Pulmonic valve stenosis
Valvular pulmonary stenosis; Heart valve pulmonary stenosis; Pulmonary stenosis; Stenosis - pulmonary valve; Balloon valvuloplasty - pulmonary
Pulmonic stenosis is a heart valve disorder that involves the pulmonary valve.
This is the valve separating the right ventricle (one of the chambers in the heart) and the pulmonary artery. The pulmonary artery carries oxygen-poor blood to the lungs.
Stenosis, or narrowing, occurs when the valve cannot open wide enough. As a result, blood flows less easily to the lungs.
Images
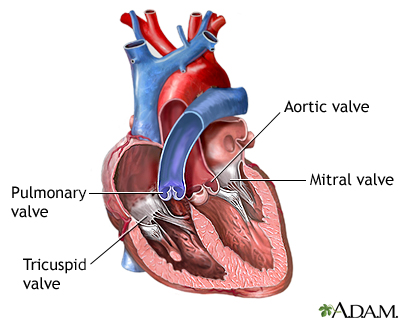
I Would Like to Learn About:
Causes
Narrowing of the pulmonary valve is most often present at birth (congenital). It is caused by a problem that occurs as the baby develops in the womb before birth. The cause is unknown, but genes may play a role.
Narrowing that occurs in the valve itself is called valvular pulmonic stenosis. There may also be narrowing just before or after the valve.
The defect may occur alone or with other heart defects that are present at birth. The condition can be mild or severe.
Pulmonic stenosis is a rare disorder. In some cases, the problem runs in families.
Symptoms
Many cases of pulmonic stenosis are mild and do not cause symptoms. The problem is most often found in infants when a heart murmur is heard during a routine heart exam.
When the valve narrowing (stenosis) is moderate to severe, the symptoms include:
- Abdominal distention
- Bluish color to the skin (cyanosis) in some people
- Poor appetite
- Chest pain
- Fainting
- Fatigue
- Poor weight gain or failure to thrive in infants with a severe blockage
- Shortness of breath
- Sudden death
Symptoms may get worse with exercise or activity.
Exams and Tests
The health care provider may hear a heart murmur when listening to the heart using a stethoscope. Murmurs are blowing, whooshing, or rasping sounds heard during a heartbeat.
Tests used to diagnose pulmonary stenosis may include:
- Cardiac catheterization
- Chest x-ray
- Electrocardiogram (ECG)
- Echocardiogram
- MRI of the heart
The provider will grade the severity of the valve stenosis to plan treatment.
Treatment
Sometimes, treatment may not be needed if the disorder is mild.
When there are also other heart defects, medicines may be used to:
- Help blood flow through the heart (prostaglandins)
- Help the heart beat stronger
- Prevent clots (blood thinners)
- Remove excess fluid (water pills)
- Treat abnormal heartbeats and rhythms
Percutaneous balloon pulmonary dilation (valvuloplasty) may be performed when no other heart defects are present.
- This procedure is done through an artery in the groin.
- The doctor sends a flexible tube (catheter) with a balloon attached to the end up to the heart. Special x-rays are used to help guide the catheter.
- The balloon stretches the opening of the valve.
Some people may need heart surgery to repair or replace the pulmonary valve. The new valve can be made from different materials. If the valve cannot be repaired or replaced, other procedures may be needed.
Outlook (Prognosis)
People with mild disease rarely get worse. However, those with moderate to severe disease will get worse. The outcome is often very good when surgery or balloon dilation is successful. Other congenital heart defects may be a factor in the outlook.
Most often, the new valves can last for decades. However, some will wear out and need to be replaced.
Possible Complications
Complications may include:
- Abnormal heartbeats (arrhythmias)
- Death
- Heart failure and enlargement of the right side of the heart
- Leaking of blood back into the right ventricle (pulmonary valve regurgitation) after repair
When to Contact a Medical Professional
Contact your provider if:
- You have symptoms of pulmonary valve stenosis.
- You have been treated or have untreated pulmonary valve stenosis and have developed swelling (of the ankles, legs, or abdomen), difficulty breathing, or other new symptoms.
Related Information
Rheumatic feverEndocarditis
Heart failure
Heart valve surgery - discharge
References
Carabello BA, Kodali S. Valvular heart disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 60.
Pellikka PA, Nkomo VT. Tricuspid, pulmonic, and multivalvular disease In: Libby, P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 77.
Sharkey A, Choudhury N, Mahmood F. Valvular heart disease. In: Hines RL, Jones SB, eds. Stoelting's Anesthesia and Co-Existing Disease. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 6.
Therrien J, Marelli AJ. Congenital heart disease in adults. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 61.
Valente AM, Dorfman AL, Babu-Narayan SV, Krieger EV. Congenital heart disease in the adolescent and adult. In: Libby, P, Bonow RO, Mann DL, Tomaselli, GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 82.
BACK TO TOPReview Date: 5/13/2024
Reviewed By: Mary C. Mancini, MD, PhD, Cardiothoracic Surgeon, Shreveport, LA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
