Urinary incontinence - injectable implant
Intrinsic sphincter deficiency repair; ISD repair; Injectable bulking agents for stress urinary incontinenceInjectable implants are injections of material into the wall of the urethra to help control urine leakage (urinary incontinence) caused by a weak urinary sphincter. The sphincter is a muscle that allows your body to hold urine in the bladder. If your sphincter muscle stops working well, you will have urine leakage.
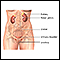
Urinary incontinence
Urinary (or bladder) incontinence occurs when you are not able to keep urine from leaking out of your urethra. The urethra is the tube that carries ...
Description
The material that is injected is permanent. Coaptite and Macroplastique are examples of two brands.
The surgeon injects material through a needle into the wall of your urethra. This is the tube that carries urine from your bladder out of your body. The material bulks up the urethral tissue, causing it to tighten. This stops urine from leaking out of your bladder.
You may receive one of the following types of anesthesia (pain relief) for this procedure:
- Local anesthesia (only the area being worked on will be numb)
-
Spinal anesthesia (you will be numb from the waist down)
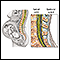
Spinal anesthesia
Spinal and epidural anesthesia are procedures that deliver medicines that numb parts of your body to block pain. They are given through shots in or ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
General anesthesia (you will be asleep and not able to feel pain)
General anesthesia
General anesthesia is treatment with certain medicines that puts you into a deep sleep-like state so you do not feel pain during surgery. After you ...
Read Article Now Book Mark Article
After you are numb or asleep from anesthesia, the surgeon puts a medical device called a cystoscope into your urethra. The cystoscope allows your surgeon to see the area.
Then the surgeon passes a needle through the cystoscope into your urethra. Material is injected into the wall of the urethra or bladder neck through this needle. The surgeon can also inject material into the tissue next to the sphincter.
The implant procedure is usually done in the hospital. Or, it is done in your surgeon's office. The procedure takes about 20 to 30 minutes.
Why the Procedure Is Performed
Implants can help both men and women.
Men who have urine leakage after prostate surgery may choose to have implants.
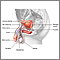
Prostate surgery
Transurethral resection of the prostate (TURP) is a surgery to remove the inside part of the prostate gland. It is done in order to treat symptoms o...
Women who have urine leakage and want a simple procedure to control the problem may choose to have an implant procedure. These women may not want to have surgery that requires general anesthesia or a long recovery after surgery.
Risks
Risks for this procedure are:
- Damage to the urethra or bladder
- Urine leakage that gets worse
- Pain where the injection was done
- Allergic reaction to the material
- Implant material that moves (migrates) to another area of the body
-
Trouble urinating after the procedure
Trouble urinating
Painful urination is any pain, discomfort, or burning sensation when passing urine.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
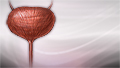
Urinary tract infection
Urinary tract infection
A urinary tract infection, or UTI, is an infection of the urinary tract. The infection can occur at different points in the urinary tract, including...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Blood in the urine
Blood in the urine
Blood in your urine is called hematuria. The amount may be very small and only detected with urine tests or under a microscope. In other cases, the...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Before the Procedure
Tell your surgeon what medicines you are taking. This includes medicines, supplements, or herbs you bought without a prescription.
You may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), vitamin E, warfarin (Coumadin), and any other medicines that make it hard for your blood to clot (blood thinners).
On the day of your procedure:
- You may be asked not to drink or eat anything for 6 to 12 hours before the procedure. This will depend on what type of anesthesia you will have.
- Take the medicines your surgeon told you to take with a small sip of water.
- You will be told when to arrive at the hospital or clinic. Be sure to arrive on time.
After the Procedure
Most people can go home soon after the procedure. It may take up to a month before the injection fully works.
It may become harder to empty your bladder. You may need to use a catheter for a few days. This and any other urinary problems usually go away.
Outlook (Prognosis)
You may need 2 or 3 more injections to get good results. If the material moves away from the spot where it was injected, you may need more treatments in the future.
Implants can help most men who have had transurethral resection of the prostate (TURP). Implants help about one half of men who have had their prostate gland removed to treat prostate cancer.
TURP
Transurethral resection of the prostate (TURP) is a surgery to remove the inside part of the prostate gland. It is done in order to treat symptoms o...

References
Boone TB, Stewart JN, Martinez LM. Additional therapies for storage and emptying failure. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 127.
Kobashi KC, Vasavada S, Bloschichak A, et al. Updates to surgical treatment of female stress urinary incontinence (SUI): AUA/SUFU Guideline (2023). J Urol. 2023;209(6):1091-1098. PMID: 37096580 pubmed.ncbi.nlm.nih.gov/37096580/.
Lentz GM, Miller JL. Lower urinary tract function and disorders: physiology of micturition, voiding dysfunction, urinary incontinence, urinary tract infections, and painful bladder syndrome. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 21.
Review Date: 1/1/2025
Reviewed By: Kelly L. Stratton, MD, FACS, Associate Professor, Department of Urology, University of Oklahoma Health Sciences Center, Oklahoma City, OK. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


