Chlamydial infections - male
STD - chlamydia male; Sexually transmitted disease - chlamydia male; Urethritis - chlamydiaChlamydia infection in males is usually an infection of the urethra. The urethra is the tube that drains urine from the bladder. It passes through the penis. This type of infection is passed from one person to another during sexual contact.
Related topics are:
- Chlamydia
Chlamydia
Chlamydia is an infection caused by the bacteria Chlamydia trachomatis. It is most often spread through sexual contact.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Chlamydia infections in women
Chlamydia infections in women
Chlamydia is an infection that can be passed from one person to another through sexual contact. This type of infection is known as sexually transmit...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Causes
Chlamydia infection is caused by the bacteria Chlamydia trachomatis. Both males and females may have chlamydia without having any symptoms. As a result, you may become infected or pass the infection to your partner without knowing it.
You are more likely to become infected with chlamydia if you:
- Have sex without wearing a male or female condom
- Have more than one sexual partner
- Use drugs or alcohol and then have sex
Symptoms
Some common symptoms are:
- Difficulty urinating, which includes painful urination or burning during urination
Painful urination
Painful urination is any pain, discomfort, or burning sensation when passing urine.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Discharge from the penis
- Redness, swelling, or itching of the opening of the urethra at the tip of the penis
- Swelling and tenderness of one or both testicles
Chlamydia and gonorrhea often occur together. The symptoms of chlamydia infection may be similar to symptoms of gonorrhea, but they continue even after treatment for gonorrhea is finished.
Gonorrhea
Gonorrhea is a common sexually transmitted infection (STI).
Read Article Now Book Mark ArticleExams and Tests
If you have symptoms of a chlamydia infection, your health care provider may suggest a lab test called PCR. Your provider will take a sample of discharge from the penis. This discharge is sent to a lab to be tested. Results will take 1 to 2 days to come back. Alternatively, your provider may collect a urine sample for a test called nucleic acid amplification.
Your provider may also check you for other types of infections, such as gonorrhea, syphilis, and HIV.
Syphilis
Syphilis is a bacterial infection that is most often spread through sexual contact.
HIV
Human immunodeficiency virus (HIV) is the virus that causes acquired immunodeficiency syndrome (AIDS). When a person becomes infected with HIV, the ...

Men who do not have symptoms of a chlamydia infection may sometimes be tested.
Treatment
Chlamydia can be treated with a variety of antibiotics. Common side effects of these antibiotics are:
- Nausea
- Upset stomach
- Diarrhea
You and your sexual partner must be treated to avoid passing the infections back and forth. Even partners without symptoms need to be treated. You and your partner should finish all of the antibiotics, even if you feel better.
Because gonorrhea often occurs with chlamydia, treatment for gonorrhea is often given at the same time.
Outlook (Prognosis)
Treatment with antibiotics is almost always successful. If your symptoms do not improve quickly, make sure you are also being treated for gonorrhea and other infections spread through sexual contact.
Severe infections or infections that are not treated quickly may rarely cause scarring of the urethra. This problem can make it harder to pass urine and may require surgery.
When to Contact a Medical Professional
Contact your provider if you have symptoms of a chlamydia infection.
Prevention
To prevent infection, practice safer sex. This means taking steps before and during sex that can help prevent you from getting an infection, or from giving one to your partner.
Safer sex
Safe sex means taking steps before and during sex that can prevent you from getting an infection, or from giving an infection to your partner. These...
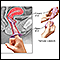
Before having sex:
- Get to know your partner and discuss your sexual histories.
- Don't feel forced into having sex.
- Don't have sexual contact with anyone but your partner.
Be sure that your sexual partner does not have any sexually transmitted infection (STI). Before having sex with a new partner, each of you should get screened for STIs. Share the test results with each other.
If you have an STI such as HIV or herpes, let any sexual partner know before you have sex. Allow them to decide what to do. If you both agree to have sexual contact, use latex or polyurethane condoms.
Remember to:
- Use condoms for all vaginal, anal, and oral intercourse.
- Make sure that the condom is in place from the beginning to the end of the sexual activity. Use it every time you have sex.
- Keep in mind that STIs can be spread by contact with surrounding skin areas. A condom reduces your risk but does not fully eliminate it.
Other tips include:
- Use lubricants. They may help reduce the chance that a condom will break.
- Use only water-based lubricants. Oil-based or petroleum-type lubricants can cause latex to weaken and tear.
- Polyurethane condoms are less prone to breaking than latex condoms, but they cost more.
- Using condoms with nonoxynol-9 (a spermicide) may irritate vaginal or penile tissue and thus increase the chance of HIV transmission.
- Stay sober. Alcohol and drugs impair your judgment. When you are not sober, you might not choose your partner as carefully. You may also forget to use condoms, or use them incorrectly.
References
Babu TM, Urban MA, Augenbraun MH. Urethritis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 107.
Reno HEL, Geisler WM. Diseases caused by chlamydiae. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 294.
Swygard H, Cohen MS. Approach to the patient with a sexually transmitted infection. In: Goldman L, Cooney KA, eds. Goldman- Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 264.
Workowski KA, Bachmann LH, Chan PA, et al. Sexually transmitted infections treatment guidelines, 2021. MMWR Recomm Rep. 2021;70(4):1-187. PMID: 34292926 pubmed.ncbi.nlm.nih.gov/34292926/.
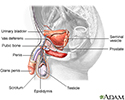
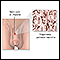
Male reproductive anatomy - illustration
The male reproductive structures include the penis, the scrotum, the testicles (testes), the epididymis, the seminal vesicles, and the prostate.
Male reproductive anatomy
illustration
Review Date: 4/18/2024
Reviewed By: Linda J. Vorvick, MD, Clinical Professor, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.