Pancreatitis - discharge
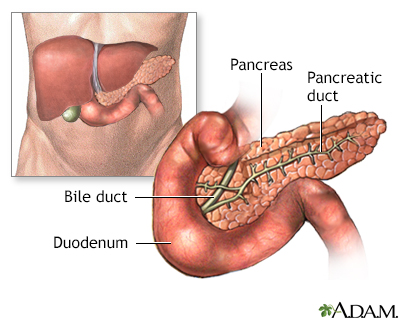
Chronic pancreatitis - discharge; Pancreatitis - chronic - discharge; Pancreatic insufficiency - discharge; Acute pancreatitis - dischargeYou were in the hospital because you have pancreatitis. This is a swelling (inflammation) of the pancreas. This article tells you what you need to know to take care of yourself after you go home from the hospital.
- When You're in the Hospital
During your stay in the hospital, you may have had blood tests and imaging exams, such as a CT scan or ultrasound. You may have been given medicines to help your pain or to fight and prevent infections. You may have been given fluids through an intravenous (IV) tube in your vein and nutrition through a feeding tube or IV. You may have had a tube inserted through your nose that helped remove the contents of your stomach.
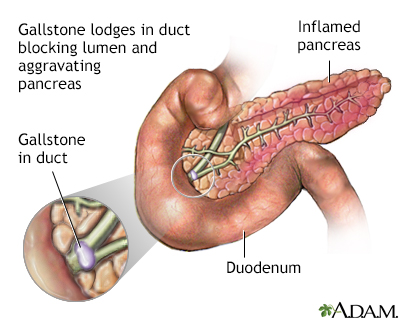
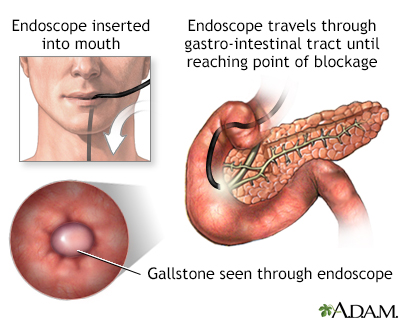
If your pancreatitis was caused by gallstones or a blocked bile or pancreatic duct, you may have had surgery. Your health care provider may also have drained a cyst (collection of fluid) in your pancreas.
You may have had a feeding tube to feed your intestine in the hospital which is helpful during most bouts of pancreatitis.
- Self-care
After an episode of pain from pancreatitis, you should start off with drinking only clear liquids, such as soup broth or gelatin. You will need to follow this diet until your symptoms get better. Slowly add other foods back to your diet when you are better.
Talk with your provider about:
- Eating a healthy diet that is low in fat, with no more than 30 grams of fat per day
- Eating foods that are high in protein and carbohydrates, but low in fat. Eat smaller meals, and eat more often. Your provider will help make sure you are getting enough calories to not lose weight.
- Quitting smoking or using other tobacco products, if you use them.
- Losing weight, if you are overweight.
Always talk to your provider before taking any medicines or herbs.
Do not drink any alcohol.
If your body can no longer absorb fats that you eat, your provider may ask you to take a medicine called pancreatic enzymes. These will help your body better absorb fats in your food.
- You will need to take this medicine with every meal and snack. Your provider will tell you how much to take.
- When you take these enzymes, you may also need to take another medicine to decrease the acid in your stomach.
If your pancreas has a lot of damage, you may also develop diabetes. You will be checked for this problem.
- Managing Your Pain
Avoiding alcohol, tobacco, and foods that make your symptoms worse is the first step to controlling pain.
Use acetaminophen (Tylenol) or nonsteroidal anti-inflammatory drugs, such as ibuprofen (Advil, Motrin), at first to try and control your pain.
You will get a prescription for pain medicines. Get it filled when you go home so you have it available. If the pain is getting worse, take your pain medicine to help before the pain becomes very bad.
- When to Call the Doctor
Contact your provider if you have:
- Very bad pain that is not relieved by over-the-counter drugs
- Problems eating, drinking, or taking your drugs because of nausea or vomiting
- Problems breathing or a very fast heartbeat
- Pain with fever, chills, frequent vomiting, or with feeling faint, weak, or tired
- Weight loss or problems digesting your food
- Yellow color to your skin and the whites of your eyes (jaundice)
References
Forsmark CE. Pancreatitis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 130.
Tenner S, Vege SS, Sheth SG, et al. American College of Gastroenterology guideline: management of acute pancreatitis. Am J Gastroenterol. 2024;119(3):419-437. PMID: 38857482 pubmed.ncbi.nlm.nih.gov/38857482/.
Van Buren G, Fisher WE. Acute and chronic pancreatitis. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier; 2024:175-182.
Vege SS. Acute pancreatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 58.