Unstable angina
Unstable angina is a condition in which your heart doesn't get enough blood flow and oxygen. It may lead to a heart attack.
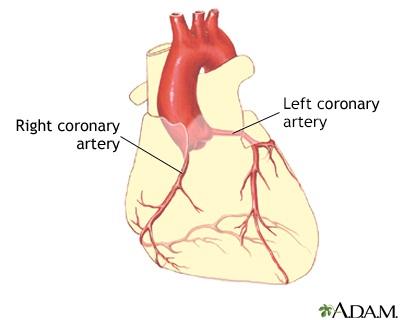
Angina is a type of chest discomfort due to poor blood flow through the blood vessels in the heart called the coronary arteries.
Angina
Angina is a type of chest discomfort or pain due to poor blood flow through the blood vessels (coronary arteries) of the heart muscle (myocardium). ...
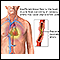
Angina causes and symptoms - Animation
Angina, or angina pectoris, is temporary chest pain or a sensation of pressure that occurs when the heart’s need for oxygen is not satisfied by the amount of blood supplied to the heart. Blood flow can be limited when the arteries are narrowed by atherosclerosis, or because of coronary artery spasms. Symptoms of angina may also include discomfort in the shoulders, inside the arms, through the back and in the throat, jaw, or teeth. Angina due to atherosclerosis usually occurs during physical exertion or emotional distress, or at rest if the artery is narrowed by more than 70%.
Causes
Heart attack - Animation
You feel a tight band of pain around your chest. The pain moves from your chest to your arms, shoulder, and neck. What could your pain mean? Could it be a heart attack, could it be the big one? Heart attacks are caused by interruption of blood supply to part of the heart. If the blood flow is blocked, your heart is starved of oxygen and heart cells die. A hard substance called plaque can build up in the walls of your coronary arteries. This plaque is made up of cholesterol and other cells. A heart attack can occur as a result of plaque buildup or the rupture of one of these plaques. We're not sure why heart attacks occur when they do. You may have a heart attack when you are resting or asleep, or after a sudden increase in physical activity, when you are outside in cold weather, or after a sudden, severe emotional or physical stress, including an illness. So, how is a heart attack treated? If you go to the hospital for a suspected heart attack, a doctor or nurse will listen to your chest with a stethoscope. You will have a blood test to look for heart damage. A coronary angiography test can show your doctor how well blood is moving through your heart. If blood moves slowly, or not at all through your coronary arteries, you have either a narrowed, or blocked artery. Other tests can look at the valves and chambers of your heart and check for abnormal heart rhythms. If you've had a heart attack, doctors can do an emergency procedure called angioplasty. This surgery or procedure can open narrowed or blocked blood vessels. Usually they'll place a small, metal mesh tube, called a stent, in your artery to help keep it open. You may also receive drugs to break up the clot in your artery. Sometimes, doctors will do heart bypass surgery to get blood flowing to your heart muscle again. After you are treated in the hospital for a heart attack, you may need to take medicines to thin your blood, to protect your heart, or to improve your cholesterol levels. You may need to take these medicines for the rest of your life. Most people who have had a heart attack also need cardiac rehabilitation. This will help you slowly increase your exercise level and learn how to follow a healthy lifestyle. After you have a heart attack, your chance of another is higher. How well you do after a heart attack depends on the damage to your heart and where the damage is, and what steps you take to prevent another one. If your heart can no longer pump blood to your body as well as it used to, you may have heart failure and will need lifelong treatment. Usually a person who has had a heart attack can slowly go back to normal activities, but you will need to take steps to prevent another heart attack.
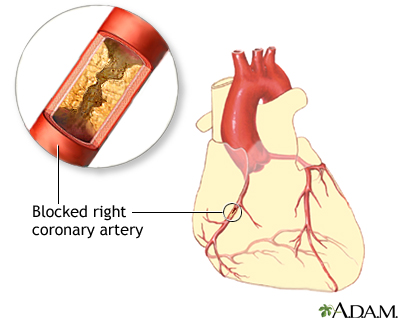
Coronary artery disease due to atherosclerosis is the most common cause of unstable angina. Atherosclerosis is the buildup of fatty material, called plaque, along the walls of the arteries. This causes arteries to become narrowed and less flexible. The narrowing can reduce blood flow to the heart, causing chest pain (angina).
Coronary artery disease
Coronary heart disease is a narrowing of the blood vessels that supply blood and oxygen to the heart. Coronary heart disease (CHD) is also called co...
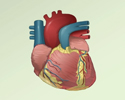
Atherosclerosis
Atherosclerosis, sometimes called "hardening of the arteries," occurs when fat, cholesterol, and other substances build up in the walls of arteries. ...

Angina
Angina is a specific type of pain in the chest caused by inadequate blood flow through the blood vessels (coronary vessels) of the heart muscle (myocardium).
Unstable angina is a special subset of angina and is defined below.
People with unstable angina are at higher risk of having a heart attack.
Less common causes of angina are:
- Abnormal function of tiny branch arteries without narrowing of larger arteries (called microvascular dysfunction or Syndrome X)
- Coronary artery spasm
Coronary artery spasm
The coronary arteries supply blood and oxygen to the heart. Coronary artery spasm is a brief, sudden narrowing of one of these arteries.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Risk factors for coronary artery disease include:
- Diabetes
Diabetes
Diabetes is a long-term (chronic) disease in which the body cannot regulate the amount of sugar in the blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Family history of early coronary heart disease (a close relative such as a sibling or parent had heart disease before age 55 in a man or before age 65 in a woman)
- High blood pressure
High blood pressure
Blood pressure is a measurement of the force exerted against the walls of your arteries as your heart pumps blood to your body. Hypertension is the ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - High LDL cholesterol
- Low HDL cholesterol
- Male sex
- Sedentary lifestyle (not getting enough exercise)
- Obesity
- Older age
- Smoking
Symptoms
Symptoms of angina may include:
- Chest pain that you may also feel in the shoulder, arm, jaw, neck, back, or other area
- Discomfort that feels like tightness, squeezing, crushing, burning, choking, or aching
- Discomfort that occurs at rest and does not easily go away when you take medicine
- Shortness of breath
- Sweating
With stable angina, the chest pain or other symptoms only occur with a certain amount of activity or stress. The pain does not occur more often or get worse over time.
Unstable angina is chest pain that is sudden and often gets worse over a short period of time. You may be developing unstable angina if your chest pain:
- Starts to feel different, is more severe, comes more often, or occurs with less activity or while you are at rest
- Lasts longer than 15 to 20 minutes
- Occurs without cause (for example, while you are asleep or sitting quietly)
- Does not respond well to a medicine called nitroglycerin (especially if this medicine worked to relieve chest pain in the past)
- Occurs with a drop in blood pressure or shortness of breath
Unstable angina is a warning sign that a heart attack may happen soon and needs to be treated right away. Contact your health care provider if you have any type of chest pain.
Exams and Tests
Your provider will do a physical exam and check your blood pressure. Your provider may hear abnormal sounds, such as a heart murmur or irregular heartbeat, when listening to your chest with a stethoscope.
Physical exam
During a physical examination, a health care provider checks your body to determine if you do or do not have a physical problem. A physical examinati...
Blood pressure
Blood pressure is a measurement of the force exerted against the walls of your arteries as your heart pumps blood to your body. Hypertension is the ...

Tests for angina include:
- Blood tests to show if you have heart tissue damage or are at a high risk for heart attack, including high sensitivity cardiac troponins I and T. Testing may also include creatine phosphokinase (CPK), and myoglobin.
Creatine phosphokinase
Creatine phosphokinase (CPK) is an enzyme in the body. It is found mainly in the heart, brain, and skeletal muscle. This article discusses the test...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleMyoglobin
The myoglobin blood test measures the level of the protein myoglobin in the blood. Myoglobin can also be measured with a urine test.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Electrocardiogram (ECG).
Electrocardiogram
An electrocardiogram (ECG) is a test that records the electrical activity of the heart.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Echocardiography.
Echocardiography
An echocardiogram is a test that uses sound waves to create pictures of the heart. The picture and information it produces is more detailed than a s...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Stress tests, such as exercise tolerance test (stress test or treadmill test), nuclear stress test, or stress echocardiogram.
Nuclear stress test
Nuclear stress test is an imaging method that uses radioactive material to show how well blood flows into the heart muscle, both at rest and during a...
 ImageRead Article Now Book Mark Article
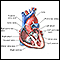
ImageRead Article Now Book Mark ArticleStress echocardiogram
Stress echocardiography is a test that uses ultrasound imaging to show how well your heart muscle is working to pump blood to your body while you exe...
 ImageRead Article Now Book Mark Article
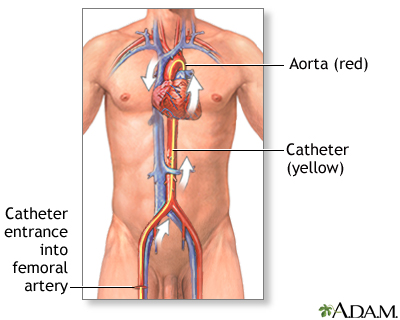
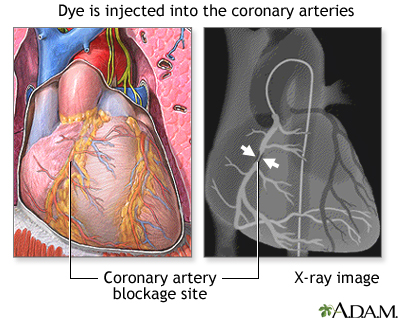
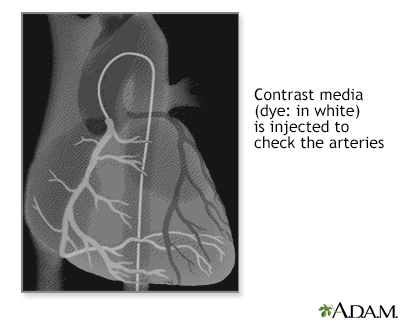
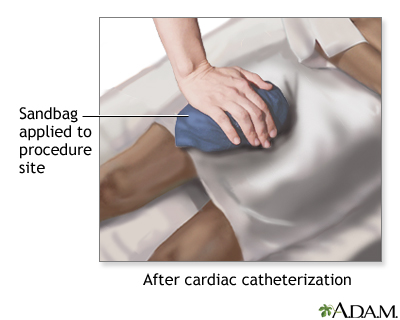
ImageRead Article Now Book Mark Article - Coronary angiography. This test involves taking pictures of the heart arteries using x-rays and dye. It is the most direct test to diagnose heart artery narrowing and find clots.
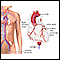
Coronary angiography
Coronary angiography is a procedure that uses a special dye (contrast material) and x-rays to see how blood flows through the arteries in your heart....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Treatment
You may need to check into the hospital to get some rest, have more tests, and prevent complications.
Certain blood thinners (antiplatelet medicines) are used to treat and prevent unstable angina. You will receive these medicines as soon as possible if you can take them safely. Medicines include aspirin and the prescription medicine clopidogrel or something similar (ticagrelor, prasugrel). These medicines may be able to reduce the chance of a heart attack or the severity of a heart attack that occurs.
During an unstable angina event:
- You may get heparin (or another blood thinner) and nitroglycerin (under your tongue or through an IV).
- Other treatments may include medicines to control blood pressure, anxiety, abnormal heart rhythms, and cholesterol (such as a statin medicine).
Abnormal heart rhythms
An arrhythmia is a disorder of the heart rate (pulse) or heart rhythm. The heart can beat too fast (tachycardia), too slow (bradycardia), or irregul...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
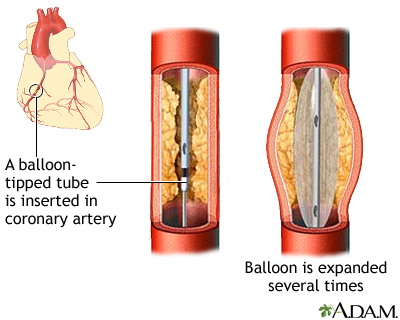
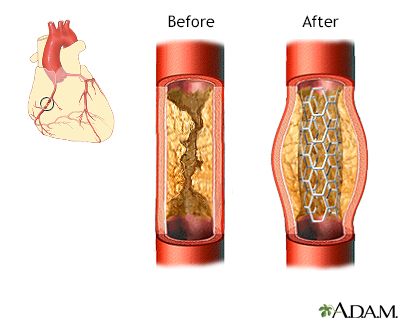
A procedure called angioplasty and stenting can often be done to open a blocked or narrowed artery.
Angioplasty
Angioplasty is a procedure to open narrowed or blocked blood vessels that supply blood to the heart. These blood vessels are called the coronary art...
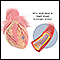
- Angioplasty is a procedure to open narrowed or blocked blood vessels that supply blood to the heart.
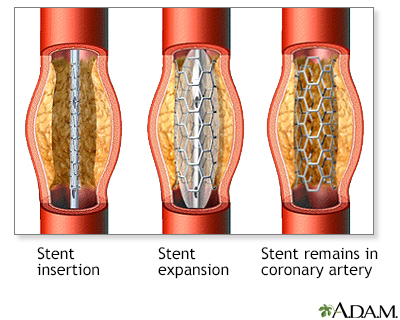
- A coronary artery stent is a small, metal mesh tube that opens up (expands) inside a coronary artery. A stent is often placed after angioplasty. It helps prevent the artery from closing up again. A drug-eluting stent has medicine in it that helps prevent the artery from closing over time.
Stent
A stent is a tiny tube placed into a hollow structure in your body. This structure can be an artery, a vein, or another structure, such as the tube ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Heart bypass surgery may be done for some people. The decision to have this surgery depends on:
Heart bypass surgery
Heart bypass surgery creates a new route, called a bypass, for blood and oxygen to go around a blockage to reach your heart.
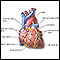
- Which arteries are blocked
- How many arteries are involved
- Which parts of the coronary arteries are narrowed
- How severe the narrowings are
Outlook (Prognosis)
Unstable angina is a sign of more severe heart disease.
How well you do depends on many different things, including:
- How many and which arteries in your heart are blocked, and how severe the blockage is
- If you have ever had a heart attack
- How well your heart muscle is able to pump blood out to your body
Abnormal heart rhythms and heart attacks can cause sudden death.
Possible Complications
Unstable angina may lead to:
- Abnormal heart rhythms (arrhythmias)
- A heart attack
- Heart failure
When to Contact a Medical Professional
Seek medical attention right away if you have new, unexplained chest pain or pressure. If you have had angina before, contact your provider.
Call 911 or the local emergency number if your angina pain:
- Is not better 5 minutes after you take nitroglycerin (your provider may tell you to take 3 total doses)
- Does not go away after 3 doses of nitroglycerin
- Is getting worse
- Returns after the nitroglycerin helped at first
Contact your provider right away if:
- You are having angina symptoms more often
- You are having angina when you are sitting (rest angina)
- You are feeling tired more often
- You are feeling faint or lightheaded, or you pass out
- Your heart is beating very slowly (less than 60 beats a minute) or very fast (more than 120 beats a minute), or it is not steady
- You are having trouble taking your heart medicines
- You have any other unusual symptoms
If you think you are having a heart attack, get medical treatment right away.
Chest pain - Animation
When people have chest pain, they're often concerned they're having a heart attack. I'm Dr. Alan Greene and I'd like to talk to you for a moment about the different kinds of chest pain and when it may be an emergency. It turns out, there are lots of different kinds of chest pain. In fact, almost everything in the chest can hurt in one way or another. Some of the causes are really nothing more than a minor inconvenience. Some of them though are quite serious, even life threatening. You can have chest pain sure from the heart, but also from pneumonia. You can have chest pain from asthma. You can have chest pain from a blood clot in the lungs. It can be from nothing more than a strain of some of the muscles between the ribs, or nerves. You can also have chest pain that comes from acid reflux of from a stomach ulcer, gallstones. Many, many things can cause chest pain. You want to call 911 if you are having sudden, crushing chest pain or if your chest pain radiates into the jaw or the left arm. You want to call 911 if your chest pain also causes shortness of breath, or dizziness, nausea, or vomiting. You want to call 911 if you know you have heart disease and you do occasionally have pain but your pain is getting significantly worse than it is ordinarily. Or comes on with less activity than it does otherwise. But whatever the cause of chest pain, unless you're sure what's causing it, it's worth contacting your physician to find out what may be going on. It's not a symptom to ignore.
Prevention
Some studies have shown that making a few lifestyle changes can prevent blockages from getting worse and may actually improve them. Lifestyle changes can also help prevent some angina attacks. Your provider may tell you to:
- Lose weight if you are overweight
- Stop smoking
- Exercise regularly
- Drink alcohol in moderation only
- Eat a healthy diet that is high in vegetables, fruits, whole grains, fish, and lean meats
Your provider will also recommend that you keep other health conditions such as high blood pressure, diabetes, and high cholesterol levels under control.
If you have one or more risk factors for heart disease, talk to your provider about taking aspirin or other medicines to help prevent a heart attack. Aspirin therapy (75 to 325 mg a day) or medicines such as clopidogrel, ticagrelor or prasugrel may help prevent heart attacks in some people. Aspirin and other blood-thinning therapies are recommended if the benefit is likely to outweigh the risk of side effects.
Reviewed By
Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Bonaca MP, Sabatine MS. Approach to the patient with chest pain. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 35.
Giugliano RP, Braunwald E. Non-ST elevation acute coronary syndromes. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 39.
Gulati M, Levy PD, Mukherjee D, et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Guideline for the evaluation and diagnosis of chest pain: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021;144(22):e368-e454. PMID: 34709879 pubmed.ncbi.nlm.nih.gov/34709879/.
Lange RA, Mukherjee D. Acute coronary syndrome: unstable angina and non-ST elevation myocardial infarction. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 57.
Rao SV, O'Donoghue ML, Ruel M, et al. 2025 ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the management of patients with acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. Published online February 27, 2025. PMID: 40014670 pubmed.ncbi.nlm.nih.gov/40014670/.
Writing Committee Members; Gulati M, Levy PD, Mukherjee D, et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Guideline for the evaluation and diagnosis of chest pain: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2021;78(22):e187-e285. PMID: 34756653 pubmed.ncbi.nlm.nih.gov/34756653/.



 All rights reserved.
All rights reserved.