Biliary atresia
Jaundice newborns - biliary atresia; Newborn jaundice - biliary atresia; Extrahepatic ductopenia; Progressive obliterative cholangiopathyBiliary atresia is a blockage in the tubes (ducts) that carry a liquid called bile from the liver to the gallbladder.
Causes
Biliary atresia occurs when the bile ducts inside or outside the liver are abnormally narrow, blocked, or absent. The bile ducts carry a digestive fluid from liver to small bowel to break down fats and filter out waste from the body.
The cause of the disease is not clear. It may be due to:
- Viral infection after birth
- Exposure to toxic substances
- Multiple genetic factors
- Perinatal injury
- Some medicines such as carbamazepine
It more commonly affects people of East Asian and African-American descent.
The bile ducts help remove waste from the liver and carry salts that help the small intestine break down (digest) fat.
In babies with biliary atresia, bile flow from the liver to the gallbladder is blocked. This can lead to liver damage and cirrhosis of the liver, which can be deadly.
Symptoms
Symptoms usually start to occur between 2 to 8 weeks. Jaundice (a yellow color to the skin and mucus membranes) develops slowly 2 to 3 weeks after birth. The infant may gain weight normally for the first month. After that point, the baby will lose weight and become irritable, and will have worsening jaundice.
Other symptoms may include:
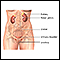
- Dark urine
Dark urine
The usual color of urine is straw-yellow. Abnormally-colored urine may be cloudy, dark, or blood-colored.
 ImageRead Article Now Book Mark Article
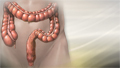
ImageRead Article Now Book Mark Article - Swollen belly
Swollen belly
Abdominal bloating is a condition in which the belly (abdomen) feels full and tight. Your belly may look swollen (distended).
 ImageRead Article Now Book Mark Article
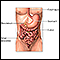
ImageRead Article Now Book Mark Article - Foul-smelling and floating stools
Foul-smelling
Foul-smelling stools are stools with a very bad odor. They very often have to do with what you eat, but may be a sign of a medical condition....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleFloating stools
Stools that float are most often due to poor absorption of nutrients (malabsorption) or too much gas (flatulence).
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Pale or clay-colored stools
Pale or clay-colored stools
Stools that are pale, clay, or putty-colored may be due to problems in the biliary system. The biliary system is the drainage system of the gallblad...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Slow growth
Slow growth
Delayed growth is poor or abnormally slow height or weight gains in a child younger than age 5. This may just be normal, and the child may outgrow i...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Exams and Tests
Your health care provider will take medical history of your child and do a physical exam to check for enlarged liver.
Tests to diagnose biliary atresia include:
- Abdominal x-ray to check for enlarged liver and spleen
Abdominal x-ray
An abdominal x-ray is an imaging test to look at organs and structures in the abdomen. Organs include the liver, spleen, stomach, and intestines. T...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Abdominal ultrasound to check internal organs
Abdominal ultrasound
Abdominal ultrasound is a type of imaging test. It is used to look at organs in the abdomen, including the liver, gallbladder, pancreas, and kidneys...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Blood tests to check total and direct bilirubin levels
- Hepatobiliary scintigraphy or HIDA scan to check whether the bile ducts and gallbladder are working properly
- Liver biopsy to check the severity of cirrhosis or to rule out other causes of jaundice
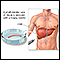
Liver biopsy
A liver biopsy is a test that takes a sample of tissue from the liver for examination.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - X-ray of the bile ducts (cholangiogram) to check if the bile ducts are opened or closed
Treatment
An operation called the Kasai procedure is done to connect the liver to the small intestine. The abnormal ducts are bypassed. The surgery is more successful if done before the baby is 8 weeks old.
Liver transplant may still be needed before 20 years of age in most of the cases.
Outlook (Prognosis)
Early surgery will improve the survival of more than one third of babies with this condition. The long-term benefit of a liver transplant is not yet known, but it is expected to improve survival.
Possible Complications
Complications may include:
- Infection
- Irreversible cirrhosis
- Liver failure
- Surgical complications, including failure of the Kasai procedure
When to Contact a Medical Professional
Contact your provider if your child appears jaundiced, or if other symptoms of biliary atresia develop.
References
Berlin SC. Diagnostic imaging of the neonate. In: Martin RJ, Fanaroff AA, Walsh MC, eds. Fanaroff and Martin's Neonatal-Perinatal Medicine. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 38.
Cazares J, Ure B, Yamataka A. Biliary atresia. In: Holcomb GW, Murphy JP, St. Peter SD, eds. Holcomb and Ashcraft's Pediatric Surgery. 7th ed. Philadelphia, PA: Elsevier; 2020:chap 43.
Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC. Cholestasis. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 383.
O'Hara SM. The pediatric liver and spleen. In: Rumack CM, Levine D, eds. Diagnostic Ultrasound. 6th ed. Philadelphia, PA: Elsevier; 2024:chap 52.
The biliary organs and duct system that creates, transports, stores, and releases bile into the duodenum for digestion includes the liver, gallbladder, and bile ducts (named the cystic, hepatic, common, and pancreatic duct).
Bile produced in the liver
illustration
Review Date: 2/17/2024
Reviewed By: Charles I. Schwartz, MD, FAAP, Clinical Assistant Professor of Pediatrics, Perelman School of Medicine at the University of Pennsylvania, General Pediatrician at PennCare for Kids, Phoenixville, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.


