Shoulder separation - aftercare
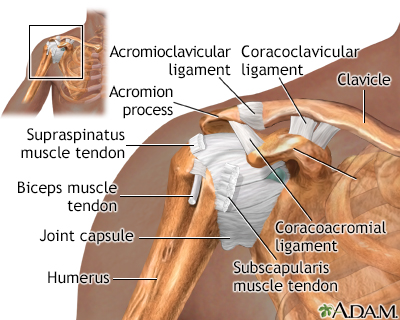
Separated shoulder - aftercare; Acromioclavicular joint separation - aftercare; A/C separation - aftercareShoulder separation is not an injury to the main shoulder joint itself. It is an injury to the top of the shoulder where the collarbone (clavicle) meets the top of the shoulder blade (acromion of the scapula).
It is not the same as a shoulder dislocation. A dislocated shoulder occurs when the arm bone comes out of the main shoulder joint.
About Your Injury
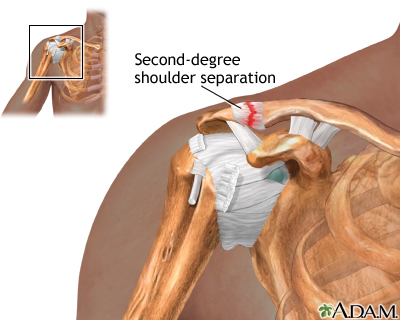
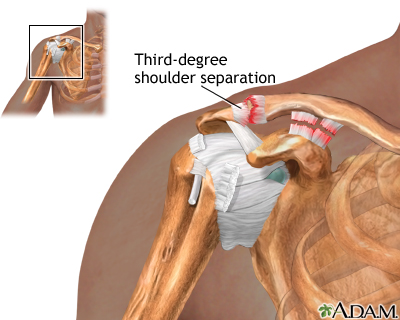
Most shoulder separation injuries are caused by falling onto the shoulder. This results in a tear in the tissue that connects the collarbone and top of the shoulder blade. These tears can also be caused by car accidents and sports injuries.
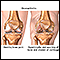
This injury can make the shoulder look abnormal due to the end of a bone sticking up or the shoulder hanging lower than normal.
Pain is usually at the very top of the shoulder.
Your health care provider may have you hold onto a weight while examining you to see if your collarbone sticks out. Your provider may also perform a cross-body adduction test, also called a scarf test, where they passively bring your arm across your body to test for a shoulder separation. An x-ray or ultrasound of your shoulder may help diagnose a shoulder separation.
Ultrasound
Ultrasound uses high-frequency sound waves to make images of organs and structures inside the body.
What to Expect
Most people recover from a shoulder separation without surgery, within 2 to 12 weeks. You will be treated with ice, pain medicines, a sling, and then exercises as you continue to heal.
Your recovery may be slower if you have:
-
Arthritis in your shoulder joint
Arthritis
Arthritis is inflammation or degeneration of one or more joints. A joint is the area where 2 bones meet. There are more than 100 different types of...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Damaged cartilage (cushioning tissue) between your collarbone and top of your shoulder blade
- A severe shoulder separation
You may need surgery right away if you have:
- Numbness in your fingers
- Cold fingers
- Muscle weakness in your arm
- Severe deformity of the joint
Self-care at Home
Make an ice pack by putting ice in a sealable plastic bag and wrapping a cloth around it. Do not put the bag of ice directly on the area, as the ice could damage your skin.
On the first day of your injury, apply the ice for 20 minutes every hour while awake. After the first day, ice the area every 3 to 4 hours for 20 minutes each time. Do this for 2 days or longer, or as instructed by your provider.
For pain, you can take ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), aspirin, or acetaminophen (Tylenol). You can buy these pain medicines without a prescription.
- Talk with your provider before using these medicines if you have heart disease, high blood pressure, kidney disease, liver disease, or have had stomach ulcers or bleeding.
- Do not take more than the amount recommended on the bottle.
- Do not give aspirin to children.
Tell your provider about any other medicines you are taking as medicine interactions may occur.
You may be given a shoulder sling to use for a few weeks.
- Once you have less pain, begin range of motion exercises so that your shoulder does not get stuck in place. This is called contracture or frozen shoulder. Check with your provider before doing any of these motions.
- After your injury has healed, do not lift heavy objects for 8 to 12 weeks or as instructed by your provider.
Follow-up
If you continue to have pain, your provider will probably ask you to come back in 1 week to decide if you need to:
- See an orthopedist (bone and joint doctor)
- Begin physical therapy or range of motion exercises
Outlook (Prognosis)
Most shoulder separations heal without serious consequences. In a severe injury, there may be long-term difficulties lifting heavy objects with the injured side.
When to Call the Doctor
Contact your provider or go to the emergency room right away if you have:
- Severe pain
- Weakness in your arm or fingers
- Numb or cold fingers
- A sharp decrease in how well you can move your arm
- A lump on top of your shoulder that makes your shoulder look abnormal
References
Andermahr J, Ring D, Jupiter JB. Fractures and dislocations of the clavicle. In: Browner BD, Jupiter JB, Krettek C, Anderson PA, eds. Skeletal Trauma: Basic Science, Management, and Reconstruction. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 48.
Rizzo TD. Acromioclavicular injuries. In: Frontera WR, Silver JK, Rizzo TD, eds. Essentials of Physical Medicine and Rehabilitation. 4th ed. Philadelphia, PA: Elsevier; 2019:chap 10.
Rudy CC, Daya MR. Shoulder injuries. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 45.
Scholten P, Stanos SP, Rivers WE, Prather H, Press J. Physical medicine and rehabilitation approaches to pain management. In: Benzon HT, Raja SN, Liu SS, Fishman SM, Cohen SP, eds. Essentials of Pain Medicine. 4th ed. Philadelphia, PA: Elsevier; 2018:chap 58.
Review Date: 4/3/2024
Reviewed By: Jesse Borke, MD, CPE, FAAEM, FACEP, Attending Physician at Kaiser Permanente, Orange County, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.