flashes
- Irregular or absent periods
- Mood swings
- Night sweats
- Vaginal dryness
This condition may also make it hard for a woman to become pregnant.
Exams and Tests
A blood test will be done to check your level of follicle-stimulating hormone, or FSH. FSH levels are higher than normal in women with premature ovarian failure.
A vaginal ultrasound may be done to check how many follicles the ovaries contain. Reduced numbers of ovarian follicles may occur in women who develop this condition.
Other blood tests may be done to look for autoimmune disorders or thyroid disease.
Women with premature ovarian failure who want to become pregnant may be concerned about their ability to conceive. Those younger than age 30 may have a chromosome analysis to check for genetic problems. In most cases, older women who are close to menopause do not need this test.
Treatment
Estrogen therapy often helps relieve menopausal symptoms and prevents bone loss. However, it will not increase your chances of becoming pregnant. Fewer than 1 in 10 women with this condition will be able to get pregnant. The chance of getting pregnant increases to 50% when you use a fertilized donor egg (an egg from another woman).
When to Contact a Medical Professional
Contact your health care provider if:
- You are no longer having monthly periods.
- You have symptoms of early menopause.
- You are having difficulty becoming pregnant.
References
Bulun SE. Physiology and pathology of the female reproductive axis. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 17.
Douglas NC, Lobo RA. Reproductive endocrinology: neuroendocrinology, gonadotropins, sex steroids, prostaglandins, ovulation, menstruation, and hormone assay. In: Lobo RA, Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 4.
Dumesic DA, Gambone JC. Amenorrhea, oligomenorrhea, and hyperandrogenic disorders. In: Hacker NF, Gambone JC, Hobel CJ, eds. Hacker & Moore's Essentials of Obstetrics and Gynecology. 6th ed. Philadelphia, PA: Elsevier; 2016:chap 33.
Fauser BCJM, Broekmans FJ. Female infertility: evaluation and management. In: Robertson RP, ed. DeGroot's Endocrinology. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 123.
Lobo RA, Suh Y. Menopause and aging. In: Strauss JF, Barbieri R, Dokras A, Williams CJ, Williams Z, eds. Yen and Jaffe's Reproductive Endocrinology. 9th ed. Philadelphia, PA: Elsevier; 2024:chap 14.
BACK TO TOPReview Date: 4/16/2024
Reviewed By: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
