ESR
Erythrocyte sedimentation rate; Sed rate; Sedimentation rateESR stands for erythrocyte sedimentation rate. It is commonly called a "sed rate."
It is a test that indirectly measures the level of certain proteins in the blood. This measurement correlates with the amount of inflammation in the body.
How the Test is Performed
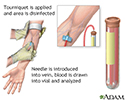
A blood sample is needed. Most of the time, blood is drawn from a vein located on the inside of the elbow or the back of the hand. The blood sample is sent to a lab.
Drawn from a vein
Venipuncture is the collection of blood from a vein. It is most often done for laboratory testing.
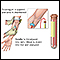
The test measures how fast red blood cells (called erythrocytes) fall to the bottom of a tall, thin tube.
How to Prepare for the Test
There are no special steps needed to prepare for this test.
How the Test will Feel
You may feel slight pain or a sting when the needle is inserted. You may also feel some throbbing at the site after the blood is drawn.
Why the Test is Performed
Reasons why a "sed rate" may be done include:
- Unexplained fevers
- Certain types of joint pain or arthritis
- Muscle symptoms
- Headache
- Other vague symptoms that cannot be explained
This test may also be used to monitor whether an illness is responding to treatment.
This test can be used to monitor inflammatory diseases or cancer. It is not used to diagnose a specific disorder.
However, the test is useful for detecting and monitoring:
- Autoimmune disorders
- Bone infections
- Certain forms of arthritis
- Inflammatory diseases
Normal Results
For adults (Westergren method):
- Men under 50 years old: less than 15 mm/hr
- Men over 50 years old: less than 20 mm/hr
- Women under 50 years old: less than 20 mm/hr
- Women over 50 years old: less than 30 mm/hr
For children (Westergren method):
- Newborn: 0 to 2 mm/hr
- Newborn to puberty: 3 to 13 mm/hr
Note: mm/hr = millimeters per hour
Normal value ranges may vary slightly among different laboratories. Talk to your health care provider about the meaning of your specific test results.
What Abnormal Results Mean
An abnormal ESR may help with a diagnosis, but it does not prove that you have a certain condition. Other tests are almost always needed.
An increased ESR rate may occur in people with:
-
Anemia
Anemia
Anemia is a condition in which the body does not have enough healthy red blood cells. Red blood cells provide oxygen to body tissues. Different type...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Cancers such as lymphoma or multiple myeloma
Multiple myeloma
Multiple myeloma is a blood cancer that starts from a type of white blood cell in the bone marrow called plasma cells. Bone marrow is the soft, spon...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Kidney disease
- Pregnancy
- Thyroid disease
The immune system helps protect the body against harmful substances. An autoimmune disorder is when the immune system mistakenly attacks and destroys healthy body tissue. ESR is often higher than normal in people with an autoimmune disorder.
Autoimmune disorder
An autoimmune disorder occurs when the body's immune system attacks and destroys healthy body tissue by mistake. There are more than 80 autoimmune d...
Common autoimmune disorders include:
-
Lupus
Lupus
Systemic lupus erythematosus (SLE) is an autoimmune disease. In this disease, the immune system of the body mistakenly attacks healthy tissue. It c...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Polymyalgia rheumatica
Polymyalgia rheumatica
Polymyalgia rheumatica (PMR) is an inflammatory disorder. It involves pain and stiffness in the shoulders and often the hips.
Read Article Now Book Mark Article -
Rheumatoid arthritis in adults or children
Rheumatoid arthritis in adults
Rheumatoid arthritis (RA) is a disease that leads to inflammation of the joints and surrounding tissues. It is a long-term disease. It can also aff...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleChildren
Juvenile idiopathic arthritis (JIA) is a term used to describe a group of disorders in children that includes arthritis. They are long-term (chronic...
Read Article Now Book Mark Article
Very high ESR levels occur with less common autoimmune or other disorders, including:
- Allergic vasculitis
-
Giant cell arteritis
Giant cell arteritis
Giant cell arteritis (GCA) is inflammation and damage to the blood vessels that supply blood to the head, neck, upper body and arms. It is also call...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Hyperfibrinogenemia (increased fibrinogen levels in the blood)
Fibrinogen
Fibrinogen is a protein produced by the liver. This protein helps stop bleeding by helping blood clots to form. A blood test can be done to tell ho...
Read Article Now Book Mark Article -
Macroglobulinemia - primary
Macroglobulinemia - primary
Waldenström macroglobulinemia (WM) is a cancer of the B lymphocytes (a type of white blood cell). WM is associated with the overproduction of protei...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Necrotizing vasculitis
Necrotizing vasculitis
Necrotizing vasculitis is a group of disorders that involve inflammation of the blood vessel walls. The size of the affected blood vessels helps to ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
An increased ESR rate may be due to some infections, including:
- Bodywide (systemic) infection
-
Bone infections
Bone infections
Osteomyelitis is a bone infection. It is caused by bacteria or other germs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Infection of the heart or heart valves
Infection of the heart or heart valves
Endocarditis is inflammation of the inside lining of the heart chambers and heart valves (endocardium). It is most often caused by a bacterial or, r...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Rheumatic fever
Rheumatic fever
Rheumatic fever is a disease that may develop after an infection with group A streptococcus bacteria (such as strep throat or scarlet fever). It can...
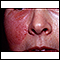
Read Article Now Book Mark Article - Severe skin infections, such as erysipelas
Erysipelas
Erysipelas is a type of skin infection. It affects the outermost layer of the skin and the local lymph nodes.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Tuberculosis
Lower-than-normal levels occur with:
-
Congestive heart failure
Congestive heart failure
Heart failure is a condition in which the heart is no longer able to pump oxygen-rich blood to the rest of the body efficiently. This causes symptom...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Hyperviscosity
Hyperviscosity
Polycythemia can occur when there are too many red blood cells (RBCs) in an infant's blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Hypofibrinogenemia (decreased fibrinogen levels)
Hypofibrinogenemia
Congenital fibrinogen deficiency is a very rare, inherited blood disorder in which the blood does not clot normally. It affects a protein called fib...
Read Article Now Book Mark Article - Leukemia
- Low plasma protein (due to liver or kidney disease)
-
Polycythemia
Polycythemia
Polycythemia vera (PV) is a bone marrow disease that leads to an abnormal increase in the number of blood cells. The red blood cells are the most af...
Read Article Now Book Mark Article -
Sickle cell anemia
Sickle cell anemia
Sickle cell disease is a disorder passed down through families. The red blood cells that are normally shaped like a disk take on a sickle or crescen...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
References
Deane KD, Pisetsky DS. Laboratory testing in the rheumatic diseases. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 237.
Vajpayee N, Graham SS, Bem S. Basic examination of blood and bone marrow. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA: Elsevier; 2022:chap 31.
-
Blood test - illustration
Blood is drawn from a vein (venipuncture), usually from the inside of the elbow or the back of the hand. A needle is inserted into the vein, and the blood is collected in an air-tight vial or a syringe. Preparation may vary depending on the specific test.
Blood test
illustration
-
Blood test - illustration
Blood is drawn from a vein (venipuncture), usually from the inside of the elbow or the back of the hand. A needle is inserted into the vein, and the blood is collected in an air-tight vial or a syringe. Preparation may vary depending on the specific test.
Blood test
illustration
Review Date: 8/20/2023
Reviewed By: Jacob Berman, MD, MPH, Clinical Assistant Professor of Medicine, Division of General Internal Medicine, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.