Bowel retraining
Fecal incontinence exercises; Neurogenic bowel - bowel retraining; Constipation - bowel retraining; Obstipation - bowel retraining; Bowel incontinence - bowel retrainingA program of bowel retraining, Kegel exercises, or biofeedback therapy may be used by people to help improve their bowel movements.
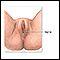
Kegel exercises
Pelvic floor muscle training exercises are a series of exercises designed to strengthen the muscles of the pelvic floor.
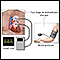
Biofeedback
Biofeedback is a technique that measures bodily functions and gives you information about them in order to help train you to control them.
Information
Problems that may benefit from bowel retraining include:
- Fecal incontinence, which is the loss of bowel control, causing you to pass stool unexpectedly and involuntarily. This can range from sometimes leaking a small amount of stool and passing gas, to not being able to control bowel movements.
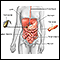
Fecal incontinence
Bowel incontinence is the loss of bowel control, causing you to unexpectedly pass stool. This can range from sometimes leaking a small amount of sto...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Severe constipation.
Constipation
Constipation in infants and children means they have hard stools or have problems passing stools. A child may have pain while passing stools or may ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
These problems may be caused by:
- Brain and nerve problems (such as from multiple sclerosis)
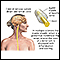
Multiple sclerosis
Multiple sclerosis (MS) is an autoimmune disease that affects the brain and spinal cord (central nervous system).
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Emotional problems
- Spinal cord damage
- Previous surgery
- Childbirth
- Overuse of laxatives
The bowel program includes several steps to help you have regular bowel movements. Most people are able to have regular bowel movements within a few weeks. Some people will need to use fiber supplements and laxatives along with bowel retraining. Your health care provider can tell you if you need to take laxatives and which ones are safe for you.
You will need a physical exam before you start a bowel training program. This will allow your provider to find the cause of the fecal incontinence or constipation. Disorders that can be corrected such as fecal impaction or infectious diarrhea can be treated at that time. The provider will use your history of bowel habits and lifestyle as a guide for setting new bowel movement patterns.
Fecal impaction
A fecal impaction is a large lump of dry, hard stool that stays stuck in the rectum. It is most often seen in people who are constipated for a long ...

Infectious diarrhea
Bacterial gastroenteritis occurs when there is a bacterial infection of your stomach or intestines.

DIET
Making the following changes to your diet will help you have regular, soft, bulky stools:
- Eat high-fiber foods such as whole-wheat grains, fresh vegetables, and beans.
Fiber
Fiber is a substance found in plants. Dietary fiber, which is the type of fiber you can eat, is found in fruits, vegetables, and grains. It is an i...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Use products containing psyllium, such as Metamucil, to add bulk to the stools.
- Try to drink 2 to 3 liters of fluid a day (unless you have a medical condition that requires you to restrict your fluid intake).
BOWEL TRAINING
You can use digital stimulation to trigger a bowel movement:
- Insert a lubricated finger into the anus. Move it in a circle until the sphincter muscle relaxes. This may take a few minutes.
- After you have done the stimulation, sit in a normal position for a bowel movement. If you are able to walk, sit on the toilet or bedside commode. If you are confined to the bed, use a bedpan. Get into as close to a sitting position as possible. If you are unable to sit, lie on your left side.
- Try to get as much privacy as you can. Some people find that reading while sitting on the toilet helps them relax.
- If you do not have a bowel movement within 20 minutes, repeat the process.
- Try to contract the muscles of the abdomen and bear down while releasing the stool. You may find it helpful to bend forward while bearing down. This increases the pressure within the abdomen and helps empty the bowel. Many people find it helpful to put a foot stool in front of the toilet to rest their feet.
- Perform stimulation with your finger every day until you start to have a regular pattern of bowel movements. If this is recommended, your provider or physical therapist will explain it to you. It is important to avoid trauma to the anus if you are performing stimulation.
- You can also stimulate bowel movements by using a suppository (glycerin or bisacodyl) or a small enema. Some people find it helpful to drink warm prune juice or fruit nectar.
Keeping to a regular pattern is very important for a bowel retraining program to succeed. Set a regular time for daily bowel movements. Choose a time that is convenient for you. Keep in mind your daily schedule. The best time for a bowel movement is 20 to 40 minutes after a meal, because eating stimulates bowel activity.
Most people are able to establish a regular routine of bowel movements within a few weeks.
KEGEL EXERCISES
Exercises to strengthen the pelvic and rectal muscles may help with bowel control in people who have incompetent anal sphincters. Kegel exercises that increase pelvic and rectal muscle tone can be used for this. These exercises were first developed to control incontinence in women after childbirth.
To be successful with Kegel exercises, use the proper technique and stick to a regular exercise program. Talk with your provider for instructions about how to do these exercises.
BIOFEEDBACK
Biofeedback gives you sound or visual feedback about a bodily function. In people with fecal incontinence, biofeedback is used to strengthen the anal sphincters.
A rectal probe is used to detect the strength of the rectal muscles. A monitoring electrode is placed on the abdomen. The rectal probe is then attached to a computer monitor. A graph displaying rectal muscle contractions and abdominal contractions will show up on the screen.
To use this method, you will be taught how to squeeze the rectal muscle around the rectal plug. The computer display guides you to make sure you are doing it correctly. Your symptoms should begin to improve after 3 sessions.
References
Camilleri M. Disorders of gastrointestinal motility. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 122.
Deutsch JK, Hass DJ. Complementary, alternative, and integrative medicine. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 131.
Iturrino JC, Lembo AJ. Constipation. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 19.
Pardi DS, Cotter TG. Other diseases of the colon. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 128.
Review Date: 8/12/2024
Reviewed By: Jenifer K. Lehrer, MD, Gastroenterologist, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.

