Bronchiolitis - discharge
RSV bronchiolitis - discharge; Respiratory syncytial virus bronchiolitis - dischargeYour child has bronchiolitis, which causes swelling and mucus to build up in the smallest air passages of the lungs.
Bronchiolitis
Bronchiolitis is swelling and mucus buildup in the smallest air passages in the lungs (bronchioles). It is usually due to a viral infection....

Now that your child is going home from the hospital, follow your health care provider's instructions on how to care for your child. Use the information below as a reminder.
When You're in the Hospital
In the hospital, your provider helped your child breathe better. They also made sure your child received enough fluids.
What to Expect at Home
Your child will likely still have symptoms of bronchiolitis after leaving the hospital.
- Wheezing may last for up to 5 days.
Wheezing
Wheezing is a high-pitched whistling sound during breathing. It occurs when air moves through narrowed breathing tubes in the lungs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Coughing and stuffy nose will slowly get better over 7 to 14 days.
- Sleeping and eating may take up to 1 week to return to normal.
- You may need to take time off work to care for your child.
Home Care
Breathing moist (wet) air helps loosen the sticky mucus that may be choking your child. You can use a humidifier to make the air moist. Follow the directions that came with the humidifier.
Do not use steam vaporizers because they can cause burns. Use cool mist humidifiers instead.
If your child's nose is stuffy, your child will not be able to drink or sleep easily. You can use warm tap water or saline nose drops to loosen the mucus. Both of these work better than any medicine you can buy.
- Place 3 drops of warm water or saline in each nostril.
- Wait 10 seconds, then use a soft rubber suction bulb to suck out the mucus from each nostril.
- Repeat several times until your child is able to breathe through the nose quietly and easily.
Before anyone touches your child, they must wash their hands with warm water and soap or use an alcohol-based hand cleanser before doing so. Try to keep other children away from your child.
Do not let anyone smoke in the house, car, or anywhere near your child.
Eating and Drinking
It is very important for your child to drink enough fluids.
- Offer breast milk or formula if your child is younger than 12 months.
- Offer regular milk if your child is older than 12 months.
Eating or drinking may make your child tired. Feed small amounts, but more often than usual.
If your child throws up because of coughing, wait a few minutes and try to feed your child again.
Medicines
Some asthma medicines help children with bronchiolitis. Your provider may prescribe such medicines for your child.
Do not give your child decongestant nose drops, antihistamines, or any other cold medicines unless your provider tells you to.
When to Call the Doctor
Contact your provider right away if your child has any of the following:
- Hard time breathing
- Chest muscles are pulling in with each breath
Pulling in
Intercostal retractions occur when the muscles between the ribs pull inward. The movement is most often a sign that the person has a breathing probl...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Breathing faster than 50 to 60 breaths per minute (when not crying)
- Making a grunting noise
- Sitting with shoulders hunched over
- Wheezing becomes more intense
- Skin, nails, gums, lips, or area around the eyes is bluish or grayish
- Extremely tired
- Not moving around very much
- Limp or floppy body
- Nostrils are flaring out when breathing
Flaring out
Nasal flaring occurs when the nostrils widen while breathing. It is often a sign of trouble breathing.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
References
Greenland JR, Jones KD, Singer JP. Bronchiolitis. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 72.
Kliegman RM, St. Geme JW, Blum NJ, et al. Wheezing, bronchiolitis, and bronchitis. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 439.
Scarfone RJ, Seiden JA. Pediatric lower airway obstruction. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 163.
Bronchiolitis - illustration
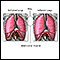
Bronchiolitis is an inflammation of the bronchioles (smaller airways that branch off the main airway) usually caused by a viral infection.
Bronchiolitis
illustration
Review Date: 4/1/2024
Reviewed By: Charles I. Schwartz, MD, FAAP, Clinical Assistant Professor of Pediatrics, Perelman School of Medicine at the University of Pennsylvania, General Pediatrician at PennCare for Kids, Phoenixville, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


