Craniopharyngioma
A craniopharyngioma is a noncancerous (benign) tumor that develops at the base of the brain near the pituitary gland.
Images
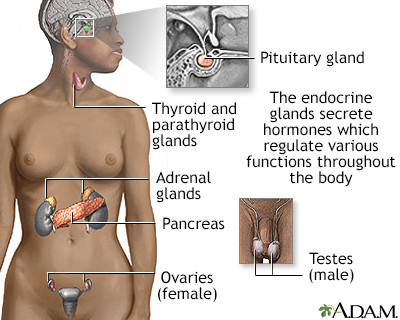
Causes
The exact cause of the tumor is unknown.
This tumor most commonly affects children from 5 to 10 years of age. Adults can sometimes be affected. Boys and girls are equally likely to develop this tumor.
Symptoms
Craniopharyngioma causes symptoms by:
- Increasing pressure on the brain, usually from hydrocephalus
- Disrupting hormone production by the hypothalamus or pituitary gland
- Pressure or damage to the optic nerve
Increased pressure on the brain can cause:
- Headache
- Nausea
- Vomiting (especially in the morning)
- Change in appetite and weight
- Confusion and drowsiness
Damage to the pituitary gland causes hormone imbalances that can lead to excessive thirst and urination, and slow growth.
When the optic nerve is damaged by the tumor, vision problems develop. These defects are often permanent. They may get worse after surgery to remove the tumor.
Behavioral and learning problems may be present.
Exams and Tests
Your health care provider will perform a physical exam. Tests will be done to check for a tumor. These may include:
- Blood tests to measure hormone levels
- CT scan or MRI scan of the brain
- Examination of the nervous system
- Testing your vision
Treatment
The goal of the treatment is to relieve symptoms. Usually, surgery has been the main treatment for craniopharyngioma. However, radiation treatment instead of surgery or along with a smaller surgery may be the best choice for some people.
In tumors that cannot be removed completely with surgery alone, radiation therapy is used. If the tumor has a classic appearance on CT scan, a biopsy may not be needed if treatment with radiation alone is planned. In some people, a shunt may be placed to treat the hydrocephalus.
Stereotactic radiosurgery is performed at some medical centers.
This tumor is best treated at a center with experience in treating craniopharyngiomas.
Outlook (Prognosis)
In general, the outlook is good. There is an 80% to 90% chance of a cure if the tumor can be completely removed with surgery or treated with high doses of radiation. If the tumor returns, it will most often come back within the first 2 years after surgery.
The outlook depends on several factors, including:
- Whether the tumor can be completely removed
- Which nervous system problems and hormonal imbalances the tumor and treatment cause
Most of the problems with hormones and vision do not improve with treatment. Sometimes, the treatment may even make them worse.
Possible Complications
There may be long-term hormone, vision, and nervous system problems after craniopharyngioma is treated.
When the tumor is not completely removed, the condition may return.
When to Contact a Medical Professional
Contact your provider for the following symptoms:
- Headache, confusion, drowsiness, nausea, vomiting, or balance problems (signs of increased pressure on the brain)
- Failing to keep up in school
- Loss or gain of weight
- Increased thirst and urination
- Poor growth in a child
- Vision changes
Related Information
TumorEndocrine glands
References
Lohkamp LN, Kasper EM, Pousa AE, Bartels UK. An update on multimodal management of craniopharyngioma in children. Front Oncol. 2023;13:1149428. PMID: 37213301 pubmed.ncbi.nlm.nih.gov/37213301/.
Styne DM. Physiology and disorders of puberty. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 26.
Suh JH, Chao ST, Murphy ES, Recinos PF. Pituitary tumors and craniopharyngiomas. In: Tepper JE, Foote RL, Michalski JM, eds. Gunderson & Tepper's Clinical Radiation Oncology. 5th ed. Philadelphia, PA: Elsevier; 2021:chap 34.
Zaky W. Central nervous system tumors in childhood. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 546.
BACK TO TOPReview Date: 5/10/2024
Reviewed By: Luc Jasmin, MD, Ph.D., FRCS (C), FACS, Department of Neuroscience, Guam Regional Medical City, Guam; Department of Surgery, Johnson City Medical Center, TN; Department of Maxillofacial Surgery at UCSF, San Francisco, CA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
