Osmotic demyelination syndrome
ODS; Central pontine demyelination; Central pontine myelinolysis
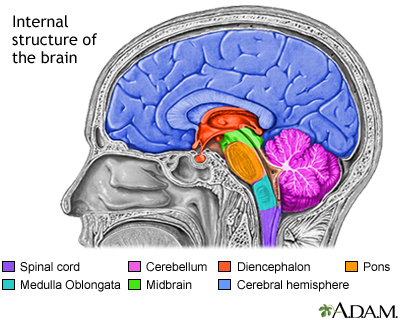
Osmotic demyelination syndrome (ODS) leads to brain cell dysfunction. It is caused by the destruction of the layer (myelin sheath) covering nerve cells in the brain, most often the middle of the brainstem (pons).
Images
I Would Like to Learn About:
Causes
When the myelin sheath that covers nerve cells is destroyed, signals from one nerve to another aren't properly transmitted. Although the brainstem is mainly affected, other areas of the brain can also be involved.
The most common cause of ODS is a quick change in the body's blood sodium levels. This most often occurs when someone is being treated for low blood sodium (hyponatremia) and the sodium is replaced too fast. Sometimes, it occurs when a high level of sodium in the body (hypernatremia) is corrected too quickly.
ODS does not usually occur on its own. Most often, it's a complication of treatment for other problems, or from the other problems themselves.
Risks include:
- Alcohol use
- Liver disease
- Malnutrition from serious illnesses
- Radiation treatment of the brain
- Severe nausea and vomiting during pregnancy
Symptoms
Symptoms may include any of the following:
- Confusion, delirium, hallucinations
- Balance problems, tremor
- Problem swallowing
- Reduced alertness, drowsiness or sleepiness, lethargy, poor responses
- Slurred speech (dysarthria)
- Weakness in the face, arms, or legs, usually affecting both sides of the body
Exams and Tests
Your health care provider will perform a physical exam and ask about the symptoms.
A head MRI scan may reveal a problem in the brainstem (pons) or other parts of the brain. This is the main diagnostic test.
Other tests may include:
- Blood sodium level and other blood tests
- Brainstem auditory evoked response (BAER)
Treatment
ODS is an emergency disorder that needs to be treated in the hospital though most people with this condition are already in the hospital for another problem.
There is no known cure for central pontine myelinolysis. Treatment is focused on relieving symptoms.
Physical therapy may help maintain muscle strength, mobility, and function in weakened arms and legs.
Outlook (Prognosis)
The nerve damage caused by central pontine myelinolysis is often long-lasting. The disorder can cause serious long-term (chronic) disability.
Possible Complications
Complications may include:
- Decreased ability to interact with others
- Decreased ability to work or care for self
- Inability to move, other than to blink eyes ("locked in" syndrome)
- Permanent nervous system damage
When to Contact a Medical Professional
There is no real guideline on when to seek medical attention, because ODS is rare in the general community.
Prevention
In the hospital, slow, controlled treatment of a low sodium level may reduce the risk for nerve damage in the pons. Being aware of how some medicines can change sodium levels can prevent the level from changing too quickly.
Related Information
MyelinLow blood sodium
Alcohol use disorder
Wernicke-Korsakoff syndrome
References
Weissenborn K, Lockwood AH. Toxic and metabolic encephalopathies. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 84.
Yaqoob MM, McCafferty K. Water balance, fluids and electrolytes. In: Feather A, Randall D, Waterhouse M, eds. Kumar and Clark's Clinical Medicine. 10th ed. Philadelphia, PA: Elsevier; 2021:chap 9.
BACK TO TOPReview Date: 6/13/2024
Reviewed By: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
