Reye syndrome
Reye's syndromeReye syndrome is characterized by sudden (acute) brain damage and liver function problems. This condition does not have a known cause.
This syndrome has occurred in children who were given aspirin when they had chickenpox or the flu. Reye syndrome has become very rare. This is because aspirin is no longer recommended for routine use in children.
Causes
There is no known cause of Reye syndrome. It is most often seen in children ages 4 to 12. Most cases that occur with chickenpox are in children ages 5 to 9. Cases that occur with the flu are most often in children ages 10 to 14.
Symptoms
Children with Reye syndrome get sick very suddenly. The syndrome often begins with vomiting. It may last for many hours. The vomiting is quickly followed by irritable and aggressive behavior. As the condition gets worse, the child may be unable to stay awake and alert.
Other symptoms of Reye syndrome:
- Confusion
Confusion
Confusion is the inability to think as clearly or quickly as you normally do. You may feel disoriented and have difficulty paying attention, remembe...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Lethargy
Lethargy
Fatigue is a feeling of weariness, tiredness, or lack of energy.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Loss of consciousness or coma
- Mental changes
- Nausea and vomiting
- Seizures
Seizures
A seizure is the physical changes in behavior that occurs during an episode of specific types of abnormal electrical activity in the brain. The term ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Unusual placement of arms and legs (decerebrate posture). The arms are extended straight and turned toward the body, the legs are held straight, and the toes are pointed downward
Decerebrate posture
Decerebrate posture is an abnormal body posture that involves the arms and legs being held straight out, the toes being pointed downward, and the hea...
Read Article Now Book Mark Article
Other symptoms that can occur with this disorder include:
- Double vision
Double vision
There are many types of eye problems and vision disturbances, such as: Halos Blurred vision (the loss of sharpness of vision and the inability to see...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Hearing loss
Hearing loss
Hearing loss is being partly or totally unable to hear sound in one or both ears.
 ImageRead Article Now Book Mark Article
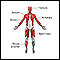
ImageRead Article Now Book Mark Article - Muscle function loss or paralysis of the arms or legs
Muscle function loss
Muscle function loss is when a muscle does not work or move normally. The medical term for complete loss of muscle function is paralysis.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Speech difficulties
- Weakness in the arms or legs
Exams and Tests
The following tests may be used to diagnose Reye syndrome:
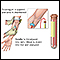
- Blood chemistry tests
Blood chemistry tests
A comprehensive metabolic panel is a group of blood tests. They provide an overall picture of your body's chemical balance and metabolism. Metaboli...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Head CT or head MRI scan
Head CT
A head computed tomography (CT) scan uses many x-rays to create pictures of the head, including the skull, brain, eye sockets, and sinuses.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleHead MRI scan
A head MRI (magnetic resonance imaging) is an imaging test that uses powerful magnets and radio waves to create pictures of the brain and surrounding...
 ImageRead Article Now Book Mark Article
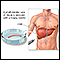
ImageRead Article Now Book Mark Article - Liver biopsy
Liver biopsy
A liver biopsy is a test that takes a sample of tissue from the liver for examination.
 ImageRead Article Now Book Mark Article
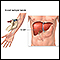
ImageRead Article Now Book Mark Article - Liver function tests
Liver function tests
Liver function tests are common tests that are used to see how well the liver is working. Tests include:AlbuminAlpha-1 antitrypsinAlkaline phosphata...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Serum ammonia test
Serum ammonia test
The ammonia test measures the level of ammonia in a blood sample.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Spinal tap
Spinal tap
Cerebrospinal fluid (CSF) collection is a test to look at the fluid that surrounds the brain and spinal cord. CSF acts as a cushion, protecting the b...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Treatment
There is no specific treatment for this condition. The health care provider will monitor the pressure in the brain, blood gases, and blood acid-base balance (pH).
Blood gases
Blood gases are a measurement of how much oxygen and carbon dioxide are in your blood. They also determine the acidity (pH) of your blood.

Treatments may include:
- Breathing support (a breathing machine may be needed during a deep coma)
- Fluids by IV to provide electrolytes and glucose
Electrolytes
Electrolytes are minerals in your blood and other body fluids that carry an electric charge. Electrolytes affect how your body functions in many ways...
Read Article Now Book Mark Article - Steroids to reduce swelling in the brain
Swelling
Swelling is the enlargement of organs, skin, or other body parts. It is caused by a buildup of fluid in the tissues. The extra fluid can lead to a ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Outlook (Prognosis)
How well a person does depends on the severity of any coma, as well as other factors.
The outcome for those who survive an acute episode may be good.
Acute
Acute means sudden. Acute symptoms appear, change, or worsen rapidly. It is the opposite of chronic.
Possible Complications
Complications may include:
- Coma
- Permanent brain damage
- Seizures
Seizures
A seizure is the physical changes in behavior that occurs during an episode of specific types of abnormal electrical activity in the brain. The term ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
When untreated, seizures and coma may be life threatening.
When to Contact a Medical Professional
Go to the emergency room or call the local emergency number (such as 911) immediately if your child has:
- Confusion
- Lethargy
- Other mental changes
Prevention
Never give a child aspirin unless told to do so by your child's provider.
When a child must take aspirin for a medical condition, take care to reduce the child's risk of catching a viral illness, such as the flu and chickenpox. Avoid aspirin for several weeks after the child has received a varicella (chickenpox) vaccine.
Note: Other over-the-counter medicines, such as Pepto-Bismol and substances with oil of wintergreen also contain aspirin-like compounds called salicylates. DO NOT give these to a child who has a cold or fever.
References
Aronson JK. Acetylsalicylic acid. In: Aronson JK, ed. Meyler's Side Effects of Drugs. 16th ed. Waltham, MA: Elsevier B.V.; 2016:26-52.
Barkoudah E. Encephalopathies. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 638.
Cherry JD. Reye syndrome. In: Cherry JD, Harrison GJ, Kaplan SL, Steinbach WJ, Hotez PJ, eds. Feigin and Cherry's Textbook of Pediatric Infectious Diseases. 8th ed. Philadelphia, PA: Elsevier; 2019:chap 50.
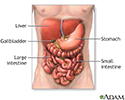
Digestive system organs - illustration
The digestive system organs in the abdominal cavity include the liver, gallbladder, stomach, small intestine and large intestine.
Digestive system organs
illustration
Review Date: 7/16/2024
Reviewed By: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.