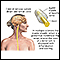
Compression fractures of the back
Vertebral compression fractures; Osteoporosis - compression fractureCompression fractures of the back are broken vertebrae. Vertebrae are the bones of the spine.
Causes
Osteoporosis is the most common cause of this type of fracture. Osteoporosis is a disease in which bones become fragile. In most cases, bone loses calcium and other minerals with age. Other causes of compression fractures may include:
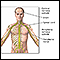
Osteoporosis
Osteoporosis is a disease in which bones become fragile and more likely to break (fracture).

- Trauma to the back
- Tumors that spread to the bone from elsewhere
- Tumors that start in the spine, such as multiple myeloma
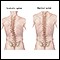
Having many fractures of the vertebrae can lead to kyphosis. This is a hump-like curvature of the spine.
Kyphosis
Kyphosis is a curving of the spine that causes a bowing or rounding of the back. This leads to a hunchback or slouching posture.

Symptoms
Compression fractures can occur suddenly. This can cause severe back pain.
- The pain is most commonly felt in the middle or lower spine. It can also be felt on the sides or in the front of the spine.
- The pain is often sharp and "knife-like." Pain can be disabling, and take weeks to months to go away.
Compression fractures due to osteoporosis may cause no symptoms at first. Often, they are discovered when x-rays of the spine are done for other reasons. Over time, the following symptoms may occur:
- Back pain that starts slowly, and gets worse with walking, but is not felt when resting
- Loss of height, as much as 6 inches (15 centimeters) over time
- Stooped-over posture, or kyphosis, also called a dowager's hump
Pressure on the spinal cord from hunched over posture can, in rare cases, cause:
- Numbness
Numbness
Numbness and tingling are abnormal sensations that can occur anywhere in your body, but they are often felt in your fingers, hands, feet, arms, or le...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Tingling
Tingling
Numbness and tingling are abnormal sensations that can occur anywhere in your body, but they are often felt in your fingers, hands, feet, arms, or le...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Weakness
- Difficulty walking
- Loss of control of the bowel or bladder
Exams and Tests
Your health care provider will perform a physical exam. This may show:
- A humpback, or kyphosis
- Tenderness over the affected spinal bone or bones
- Loss of height
A spine x-ray may show at least 1 compressed vertebra that is shorter than the other vertebrae.
Spine x-ray
A thoracic spine x-ray is an x-ray of the 12 chest (thoracic) bones (vertebrae) of the spine. The vertebrae are separated by flat pads of cartilage ...

Other tests that may be done include:
- A bone density test to evaluate for osteoporosis
- A CT or MRI scan, if there is a concern that the fracture was caused by a tumor or severe trauma (such as a fall or car accident) or if there are symptoms of nerve damage
Treatment
Most compression fractures are seen in older people with osteoporosis. These fractures often do not cause injury to the spinal cord. The condition is usually treated with medicines and calcium supplements to prevent further fractures.
Pain may be treated with:
- Pain medicine
- Bed rest
Other treatments may include:
- Back braces, but these may further weaken the bones and increase the risk for more fractures
- Physical therapy to improve movement and strength around the spine
- A medicine called calcitonin to help relieve bone pain
Surgery may be done if you have severe and disabling pain for more than 2 months that does not get better with other treatments. Surgery can include:
- Balloon kyphoplasty
Balloon kyphoplasty
Kyphoplasty is used to treat painful compression fractures in the spine. In a compression fracture, all or part of a spine bone collapses. The proc...
Read Article Now Book Mark Article - Vertebroplasty
Vertebroplasty
Vertebroplasty is often an outpatient procedure used to treat painful compression fractures in the spine. In a compression fracture, all or part of ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Spinal fusion
Spinal fusion
Spinal fusion is surgery to permanently join together two or more bones in the spine so there is no movement between them. These bones are called ve...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Other surgery may be done to remove bone if the fracture is due to a tumor.
After surgery you may need:
- A brace for 6 to 10 weeks if the fracture was due to an injury.
- More surgery to join spine bones together or to relieve pressure on a nerve.
Outlook (Prognosis)
Most compression fractures due to injury heal in 8 to 10 weeks with rest, wearing of a brace, and pain medicines. However, recovery can take much longer if surgery was done. You will lose some height and have a more bent back.
Fractures due to osteoporosis often become less painful with rest and pain medicines. Some fractures, though, can lead to long-term (chronic) pain and disability.
Medicines to treat osteoporosis can help prevent future fractures. However, medicines cannot reverse damage that has already occurred.
For compression fractures caused by tumors, the outcome depends on the type of tumor involved. Tumors that involve the spine include:
- Breast cancer
- Lung cancer
- Lymphoma
- Prostate cancer
- Multiple myeloma
- Hemangioma
Possible Complications
Complications may include:
- Failure of the bones to fuse after surgery
- Humpback
- Spinal cord or nerve root compression
When to Contact a Medical Professional
Contact your provider if:
- You have back pain and you think you may have a compression fracture.
- Your symptoms are getting worse, or you have problems controlling your bladder and bowel function.
Prevention
Taking steps to prevent and treat osteoporosis is the most effective way to prevent compression or insufficiency fractures. Getting regular load-bearing exercise (such as walking) can help you avoid bone loss.
Prevent and treat osteoporosis
Osteoporosis, or weak bones, is a disease that causes bones to become brittle and more likely to fracture (break). With osteoporosis, the bones lose...

Women should have their bone density checked at age 65, or earlier if you are at increased risk for osteoporosis.
References
Abode-Iyamah K. Compression fracture with back pain. In: Chaichana KL, Quiñones-Hinojosa A, eds. Comparative Management of Spine Pathology. Philadelphia. PA: Elsevier; 2021:chap 24.
LeBoff MS, Greenspan SL, Insogna KL, et al. The clinician's guide to prevention and treatment of osteoporosis. Osteoporos Int. 2022;33(10):2049-2102. PMID: 35478046 pubmed.ncbi.nlm.nih.gov/35478046/.
Savage JW, Anderson PA. Osteoporotic spinal fractures. In: Browner BD, Jupiter JB, Krettek C, Anderson PA, eds. Skeletal Trauma: Basic Science, Management, and Reconstruction. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 35.
Waldman SD. Thoracic vertebral compression fracture. In: Waldman SD, ed. Atlas of Common Pain Syndromes. 4th ed. Philadelphia, PA: Elsevier; 2019:chap 73.
Williams KD. Fractures, dislocations, and fracture-dislocations of the spine. In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 41.
Compression fracture - illustration
In a compression fracture the body of the bone tissue of the vertebra collapses. This can occur because of trauma or a disease process such as osteoporosis or a tumor.
Compression fracture
illustration
- Back pain and sciatica - InDepth(In-Depth)
- Low back pain(Alt. Medicine)
Review Date: 8/12/2023
Reviewed By: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.