Spinal cord abscess
Abscess - spinal cordSpinal cord abscess is the swelling and irritation (inflammation) and the collection of infected material (pus) and germs in or around the spinal cord.
Causes
A spinal cord abscess is caused by an infection inside the spine. An abscess of the spinal cord itself is very rare. A spinal abscess usually occurs as a complication of an epidural abscess.
Epidural abscess
An epidural abscess is a collection of pus (infected material) and germs between the outer covering of the brain and spinal cord and the bones of the...
Pus forms as a collection of:
- White blood cells
- Fluid
- Live and dead bacteria or other microorganisms
- Destroyed tissue cells
The pus is commonly covered by a lining or membrane that forms around the edges. The pus collection causes pressure on the spinal cord.
The infection is usually due to bacteria. Often it is caused by a staphylococcus infection that spreads through the spine. It may be caused by tuberculosis in some areas of the world, but this is not as common today as it was in the past. In rare cases, the infection may be due to a fungus.
Tuberculosis
Pulmonary tuberculosis (TB) is a contagious bacterial infection that involves the lungs. It may spread to other organs.
The following increase your risk for a spinal cord abscess:
- Back injuries or trauma, including minor ones
- Boils on the skin, especially on the back or scalp (rare)
Boils
A boil is an infection that affects groups of hair follicles and nearby skin tissue. Related conditions include folliculitis, an inflammation of one ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Complication of lumbar puncture or back surgery
Lumbar puncture
Cerebrospinal fluid (CSF) collection is a test to look at the fluid that surrounds the brain and spinal cord. CSF acts as a cushion, protecting the b...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Spread of any infection through the bloodstream from another part of the body (bacteremia)
Bacteremia
Sepsis is an illness in which the body has a severe, inflammatory response to bacteria or other germs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Injecting drugs
The infection often begins in the bone (osteomyelitis). The bone infection may cause an epidural abscess to form. This abscess gets larger and presses on the spinal cord. The infection can spread to the cord itself.
Osteomyelitis
Osteomyelitis is a bone infection. It is mainly caused by bacteria or other germs.

A spinal cord abscess is rare. When it does occur, it can be life threatening.
Symptoms
Symptoms may include any of the following:
- Fever and chills.
- Loss of bladder or bowel control.
- Loss of movement of an area of the body below the abscess.
Loss of movement
Muscle function loss is when a muscle does not work or move normally. The medical term for complete loss of muscle function is paralysis.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Loss of sensation of an area of the body below the abscess.
Loss of sensation
Numbness and tingling are abnormal sensations that can occur anywhere in your body, but they are often felt in your fingers, hands, feet, arms, or le...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Low backache, often mild, but slowly gets worse, with pain moving to the hip, leg, or feet. Or, pain may spread to the shoulder, arm, or hand.
Exams and Tests
The health care provider will perform a physical exam and may find the following:
- Tenderness over the spine
- Spinal cord compression
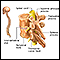
Spinal cord compression
Spinal cord trauma is damage to the spinal cord. It may result from direct injury to the cord itself or indirectly from disease of the nearby bones,...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Paralysis of the lower body (paraplegia) or of the entire trunk, arms, and legs (quadriplegia)
- Changes in sensation below the area where the spine is affected
The amount of nerve loss depends on where the abscess is located on the spine and how much it is compressing the spinal cord.
Tests that may be done include:
- Complete blood count (CBC)
Complete blood count (CBC)
A complete blood count (CBC) test measures the following:The number of white blood cells (WBC count)The number of red blood cells (RBC count)The numb...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - CT scan of the spine
CT scan
A computed tomography (CT) scan is an imaging method that uses x-rays to create pictures of cross-sections of the body. Related tests include:Abdomin...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Draining of abscess (may require surgery)
- Gram stain and culture of abscess material
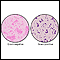
Gram stain
A Gram stain is a test used to identify bacteria. It is one of the most common ways to quickly diagnose bacterial infection in the body.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - MRI of the spine
MRI
A magnetic resonance imaging (MRI) scan is an imaging test that uses powerful magnets and radio waves to create pictures of the body. It does not us...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Treatment
The goals of treatment are to relieve pressure on the spinal cord and cure the infection.
Surgery may be done right away to relieve the pressure. It involves removing part of the spine bone and draining the abscess. Sometimes it is not possible to drain the abscess completely.
Antibiotics are used to treat the infection. They are usually given through a vein (IV).
Outlook (Prognosis)
How well a person does after treatment varies. Some people recover completely.
An untreated spinal cord abscess can lead to spinal cord compression. It can cause permanent, severe paralysis and nerve loss. It may be life threatening.
If the abscess is not drained completely, it may return or cause scarring in the spinal cord.
Possible Complications
The abscess can injure the spinal cord from direct pressure. Or, it can cut off the blood supply to the spinal cord.
Complications may include:
- Long-term (chronic) back pain
- Loss of bladder/bowel control
- Loss of sensation
- Male impotence
- Return of infection
- Weakness, paralysis
When to Contact a Medical Professional
Go to the emergency room or call 911 or the local emergency number, if you have symptoms of spinal cord abscess.
Prevention
Thorough treatment of boils, tuberculosis, and other infections decreases the risk. Early diagnosis and treatment are important to prevent complications.
References
Rajasekaran S, Viswanathan VK, Shetty AP. Primary infections of the spine. In: Steinmetz MP, Berven SH, Benzel EC, eds. Benzel's Spine Surgery. 5th ed. Philadelphia, PA: Elsevier; 2022:chap 44.
Williams KD. Infections and tumors of the spine. In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 42.
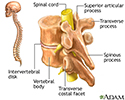
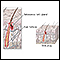
Vertebrae - illustration
The vertebral column is made up of 26 bones that provide axial support to the trunk. The vertebral column provides protection to the spinal cord, which runs through its central cavity. Between each vertebra is an intervertebral disk, which acts as a shock absorber.
Vertebrae
illustration
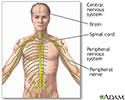
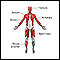
Central nervous system and peripheral nervous system - illustration
The central nervous system comprises the brain and spinal cord. The peripheral nervous system includes nerves outside the brain and spinal cord.
Central nervous system and peripheral nervous system
illustration
Vertebrae - illustration
The vertebral column is made up of 26 bones that provide axial support to the trunk. The vertebral column provides protection to the spinal cord, which runs through its central cavity. Between each vertebra is an intervertebral disk, which acts as a shock absorber.
Vertebrae
illustration
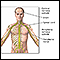
Central nervous system and peripheral nervous system - illustration
The central nervous system comprises the brain and spinal cord. The peripheral nervous system includes nerves outside the brain and spinal cord.
Central nervous system and peripheral nervous system
illustration
Review Date: 12/4/2022
Reviewed By: Jatin M. Vyas, MD, PhD, Associate Professor in Medicine, Harvard Medical School; Associate in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.