Gastroesophageal reflux disease
Gastroesophageal reflux disease (GERD) is a condition in which the stomach contents leak backward from the stomach into the esophagus (food pipe). Food travels from your mouth to the stomach through your esophagus. GERD can irritate the food pipe and cause heartburn and other symptoms.
Gastroesophageal reflux disease - Animation
Do you feel a burning in your chest not long after you eat or lie down? If so, you may have Gastroesophageal reflux disease, or GERD. When we swallow food, it travels down our esophagus into the stomach, where it's greeted by a rush of Hydrochloric acid in the stomach to begin digestion. This acid is so powerful, it could eat the paint right off your car! Fortunately, there's a band of muscle between the stomach and the esophagus - called the Lower Esophageal Sphincter or L-E-S, that clamps down to prevent the stomach contents from moving or refluxing upward and burning the lining of the esophagus. If that band of muscle does not adequately clamp down, this backwash causes the irritation and burning that's known as heartburn or GERD. Maintaining good tight L-E-S muscle tone is the key to preventing this condition. Causes of GERD include being overweight, smoking, and drinking too much alcohol. Certain foods, like chocolate and peppermint and if you're a woman, pregnancy can bring on GERD. To determine if you have GERD, your doctor may request an upper endoscopy exam to look into your esophagus and stomach to diagnose reflux. Other tests can measure the acid and amount of pressure in your esophagus, or if you have blood in your stool. If you do have GERD, lifestyle changes can help. First, avoid foods that cause problems for you and avoid eating large meals. If you're a little on the heavy side, try to lose some weight. Since most GERD symptoms are experienced lying down in bed, let gravity help. Elevating the head of your bed 4 to 6 inches using blocks of wood may help. If symptoms continue, see your doctor or a Gastroenterologist for evaluation and an upper endoscopy exam. Your doctor may suggest you take over-the-counter antacids or may prescribe stronger medications. Call your doctor if you are bleeding, feel like you are choking, have trouble-swallowing, or experience sudden weight loss. The good news is most people who have GERD do not need surgery. For the worst cases, surgeons may perform a laparoscopic procedure to tighten a weak L-E-S muscle. If you have occasional heartburn, antacid tablets can be used as needed. However! If you're having heartburn more than 3 to 4 times a week, see your doctor & take the prescribed medication to prevent this condition.
Causes
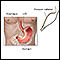
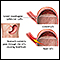
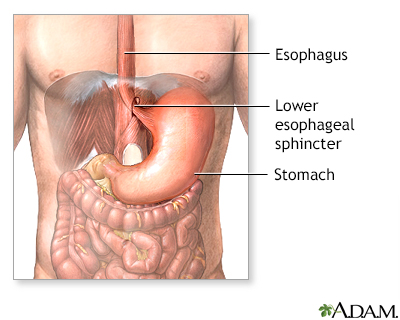
When you eat, food passes from the throat to the stomach through the esophagus. A ring of muscle fibers in the lower esophagus prevents swallowed food from moving back up. These muscle fibers are called the lower esophageal sphincter (LES).
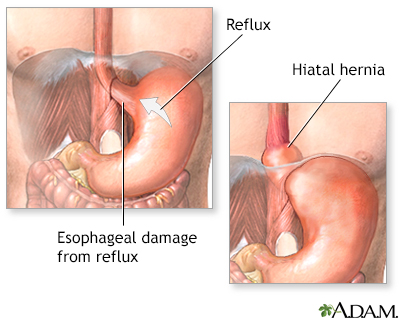
When this ring of muscle does not close all the way, stomach contents can leak back into the esophagus. This is called reflux or gastroesophageal reflux. Reflux may cause symptoms. Harsh stomach acids can also damage the lining of the esophagus.

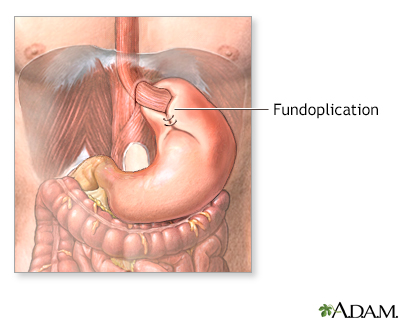
Gastroesophageal reflux disease
A band of muscle fibers, the lower esophageal sphincter, closes off the esophagus from the stomach. If the sphincter does not close properly, food and liquid can move backward into the esophagus and cause heartburn and other symptoms known as gastroesophageal disease (GERD). To alleviate symptoms dietary changes and medications are prescribed. For a patient who has persistent symptoms despite medical treatment, an anti-reflux operation may be an option.
The risk factors for reflux include:
- Use of alcohol (possibly)
- Hiatal hernia (a condition in which part of the stomach moves above the diaphragm, which is the muscle that separates the chest and abdominal cavities)
Hiatal hernia
Hiatal hernia is a condition in which part of the stomach extends through an opening of the diaphragm into the chest. The diaphragm is the sheet of ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Obesity
Obesity
Obesity means weighing more than what is healthy for a given height. Obesity is a serious, chronic disease. It can lead to other health problems, i...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Pregnancy
Pregnancy
Growing a baby is hard work. Your body will go through a lot of changes as your baby grows and your hormones change. Along with the aches and pains...
Read Article Now Book Mark Article - Scleroderma
Scleroderma
Scleroderma is a disease that involves the buildup of fibrous tissue in the skin and elsewhere in the body. It also damages the cells that line the ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Smoking or tobacco use
- Lying down within 3 hours after eating
Heartburn and gastroesophageal reflux can be caused by or made worse by pregnancy. Symptoms can also be caused by certain medicines, such as:
- Anticholinergics (for example, sea sickness medicine)
- Beta-blockers for high blood pressure or heart disease
- Bronchodilators for asthma or other lung diseases
Asthma
Asthma is a chronic disease that causes the airways of the lungs to swell and narrow. It leads to breathing difficulty such as wheezing, shortness o...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Calcium channel blockers for high blood pressure
High blood pressure
Blood pressure is a measurement of the force exerted against the walls of your arteries as your heart pumps blood to your body. Hypertension is the ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Dopamine-active medicines for Parkinson disease
Parkinson disease
Parkinson disease results from certain brain cells dying. These cells help control movement and coordination. The disease leads to shaking (tremors...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Progestin for abnormal menstrual bleeding or birth control
- Sedatives for insomnia or anxiety
- Theophylline (for asthma or other lung diseases)
- Tricyclic antidepressants
Talk to your health care provider if you think one of your medicines may be causing heartburn. Never change or stop taking a medicine without first talking to your provider.
Heartburn - Animation
Eating spicy foods, such as pizza, may cause a person to feel heartburn. Although the name may imply the heart, heartburn has nothing to do with the heart itself. Heartburn is pain felt in the chest by a burning sensation in the esophagus. Here, you can see the pizza passing from the mouth to the esophagus and on to the stomach. At the junction between the stomach and esophagus is the lower esophageal sphincter. This muscular sphincter acts as a valve that normally keeps food and stomach acid in the stomach, and prevents the stomach’s contents from regurgitating back into the esophagus. However, certain foods may affect the lower esophageal sphincter, making it less effective. That’s how heartburn begins. The stomach produces hydrochloric acid to digest food. The stomach has a mucous lining that protects it from hydrochloric acid, but the esophagus does not. So, when food and stomach acid regurgitate back into the esophagus, a burning feeling is felt near the heart. This feeling is known as heartburn. Antacids may be used to relieve heartburn by making stomach juices less acidic, thereby reducing the burning feeling felt in the esophagus. If heartburn becomes frequent or prolonged, medical intervention may be necessary to correct the problem.
Symptoms
Typical symptoms of GERD are:
- Heartburn or a burning pain in the chest
Heartburn
Heartburn is a painful burning feeling just below or behind the breastbone. Most of the time, it comes from the esophagus. The pain often rises in ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Bringing food back up (regurgitation)
Less common symptoms are:
- Nausea after eating
- Cough or wheezing
Cough
Coughing is an important way to keep your throat and airways clear. But too much coughing may mean you have a disease or disorder. Some coughs are d...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleWheezing
Wheezing is a high-pitched whistling sound during breathing. It occurs when air moves through narrowed breathing tubes in the lungs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Difficulty swallowing (make sure to discuss this with your provider)
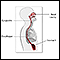
Difficulty swallowing
Difficulty with swallowing is the feeling that food or liquid is stuck in the throat or at any point before the food enters the stomach. This proble...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Hiccups
Hiccups
A hiccup is an unintentional movement (spasm) of the diaphragm, the muscle at the base of the lungs. The spasm is followed by quick closing of the v...
Read Article Now Book Mark Article - Hoarseness or change in voice
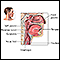
Hoarseness
Hoarseness refers to difficulty making sounds when trying to speak. Vocal sounds may be weak, breathy, scratchy, or husky, and the pitch or quality ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Sore throat
Sore throat
Pharyngitis, or sore throat, is discomfort, pain, or scratchiness in the throat. It often makes it painful to swallow.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Symptoms may get worse when you bend over or lie down, or after you eat. Symptoms may also be worse at night.
Exams and Tests
You may not need any tests if your symptoms are mild.
If your symptoms are severe or they come back after you have been treated, your provider may recommend a test called an upper endoscopy (esophagogastroduodenoscopy).
Upper endoscopy
Esophagogastroduodenoscopy (EGD) is a test to examine the lining of the esophagus, stomach, and first part of the small intestine (the duodenum)....
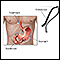
- This is a test to examine the lining of the esophagus, stomach, and first part of the small intestine.
- It is done with a small camera (flexible endoscope) that is inserted down the throat.
You may also be recommended to have one or more of the following tests:
- A test that measures how often stomach acid enters the esophagus. This can be done with a catheter through the nose or with a device clipped to the bottom of your esophagus during an upper endoscopy.
- A test to measure the pressure inside the lower part of the esophagus (esophageal manometry).
Esophageal manometry
Esophageal manometry is a test to measure how well the esophagus is working.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - A test to measure fluid and air coming up from the esophagus (impedance).
A positive stool occult blood test may diagnose bleeding that is coming from the irritation in the esophagus, stomach, or intestines.
Stool occult blood test
The stool guaiac test looks for hidden (occult) blood in a stool sample. It can find blood even if you cannot see it yourself. It is a common type ...

Treatment
You can make many lifestyle changes to help treat your symptoms such as avoiding tobacco, alcohol, or foods that cause your symptoms.
Lifestyle changes
Gastroesophageal reflux disease (GERD) is a condition in which the stomach contents leak backwards from the stomach into the esophagus (the tube from...
Other tips include:
- If you are overweight or obese, in many cases, losing weight can help.
- Raise the head of the bed if your symptoms get worse at night.
- Have your dinner 2 to 3 hours before going to sleep. Avoid eating food after dinner.
- Avoid medicines such as aspirin, ibuprofen (Advil, Motrin), or naproxen (Aleve, Naprosyn). Take acetaminophen (Tylenol) to relieve pain.
- Take all of your medicines with plenty of water. When your provider gives you a new medicine, ask whether it will make your heartburn worse.
You may use over-the-counter antacids after meals and at bedtime, although the relief may not last very long. Common side effects of antacids include diarrhea or constipation.
Over-the-counter antacids
Antacids help to treat heartburn (indigestion). They work by neutralizing the stomach acid that causes heartburn. You can buy many antacids without ...
Read Article Now Book Mark ArticleOther over-the-counter and prescription medicines can treat GERD. They work more slowly than antacids, but give you longer relief. Your pharmacist, provider, or nurse can tell you how to take these medicines.
- Proton pump inhibitors (PPIs) decrease the amount of acid produced in your stomach.
- H2 blockers also lower the amount of acid released in the stomach.
- Potassium competitive acid blockers (PCABs) are the newest medicines that decrease stomach acid.
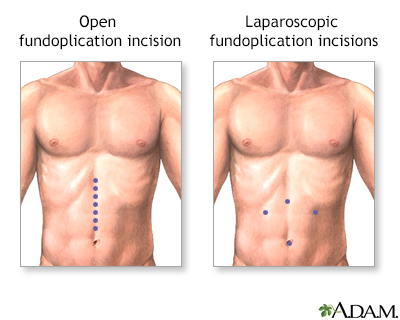
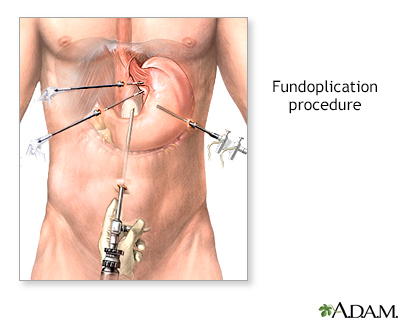
Anti-reflux surgery may be an option for people whose symptoms do not go away with lifestyle changes and medicines. Heartburn and other symptoms should improve after surgery. But you may still need to take medicines for your heartburn. Your provider will recommend certain tests before any surgery for GERD to help you get the best outcome.
There are also new therapies for reflux that can be performed through an endoscope (a flexible tube passed through the mouth into the stomach).
Outlook (Prognosis)
Most people respond to lifestyle changes and medicines. However, many people feel the need to continue taking medicines to control their symptoms. If you have inflammation from your GERD (esophagitis) or precancerous changes (Barrett esophagus), your provider may recommend staying on these medicines. Otherwise speak with your provider about whether you need to stay on medicines long term.
Possible Complications
Complications may include:
- Worsening of asthma
- A change in the lining of the esophagus that can increase the risk of cancer (Barrett esophagus)
Barrett esophagus
Barrett esophagus (BE) is a disorder in which the lining of the esophagus is damaged by stomach acid leading to changes in the cells of the lining. ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Bronchospasm (irritation and spasm of the airways due to acid)
- Long-term (chronic) cough or hoarseness
- Dental problems
- Ulcer or inflammation in the esophagus
Ulcer
An ulcer is a crater-like sore on the skin or mucous membrane. Ulcers form when the top layers of skin or tissue have been removed. They can occur ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Stricture (a narrowing of the esophagus due to scarring from chronic irritation)
When to Contact a Medical Professional
Contact your provider if symptoms do not improve with lifestyle changes or medicine.
Also contact your provider if you have:
- Bleeding
- Choking (coughing, shortness of breath)
Shortness of breath
Someone who is very ill may have trouble breathing or feel as if they are not getting enough air. This condition is called shortness of breath. The...
Read Article Now Book Mark Article - Feeling filled up quickly when eating
- Frequent vomiting
- Hoarseness
- Loss of appetite
Loss of appetite
A decreased appetite is when your desire to eat is reduced. The medical term for a loss of appetite is anorexia.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Trouble swallowing (dysphagia) or pain with swallowing (odynophagia)
Pain with swallowing
Painful swallowing is any pain or discomfort while swallowing. You may feel it high in the neck or lower down behind the breastbone. Most often, th...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Weight loss
- A feeling like food or pills are sticking behind the breast bone
Prevention
Avoiding factors that cause heartburn may help prevent symptoms. Obesity is linked to GERD. Maintaining a healthy body weight may help prevent the condition.
Heartburn
Heartburn is a painful burning feeling just below or behind the breastbone. Most of the time, it comes from the esophagus. The pain often rises in ...

Reviewed By
Jenifer K. Lehrer, MD, Gastroenterologist, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Falk GW, Katzka DA. Diseases of the esophagus. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 124.
Katz PO, Dunbar KB, Schnoll-Sussman FH, Greer KB, Yadlapati R, Spechler SJ. ACG Clinical Guideline for the diagnosis and management of Gastroesophageal Reflux Disease. Am J Gastroenterol. 2022;117(1):27-56. PMID: 34807007 pubmed.ncbi.nlm.nih.gov/34807007/.
National Institute of Diabetes and Digestive and Kidney Diseases website. Acid reflux (GER & GERD) in adults. www.niddk.nih.gov/health-information/digestive-diseases/acid-reflux-ger-gerd-adults. Updated July 2020. Accessed March 17, 2025.
Richter JE, Vaezi MF. Gastroesophageal reflux disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 46.




 All rights reserved.
All rights reserved.