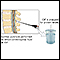
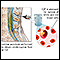
Cerebrospinal fluid (CSF) collection
Spinal tap; Ventricular puncture; Lumbar puncture; Cisternal puncture; Cerebrospinal fluid cultureCerebrospinal fluid (CSF) collection is a test to look at the fluid that surrounds the brain and spinal cord.
CSF acts as a cushion, protecting the brain and spine from injury. The fluid is normally clear. It has the same consistency as water. The test is also used to measure pressure in the spinal fluid.
-
How the Test is Performed
There are different ways to get a sample of CSF. Lumbar puncture (spinal tap) is the most common method.
To have the test:
- You will lie on your side with your knees pulled up toward the chest, and chin tucked downward. Sometimes the test is done sitting up, but bent forward.
- After the back is cleaned, the health care provider will inject a local numbing medicine (anesthetic) into the lower spine.
- A spinal needle will be inserted.
- An opening pressure is sometimes taken. An abnormal pressure can indicate an infection or other problem.
- Once the needle is in position, and after the CSF pressure is measured, a sample of 1 to 10 milliliters (mL) of CSF is collected in 4 vials.
- The needle is removed, the area is cleaned, and a bandage is placed over the needle site. You may be asked to remain lying down for a short time after the test.
In some cases, special x-rays are used to help guide the needle into position. This is called fluoroscopy.
Lumbar puncture with fluid collection may also be part of other procedures such as an x-ray or CT scan after dye has been inserted into the CSF.
Rarely, other methods of CSF collection may be used.
- Cisternal puncture uses a needle placed below the occipital bone (back of the skull). It can be dangerous because it is so close to the brain stem. It is always done with fluoroscopy or other imaging guidance.
- Ventricular puncture may be recommended in people with possible brain herniation. It is most often done in the operating room. A hole is drilled in the skull, and a needle is inserted directly into one of the brain's ventricles.
CSF may also be collected from a tube that is already placed in the fluid, such as a shunt or a ventricular drain.
-
How to Prepare for the Test
You will need to give the health care team your consent before the test. Tell your provider if you are on any aspirin or any other blood-thinning medicines.
After the procedure, you should plan to rest for several hours, even if you feel fine. This is to prevent fluid from leaking around the site of the puncture. You will not need to lie flat on your back the entire time. If you develop a headache, it may be helpful to drink caffeinated beverages such as coffee, tea or soda.
-
How the Test will Feel
It may be uncomfortable to stay in position for the test. Staying still is important because movement may lead to injury of the spinal cord.
You may be told to straighten your position slightly after the needle is in place. This is to help measure the CSF pressure.
The anesthetic will sting or burn when first injected. There will be a hard pressure sensation when the needle is inserted. Often, there is some brief discomfort when the needle goes through the tissue surrounding the spinal cord. This pain should stop in a few seconds.
In most cases, the procedure takes about 30 minutes. The actual pressure measurements and CSF collection only take a few minutes.
-
Why the Test is Performed
This test is done to measure pressures within the CSF and to collect a sample of the fluid for further testing.
CSF analysis can be used to diagnose certain neurologic disorders. These may include infections (such as meningitis) and brain or spinal cord damage. A spinal tap may also be done to establish the diagnosis of normal pressure hydrocephalus or bleeding into the spinal fluid from an aneurysm.
-
Normal Results
Normal values typically range as follows:
- Pressure: 70 to 180 mm H2O
- Appearance: clear, colorless
- CSF total protein: 15 to 60 mg/100 mL (0.15 to 0.6 g/L)
- Gamma globulin: 3% to 12% of the total protein
- CSF glucose: 50 to 80 mg/100 mL or 2.77 to 4.44 mmol/L (or greater than two thirds of blood sugar level)
- CSF cell count: 0 to 5 white blood cells (all mononuclear), and no red blood cells
- Chloride: 110 to 125 mEq/L
Normal value ranges may vary slightly among different laboratories. Talk to your provider about the meaning of your specific test results.
The examples above show the common measurements for results for these tests. Some laboratories use different measurements or may test different specimens.
-
What Abnormal Results Mean
If the CSF looks cloudy, it could mean there is an infection or a buildup of white blood cells or protein.
If the CSF looks bloody or red, it may be a sign of bleeding or spinal cord obstruction. If it is brown, orange, or yellow, it may be a sign of increased CSF protein or previous bleeding (more than 3 days ago). There may be blood in the sample that came from the spinal tap itself. This makes it harder to interpret the test results.
CSF PRESSURE
- Increased CSF pressure may be due to increased intracranial pressure (pressure within the skull).
- Decreased CSF pressure may be due to spinal block, dehydration, or CSF leakage.
CSF PROTEIN
- Increased CSF protein may be due to blood in the CSF, diabetes, polyneuritis, tumor, injury, or any inflammatory or infectious condition.
- Decreased protein is a sign of rapid CSF production or systemic loss of protein.
CSF GLUCOSE
- Increased CSF glucose is a sign of high blood sugar.
- Decreased CSF glucose may be due to hypoglycemia (low blood sugar), bacterial or fungal infection (such as meningitis), tuberculosis, or certain other types of meningitis.
BLOOD CELLS IN CSF
- Increased white blood cells in the CSF may be a sign of meningitis, acute infection, beginning of a long-term (chronic) illness, tumor, abscess, or demyelinating disease (such as multiple sclerosis).
- Red blood cells in the CSF sample may be a sign of bleeding into the spinal fluid or the result of a traumatic lumbar puncture.
OTHER CSF RESULTS
- Increased CSF gamma globulin levels may be due to diseases such as multiple sclerosis, neurosyphilis, or Guillain-Barré syndrome.
Additional conditions under which the test may be performed:
- Chronic inflammatory polyneuropathy
- Dementia due to metabolic causes
- Encephalitis
- Epilepsy
- Febrile seizure (children)
- Generalized tonic-clonic seizure
- Hydrocephalus
- Normal pressure hydrocephalus (NPH)
- Pituitary tumor
- Reye syndrome
-
Risks
Risks of lumbar puncture include:
- Bleeding into the spinal canal or around the brain (subdural hematomas).
- Discomfort during the test.
- Headache after the test that can last a few hours or days. It may be helpful to drink caffeinated beverages such as coffee, tea or soda to help relieve the headache. If headaches last more than a few days (especially when you sit, stand or walk) you might have a CSF-leak. You should talk to your physician if this occurs.
- Hypersensitivity (allergic) reaction to the anesthetic.
- Infection introduced by the needle going through the skin.
Brain herniation may occur if this test is done on a person with a mass in the brain (such as a tumor or abscess). This can result in brain damage or death. This test is not done if an exam or test reveals signs of a brain mass.
Damage to the nerves in the spinal cord may occur, particularly if the person moves during the test.
Cisternal puncture or ventricular puncture carries additional risks of brain or spinal cord damage and bleeding within the brain.
-
Considerations
This test is more dangerous for people with:
- A tumor in the back of the brain that is pressing down on the brainstem
- Blood clotting problems
- Low platelet count (thrombocytopenia)
- Individuals taking blood thinners, aspirin, clopidogrel, or other similar drugs to decrease the formation of blood clots.
References
Deluca GC, Griggs RC. Approach to the patient with neurologic disease. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 368.
Euerle BD. Spinal puncture and cerebrospinal fluid examination. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 60.
Rosenberg GA. Brain edema and disorders of cerebrospinal fluid circulation. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 88.