Ganglioneuroma
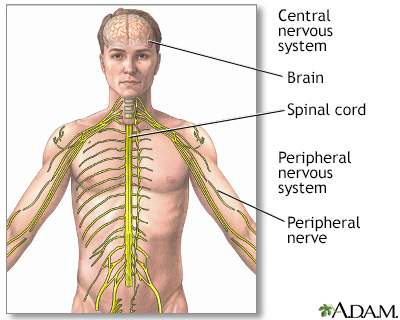
Ganglioneuroma is a tumor of the autonomic nervous system.
Causes
Ganglioneuromas are rare tumors that most often start in autonomic nerve cells. Autonomic nerves manage body functions such as blood pressure, heart rate, sweating, bowel and bladder emptying, and digestion. The tumors are usually noncancerous (benign).
Benign
Benign refers to a condition, tumor, or growth that is not cancerous. This means that it does not spread to other parts of the body. It does not in...
Ganglioneuromas usually occur in people over 10 years of age. They grow slowly, and may release certain chemicals or hormones.
There are no known risk factors. However, the tumors may be associated with some genetic problems, such as neurofibromatosis type 1.
Neurofibromatosis type 1
Neurofibromatosis-1 (NF1) is an inherited disorder in which nerve tissue tumors (neurofibromas) form in the:Upper and lower layers of the skinNerves ...
Symptoms
A ganglioneuroma usually causes no symptoms. The tumor is only discovered when a person is examined or treated for another condition.
Symptoms depend on the location of the tumor and the type of chemicals it releases.
If the tumor is in the chest area (mediastinum), symptoms may include:
- Breathing difficulty
- Chest pain
Chest pain
Chest pain is discomfort or pain that you feel anywhere along the front of your body between your neck and upper abdomen.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Compression of the windpipe (trachea)
If the tumor is lower down in the abdomen in the area called the retroperitoneal space, symptoms may include:
- Abdominal or back pain
- Bloating
If the tumor is near the spinal cord, it may cause:
- Compression of the spinal cord, which leads to pain and loss of strength or feeling in the legs, arms, or both
- Spine deformity
These tumors may produce certain hormones, which can cause the following symptoms:
- Diarrhea
- High blood pressure
- Increased body hair
Exams and Tests
The best tests to identify a ganglioneuroma are:
- CT scan of the chest, abdomen, and pelvis
CT scan
A computed tomography (CT) scan is an imaging method that uses x-rays to create pictures of cross-sections of the body. Related tests include:Abdomin...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - MRI scan of the chest and abdomen
MRI scan
A magnetic resonance imaging (MRI) scan is an imaging test that uses powerful magnets and radio waves to create pictures of the body. It does not us...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Ultrasound of the abdomen or pelvis
Ultrasound of the abdomen or pelvis
Abdominal ultrasound is a type of imaging test. It is used to look at organs in the abdomen, including the liver, gallbladder, pancreas, and kidneys...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Blood and urine tests may be done to determine if the tumor is producing hormones or other chemicals.
A biopsy or complete removal of the tumor may be needed to confirm the diagnosis.
Biopsy
A biopsy is the removal of a small piece of tissue for lab examination.
Treatment
Treatment involves surgery to remove the tumor (if it is causing symptoms).
Outlook (Prognosis)
Most ganglioneuromas are noncancerous. The expected outcome is usually good.
Possible Complications
If the tumor has been present for a long time and has pressed on the spinal cord or caused other symptoms, surgery to remove the tumor may not reverse the damage. Compression of the spinal cord may result in loss of movement (paralysis), especially if the cause is not detected promptly.
Surgery to remove the tumor may also lead to complications in some cases. In rare cases, problems due to compression may occur even after the tumor is removed.
When to Contact a Medical Professional
Contact your health care provider if you or your child has symptoms that may be caused by this type of tumor.
Reviewed By
Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Goldblum JR, Folpe AL, Weiss SW. Benign tumors of peripheral nerves. In: Goldblum JR, Folpe AL, Weiss SW, eds. Enzinger and Weiss's Soft Tissue Tumors. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 26.
Kaidar-Person O, Zagar T, Haithcock BE, Weiss J. Diseases of the pleura and mediastinum. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 70.
Kutikov A, Crispen PL, Uzzo RG. Pathophysiology, evaluation, and medical management of adrenal disorders. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 106.
 All rights reserved.
All rights reserved.