Disseminated tuberculosis
Disseminated tuberculosis is a mycobacterial infection in which mycobacteria spread from the lungs to other parts of the body through the blood or lymph system.
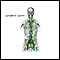
Lymph system
The lymph system is a network of organs, lymph nodes, lymph ducts, and lymph vessels that make and move lymph from tissues to the bloodstream. The l...
Causes
Tuberculosis (TB) infection can develop after breathing in droplets sprayed into the air from a cough or sneeze by someone infected with the Mycobacterium tuberculosis bacterium. The resulting lung infection is called primary TB.
The usual site of TB is the lungs (pulmonary TB), but other organs can be involved. In the United States, most people with primary TB get better and have no further evidence of disease. Disseminated TB develops in a small number of infected people whose immune systems do not successfully contain the primary infection.
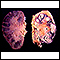
Pulmonary TB
Pulmonary tuberculosis (TB) is a contagious bacterial infection that involves the lungs. It may spread to other organs.
Disseminated disease can occur within weeks of the primary infection. Sometimes, it occurs years after you become infected. You are more likely to get this type of TB if you have a weakened immune system due to disease (such as AIDS) or certain medicines. Infants and older adults are also at higher risk.
Your risk of catching TB increases if you:
- Are around people who have the disease (such as during overseas travel)
- Live in crowded or unclean conditions
- Are immunocompromised by a disease or medicines
- Have poor nutrition
The following factors can increase the rate of TB infection in a population:
- Increase in HIV infections
- Increase in number of homeless people with unstable housing (poor environment and nutrition)
- The appearance of drug-resistant strains of TB
Symptoms
Disseminated tuberculosis can affect many different body areas. Symptoms depend on the affected areas of the body and can include:
- Abdominal pain or swelling
Abdominal pain
Abdominal pain is pain that you feel anywhere between your chest and groin. This is often referred to as the stomach region or belly.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleSwelling
Swelling is the enlargement of organs, skin, or other body parts. It is caused by a buildup of fluid in the tissues. The extra fluid can lead to a ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Chills
- Cough and shortness of breath
- Fatigue
- Fever
- General discomfort, uneasiness, or ill feeling (malaise)
Malaise
Malaise is a general feeling of discomfort, illness, or lack of well-being.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Joint pain
- Pale skin due to anemia (pallor)
Pallor
Paleness is an abnormal loss of color from normal skin or mucous membranes.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Sweating
- Swollen glands
Swollen glands
Lymph nodes are present throughout your body. They are an important part of your immune system. Lymph nodes help your body recognize and fight germ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Weight loss
Exams and Tests
Your health care provider will perform a physical exam. This may show:
- Swollen liver
Swollen liver
Enlarged liver refers to swelling of the liver beyond its normal size. Hepatomegaly is another word to describe this problem. If both the liver and ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Swollen lymph nodes
Swollen lymph nodes
Lymph nodes are present throughout your body. They are an important part of your immune system. Lymph nodes help your body recognize and fight germ...
 ImageRead Article Now Book Mark Article
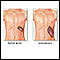
ImageRead Article Now Book Mark Article - Swollen spleen
Swollen spleen
Splenomegaly is a larger-than-normal spleen. The spleen is an organ in the upper left part of the belly.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Tests that may be ordered include:
- Biopsies and cultures of affected organs or tissues
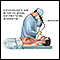
- Bronchoscopy for biopsy or culture
Bronchoscopy
Bronchoscopy is a test to view the airways and diagnose lung disease. It may also be used during the treatment of some lung conditions.
 ImageRead Article Now Book Mark Article
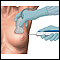
ImageRead Article Now Book Mark ArticleBiopsy
A biopsy is the removal of a small piece of tissue for lab examination.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Chest x-ray
Chest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - CT scan of the affected area
CT scan
A computed tomography (CT) scan is an imaging method that uses x-rays to create pictures of cross-sections of the body. Related tests include:Abdomin...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Fundoscopy to check for retinal lesions
- Interferon-gamma release blood test, such as the QFT-Gold test to test for prior exposure to TB
- Lung biopsy
Lung biopsy
An open lung biopsy is surgery to remove a small piece of tissue from the lung. The sample is then examined for cancer, infection, or lung disease....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Mycobacterial culture of bone marrow or blood
- Pleural biopsy
- Tuberculin skin test (PPD test)
Tuberculin skin test
The PPD skin test is a method used to diagnose silent (latent) tuberculosis (TB) infection. PPD stands for purified protein derivative.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Sputum examination and cultures
Cultures
Routine sputum culture is a laboratory test that looks for germs that cause infection. Sputum is the material that comes up from air passages when y...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Thoracentesis
Thoracentesis
Thoracentesis is a procedure to remove fluid from the space between the lining of the outside of the lungs (pleura) and the wall of the chest....
Read Article Now Book Mark Article
Treatment
The goal of treatment is to cure the infection with medicines that fight the TB bacteria. Treatment of disseminated TB involves a combination of several medicines (usually 4). All medicines are continued until lab tests show which work best.
You may need to take many different pills for 6 months or longer. It is very important that you take the pills the way your provider instructs.
When people do not take their TB medicines as instructed, the infection can become much more difficult to treat. The TB bacteria can become resistant to treatment. This means the medicines no longer work.
When there is concern that a person may not take all the medicines as directed, a provider may need to watch the person take the prescribed medicines. This approach is called directly observed therapy. In this case, medicines may be given 2 or 3 times a week, as prescribed by a provider.
You may need to stay at home or be admitted to a hospital for 2 to 4 weeks to avoid spreading the disease to others until you are no longer contagious.
Your provider may be required by law to report your TB illness to the local health department. Your health care team will ensure that you receive the best care.
Outlook (Prognosis)
Most forms of disseminated TB respond well to treatment. The tissue that is affected, such as the bones or joints, may have permanent damage due to the infection.
Possible Complications
Complications of disseminated TB can include:
- Acute respiratory distress syndrome (ARDS)
ARDS
Acute respiratory distress syndrome (ARDS) is a life-threatening lung condition that prevents enough oxygen from getting to the lungs and into the bl...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Liver inflammation
Liver inflammation
Hepatitis is swelling and inflammation of the liver.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Lung failure
- Return of the disease
Medicines used to treat TB can cause side effects, including:
- Changes in vision
- Orange- or brown-colored tears and urine
- Rash
- Liver inflammation
Liver inflammation
Drug-induced liver injury (DILI) is an injury of the liver that may occur when you take certain medicines. Other types of liver injury include:Viral ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
A vision test may be done before treatment so your provider can monitor any changes in the health of your eyes.
When to Contact a Medical Professional
Contact your provider if you know or suspect that you have been exposed to TB. All forms of TB and exposure need prompt evaluation and treatment.
Prevention
TB is a preventable disease, even in those who have been exposed to an infected person. Skin testing for TB is used in high-risk populations or in people who may have been exposed to TB, such as health care workers.
People who have been exposed to TB should be skin tested immediately and have a follow-up test at a later date, if the first test is negative.
A positive skin test means you have come into contact with the TB bacteria. It does not mean that you have active disease or are contagious. Talk to your provider about how to prevent developing active disease.
Prompt treatment is extremely important in controlling the spread of TB from those who have active TB disease to those who have never been infected with TB.
Some countries with a high incidence of TB give people a vaccination (called BCG) to prevent TB. The effectiveness of this vaccine is limited and it is not routinely used in the United States.
People who have had BCG may still be skin tested for TB. Discuss the test results (if positive) with your provider.
Reviewed By
Jatin M. Vyas, MD, PhD, Associate Professor in Medicine, Harvard Medical School; Associate in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Bailey TC, Philips JA. Tuberculosis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 299.
Centers for Disease Control and Prevention website. Tuberculosis (TB). www.cdc.gov/tb/. Accessed June 18, 2024.
Fitzgerald DW, Sterling TR, Haas DW. Mycobacterium tuberculosis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 249.





 All rights reserved.
All rights reserved.