Diverticulitis
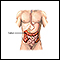
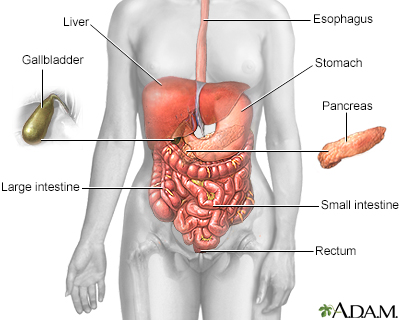
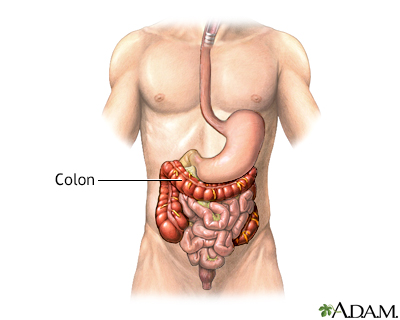
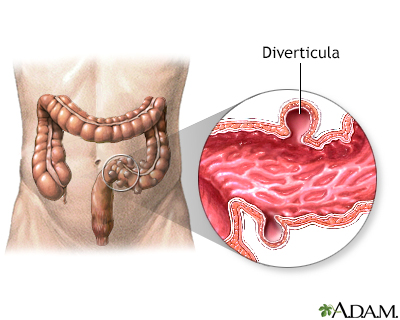
Diverticula are small, bulging sacs or pouches that form on the inner wall of the intestine. Diverticulitis occurs when these pouches become inflamed or infected. Most often, these pouches are in the lower part of the large intestine (colon).
Causes
The formation of pouches or sacs on the intestinal lining is called diverticulosis. It is found in more than half of Americans over age 60. However, no one knows exactly what causes the pouches to form.
Eating a low-fiber diet mostly made up of processed foods may be a cause. Constipation and hard stools are more likely when you do not eat enough fiber. Straining to pass stools increases the pressure in the colon or intestines, which may lead to the formation of these pouches.
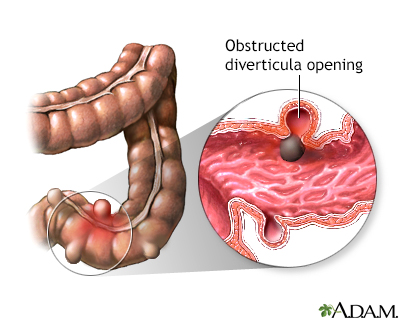
In some cases, one of the pouches can become inflamed and a small tear develops in the lining of the intestine. This can lead to an infection at the site. When this occurs, the condition is called diverticulitis. The cause of diverticulitis is not known.
Symptoms
People with diverticulosis often have no symptoms, but they may have bloating and cramping in the lower part of the belly. Rarely, they may notice blood in their stool or on toilet paper.
Diverticulosis
Diverticulosis occurs when small, bulging sacs or pouches form on the inner wall of the intestine. These sacs are called diverticula. Most often, t...
Symptoms of diverticulitis are more severe and often start suddenly, but they may become worse over a few days. They include:
- Pain or discomfort, usually in the left lower part of the abdomen
- Bloating or gas
- Fever and chills
- Nausea and vomiting
- Not feeling hungry and not eating
Exams and Tests
Your health care provider will examine you. This may show tenderness in the abdomen, especially in its left lower part. You may need blood tests to see if you have an infection.
Other tests that help diagnose diverticulitis may include:
- CT scan
CT scan
An abdominal CT scan is an imaging test that uses x-rays to create cross-sectional pictures of the belly area. CT stands for computed tomography....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Ultrasound of the abdomen
Ultrasound of the abdomen
Abdominal ultrasound is a type of imaging test. It is used to look at organs in the abdomen, including the liver, gallbladder, pancreas, and kidneys...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - X-rays of the abdomen
Treatment
The treatment of diverticulitis depends on how serious the symptoms are. Some people may need to be in the hospital, but often, the problem can be treated at home.
To help with the pain, your provider may suggest that you:
- Rest in bed and use a heating pad on your belly.
- Take pain medicines (ask your provider which ones you should use).
- Drink only fluids for a day or two, and then slowly begin drinking thicker liquids and then eating foods.
The provider may treat you with antibiotics.
After you are better, your provider may suggest that you add more fiber to your diet. Eating more fiber can help prevent future attacks. If you have bloating or gas, reduce the amount of fiber you eat for a few days.
Once these pouches have formed, you will have them for life. Diverticulitis can return, but some providers think a high-fiber diet may lessen your chances of a recurrence.
High-fiber diet
Fiber is a substance found in plants. Dietary fiber, the kind you eat, is found in fruits, vegetables, and grains. Your body cannot digest fiber, s...

Outlook (Prognosis)
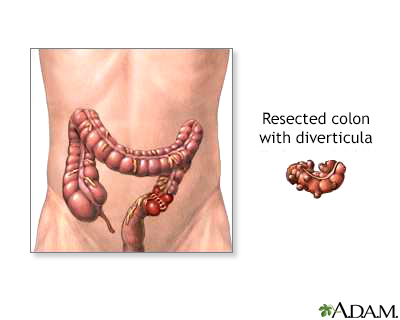
Most often, this is a mild condition that responds well to treatment. Some people will have more than one attack of diverticulitis. Surgery may be needed in some cases. Many times, providers will recommend that you have a colonoscopy after diverticulitis has healed. This can help to rule out other conditions that could mimic diverticulitis symptoms.
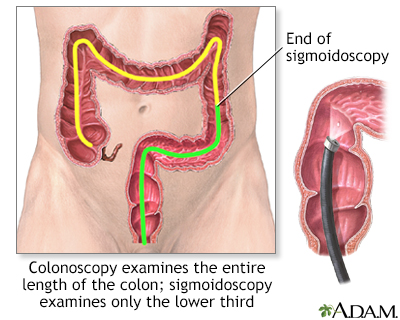
Colonoscopy
A colonoscopy is an exam that views the inside of the colon (large intestine) and rectum, using a tool called a colonoscope. The colonoscope has a sm...
Possible Complications
More serious problems that may develop are:
- Abnormal connections that form between parts of the colon or between the colon and another part of the body (fistula)
- Hole or tear in the colon (perforation)
- Narrowed area in the colon (stricture)
- Pocket filled with pus or infection (abscess)
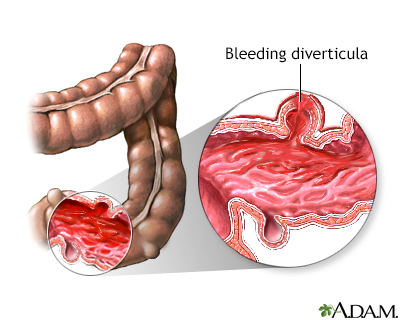
- Bleeding from the diverticula
When to Contact a Medical Professional
Contact your provider if symptoms of diverticulitis occur.
Also call if you have diverticulitis and you have:
- Blood in your stools
- Fever above 100.4°F (38°C) that does not go away
- Nausea, vomiting, or chills
- Sudden belly or back pain that gets worse or is very severe
Reviewed By
Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Bhuket TP, Stollman NH. Diverticular disease of the colon. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 121.
Kuemmerle JF. Inflammatory and anatomic diseases of the intestine, peritoneum, mesentery, and omentum. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 128.



 All rights reserved.
All rights reserved.