Pleural fluid analysis
Pleural fluid analysis is a test that examines a sample of fluid that has collected in the pleural space. This is the space between the lining of the outside of the lungs (pleura) and the wall of the chest. When fluid collects in the pleural space, the condition is called pleural effusion.
Pleural effusion
A pleural effusion is a buildup of fluid between the layers of tissue that line the lungs and chest cavity.

How the Test is Performed
A procedure called thoracentesis is used to get a sample of pleural fluid. Your health care provider tests the sample to look for:
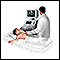
Thoracentesis
Thoracentesis is a procedure to remove fluid from the space between the lining of the outside of the lungs (pleura) and the wall of the chest....
Read Article Now Book Mark Article- Cancerous (malignant) cells
- Other types of cells (for example blood cells)
- Levels of glucose, protein and other chemicals
- Bacteria, fungi, mycobacteria, viruses, and other germs that can cause infections
- Inflammation
How to Prepare for the Test
No special preparation is needed before the test. An ultrasound, CT scan, or chest x-ray will be performed before and after the test.
Ultrasound
Ultrasound uses high-frequency sound waves to make images of organs and structures inside the body.
CT scan
A chest CT (computed tomography) scan is an imaging method that uses x-rays to create cross-sectional pictures of the chest and upper abdomen....

Chest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
Do not cough, breathe deeply, or move during the test to avoid injury to the lung.
Tell your provider if you take medicines to thin the blood.
How the Test will Feel
For thoracentesis, you sit on the edge of a chair or bed with your head and arms resting on a table. Your provider cleans your skin around the insertion site. Numbing medicine (anesthetic) is injected into your skin.
A needle is placed through the skin and muscles of your chest wall into the pleural space. As fluid drains into a collection bottle, you may cough a bit. This is because your lung re-expands to fill the space where fluid had been. This sensation may last for a few hours after the test.
During the test, tell your provider if you have sharp chest pain or shortness of breath.
Ultrasound is often used to decide where to insert the needle and to get a better view of the fluid in your chest.
Why the Test is Performed
The test is performed to determine the cause of a pleural effusion. It is also done to relieve the shortness of breath that a large pleural effusion can cause.
Normal Results
Normally the pleural space contains less than 20 milliliters (4 teaspoons) of clear, yellowish (serous) fluid.
What Abnormal Results Mean
Abnormal results may indicate possible causes of pleural effusion, such as:
- Cancer
- Cirrhosis
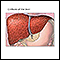
Cirrhosis
Cirrhosis is scarring of the liver and poor liver function. It is the last stage of chronic liver disease.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Heart failure
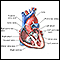
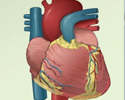
Heart failure
Heart failure is a condition in which the heart is no longer able to pump oxygen-rich blood to the rest of the body efficiently. This causes symptom...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Infection
- Severe malnutrition
Malnutrition
Malnutrition is the condition that occurs when your body does not get enough nutrients.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Very low protein (albumin) in the blood
- Trauma
- Abnormal connections between the pleural space and other organs (for example, the esophagus)
If your provider suspects an infection, a culture of the fluid is done to check for bacteria and other microbes.
Culture of the fluid
Pleural fluid culture is a test that examines a sample of fluid that has been collected in the pleural space to see if you have an infection to help ...
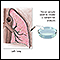
The test may also be performed for hemothorax. This is a collection of blood in the pleura.
Hemothorax
Hemothorax is a collection of blood in the space between the chest wall and the lung (the pleural cavity).

Risks
Risks of thoracentesis are:
- Collapsed lung (pneumothorax)
Pneumothorax
A collapsed lung occurs when air escapes from the lung. The air then fills the space outside of the lung between the lung and chest wall. This buil...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Excessive loss of blood
- Fluid re-accumulation
- Infection
- Pulmonary edema
Pulmonary edema
Pulmonary edema is an abnormal buildup of fluid in the lungs. This buildup of fluid leads to shortness of breath.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Respiratory distress
Respiratory distress
Acute respiratory distress syndrome (ARDS) is a life-threatening lung condition that prevents enough oxygen from getting to the lungs and into the bl...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Cough that doesn't go away
Serious complications are uncommon.
Reviewed By
Denis Hadjiliadis, MD, MHS, Paul F. Harron Jr. Professor of Medicine, Pulmonary, Allergy, and Critical Care, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Blok BK. Thoracentesis. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts & Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 9.
Broaddus VC, Light RW. Pleural effusion. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 108.

 All rights reserved.
All rights reserved.