Peutz-Jeghers syndrome
PJS
Peutz-Jeghers syndrome (PJS) is a rare disorder in which growths called polyps form in the intestines. A person with PJS has a high risk for developing certain cancers.
Images
Causes
It is unknown how many people are affected by PJS. However, the National Institutes of Health estimates that it affects about 1 in 50,000 to 200,000 people.
PJS is caused by a mutation in the gene called STK11 (previously known as LKB1). There are two ways that PJS can occur:
- Familial PJS is inherited in families as an autosomal dominant trait. That means if one of your parents has this type of PJS, you have a 50% chance of inheriting the gene and having the disease.
- Spontaneous PJS is not inherited from a parent. The gene mutation occurs on its own. Once someone carries the genetic change, their children have a 50% chance of inheriting it.
Symptoms
Symptoms of PJS are:
- Brownish or bluish-gray spots on the lips, gums, inner lining of the mouth, and skin
- Clubbed fingers or toes
- Cramping pain in the belly area
- Dark freckles on and around the lips of a child
- Blood in the stool that can be seen with the naked eye (sometimes)
- Vomiting
Exams and Tests
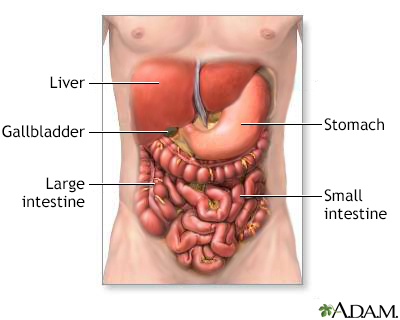
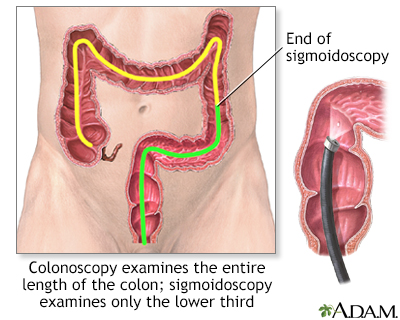
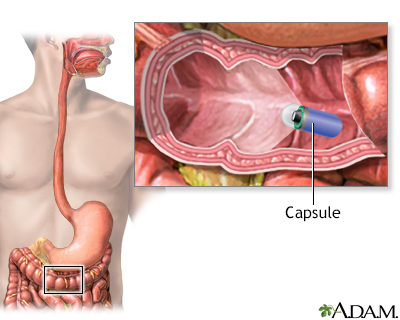
The polyps develop mainly in the small intestine, but also in the large intestine (colon). An exam of the colon called a colonoscopy will show colon polyps. The small intestine is evaluated in two ways. One is a barium x-ray (small bowel series). The other is a capsule endoscopy, in which a small camera is swallowed and then takes many pictures as it travels through the small intestine.
Additional exams may show:
- Part of the intestine folded in on itself (intussusception)
- Benign (noncancerous) tumors in the nose, airways, ureters, or bladder
Laboratory tests may include:
- Complete blood count (CBC) -- may reveal anemia
- Genetic testing
- Stool occult blood, to look for blood in stool
- Total serum iron and iron-binding capacity (TIBC) -- may indicate iron-deficiency anemia
Treatment
Surgery may be needed to remove polyps that cause long-term problems. Iron supplements help counteract blood loss.
People with this condition should be monitored by a health care provider and checked regularly for cancerous polyp changes.
Support Groups
More information and support for people with PJS and their families can be found at:
- National Organization for Rare Disorders (NORD) -- rarediseases.org/rare-diseases/peutz-jeghers-syndrome
- Genetic and Rare Diseases Information Center (GARD) -- rarediseases.info.nih.gov/diseases/7378/peutz-jeghers-syndrome
Outlook (Prognosis)
There may be a high risk for these polyps becoming cancerous. Some studies link PJS with cancers of the gastrointestinal tract, lung, breast, uterus, and ovaries.
Possible Complications
Complications may include:
- Intussusception
- Polyps that lead to cancer
- Ovarian cysts
- A type of ovarian tumors called sex cord tumors
When to Contact a Medical Professional
Contact your provider for an appointment if you or your child has symptoms of this condition. Severe abdominal pain may be a sign of an emergency condition such as intussusception.
Prevention
Genetic counseling is recommended if you are planning to have children and have a family history of this condition.
Related Information
Colorectal polypsAutosomal dominant
Ovarian cysts
References
Garber JJ, Chung DC. Colonic polyps and polyposis syndromes. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 126.
McGarrity TJ, Amos CI, Baker MJ. Peutz-Jeghers syndrome. In: Adam MP, Ardinger HH, Pagon RA, et al, eds. GeneReviews. Seattle, WA: University of Washington. www.ncbi.nlm.nih.gov/books/NBK1266/. Updated September 2, 2021. Accessed April 18, 2024.
Zahler SG, Kabbany MN, Murray KF. Tumors of the digestive tract. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 393.
BACK TO TOPReview Date: 12/31/2023
Reviewed By: Anna C. Edens Hurst, MD, MS, Associate Professor in Medical Genetics, The University of Alabama at Birmingham, Birmingham, AL. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

Health Content Provider
06/01/2025
|
A.D.A.M., Inc. is accredited by URAC, for Health Content Provider (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics. This site complied with the HONcode standard for trustworthy health information from 1995 to 2022, after which HON (Health On the Net, a not-for-profit organization that promoted transparent and reliable health information online) was discontinued. |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997- 2025 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
