Peripheral artery disease of the legs - self-care
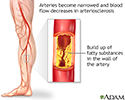
Peripheral vascular disease - self-care; Intermittent claudication - self-carePeripheral artery disease (PAD) is a narrowing of the blood vessels that bring blood to the legs and feet. It can occur when cholesterol and other fatty material (atherosclerotic plaque) build-up on the walls of your arteries.
Atherosclerotic plaque
Atherosclerosis, sometimes called "hardening of the arteries," occurs when fat, cholesterol, and other substances build up in the walls of arteries. ...
PAD is mostly seen in people above 65 years of age. Diabetes, smoking, and high blood pressure increase the risk for PAD.
Diabetes
Diabetes is a long-term (chronic) disease in which the body cannot regulate the amount of sugar in the blood.
High blood pressure
Blood pressure is a measurement of the force exerted against the walls of your arteries as your heart pumps blood to your body. Hypertension is the ...

The symptoms of PAD include cramps in the legs mostly during physical activities (intermittent claudication). In severe cases, there may also be pain when the leg is at rest.
Managing the risk factors can reduce the risk of further cardiovascular damage. Treatment mainly includes medicines and rehabilitation. In severe cases, surgery or other procedures may also be done.
Walking Improves Blood Flow
A regular walking program will improve blood flow as new, small blood vessels form. The walking program is mainly as follows:
- Warm up by walking at a pace that does not cause your normal leg symptoms.
- Then walk to the point of mild-to-moderate pain or discomfort.
- Rest until the pain goes away, then try walking again.
Your goal over time is to be able to walk 30 to 60 minutes. Always talk with your health care provider before you start an exercise program. Contact your provider right away if you have any of these symptoms during or after exercise:
-
Chest pain
Chest pain
Chest pain is discomfort or pain that you feel anywhere along the front of your body between your neck and upper abdomen.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Breathing problems
-
Dizziness
Dizziness
Dizziness is a term that is often used to describe 2 different symptoms: lightheadedness and vertigo. Lightheadedness is a feeling that you might fai...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
An uneven heart rate
An uneven heart rate
An arrhythmia is a disorder of the heart rate (pulse) or heart rhythm. The heart can beat too fast (tachycardia), too slow (bradycardia), or irregul...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Make simple changes to add walking to your day.
Make simple changes to add walking to y...
Physical activity -- which includes an active lifestyle and routine exercise -- plus eating well, is the best way to stay healthy.

- At work, try taking the stairs instead of the elevator, take a 5-minute walk break every hour, or add a 10- to 20-minute walk during lunch.
- Try parking at the far end of the parking lot, or even down the street. Even better, try walking to the store.
- If you ride the bus, get off the bus 1 or more stops before your normal stop and walk the rest of the way.
- Aim for a total of 30 minutes of walking, 5 times per week.
Lifestyle Changes
Stop smoking. Smoking narrows your arteries and increases the risk for atherosclerotic plaque or blood clots forming. Other things you can do to stay as healthy as possible are to:
- Make sure your blood pressure is well-controlled.
- Reduce your weight, if you are overweight.
- Eat a low-cholesterol and low-fat diet.
- Test your blood sugar if you have diabetes, and keep it under control.
Take Care of Your Feet
Check your feet every day. Inspect the tops, sides, soles, heels, and between your toes. If you have vision problems, ask someone to check your feet for you. Use a moisturizer to keep your skin healthier. Look for:
- Dry or cracked skin
- Blisters or sores
- Bruises or cuts
- Redness, warmth, or tenderness
- Firm or hard spots
Contact your provider right away about any foot problems. Do not try to treat them yourself first.
What Else?
If you are taking medicines for high blood pressure, high cholesterol, or diabetes, take them as prescribed. If you are not taking medicine for high cholesterol, ask your provider about it as it may still help you even if your cholesterol is not high.
Your provider may prescribe the following medicines to control your peripheral artery disease:
- Aspirin, clopidogrel (Plavix), or other medicines which keep your blood from forming clots
- Cilostazol, a medicine that widens (dilates) the blood vessels and also thins the blood
Do not stop taking these medicines without first talking with your provider.
When to Call the Doctor
Contact your provider if you have:
- A leg or foot that is cool to the touch, pale, blue, or numb
- Chest pain or shortness of breath when you have leg pain
- Leg pain that does not go away, even when you are not walking or moving (called rest pain)
- Legs that are red, hot, or swollen
- New sores on your legs or feet
- Signs of infection (fever, sweats, red and painful skin, general ill feeling)
- Sores that do not heal
References
Bonaca MP, Creager MA. Peripheral artery diseases. In: Libby P, Bonow RO, Mann DL, Tomaselli GF, Bhatt DL, Solomon SD, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 12th ed. Philadelphia, PA: Elsevier; 2022:chap 43.
Michael W. Peripheral artery disease. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier 2024:152-155.
Henkin S, Creager MA. Peripheral artery disease. In: Hoffman R, Benz EJ, Silberstein LE, et al, eds. Hematology: Basic Principles and Practice. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 146.
Simons JP, Schanzer A. Lower extremity arterial disease: decision making and medical management. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 108.
-
Walking for health - illustration
Exercise, including walking at least 30 minutes a day, decreases the risk of heart attacks, stroke, hypertension, some cancers, osteoporosis, depression and obesity.
Walking for health
illustration
-
Arteriosclerosis of the extremities - illustration
Arteriosclerosis of the extremities is a disease of the peripheral blood vessels that is characterized by narrowing and hardening of the arteries that supply the legs and feet. The narrowing of the arteries causes a decrease in blood flow. Symptoms include leg pain, numbness, cold legs or feet and muscle pain in the thighs, calves or feet.
Arteriosclerosis of the extremities
illustration
-
Walking for health - illustration
Exercise, including walking at least 30 minutes a day, decreases the risk of heart attacks, stroke, hypertension, some cancers, osteoporosis, depression and obesity.
Walking for health
illustration
-
Arteriosclerosis of the extremities - illustration
Arteriosclerosis of the extremities is a disease of the peripheral blood vessels that is characterized by narrowing and hardening of the arteries that supply the legs and feet. The narrowing of the arteries causes a decrease in blood flow. Symptoms include leg pain, numbness, cold legs or feet and muscle pain in the thighs, calves or feet.
Arteriosclerosis of the extremities
illustration
-
Stroke - InDepth
(In-Depth)
-
Diabetes - type 2 - InDepth
(In-Depth)
-
Diabetes - type 1 - InDepth
(In-Depth)
-
Smoking - InDepth
(In-Depth)
-
Erectile dysfunction - InDepth
(In-Depth)
-
Headaches - cluster - InDepth
(In-Depth)
Review Date: 10/11/2024
Reviewed By: Frank D. Brodkey, MD, FCCM, Associate Professor, Section of Pulmonary and Critical Care Medicine, University of Wisconsin School of Medicine and Public Health, Madison, WI. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.