Drug-induced pulmonary disease
Interstitial lung disease - drug inducedDrug-induced pulmonary disease is lung disease brought on by a bad reaction to a medicine. Pulmonary means related to the lungs.
Causes
Many types of lung injury can result from medicines. It is usually impossible to predict who will develop lung disease from a medicine.
Types of lung problems or diseases that may be caused by medicines include:
-
Allergic reactions -- asthma, hypersensitivity pneumonitis, or eosinophilic pneumonia
Allergic reactions
Allergic reactions are sensitivities to substances called allergens that come into contact with the skin, nose, eyes, respiratory tract, and gastroin...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleAsthma
Asthma is a chronic disease that causes the airways of the lungs to swell and narrow. It leads to breathing difficulty such as wheezing, shortness o...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleHypersensitivity pneumonitis
Hypersensitivity pneumonitis is inflammation of the lungs due to breathing in dust, fungus, molds, or other substances.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleEosinophilic pneumonia
Simple pulmonary eosinophilia is inflammation of the lungs from an increase in eosinophils, a type of white blood cell. Pulmonary means related to t...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Bleeding into the lung air sacs, called alveoli (alveolar hemorrhage)
- Swelling and inflamed tissue in the main passages that carry air to the lungs (bronchitis)
Bronchitis
Acute bronchitis is swelling and inflamed tissue in the bronchi, the main passages that carry air to the lungs. This swelling narrows the airways, w...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Damage to lung tissue (interstitial fibrosis)
Interstitial fibrosis
Interstitial lung disease (ILD) is a group of lung disorders in which the lung tissues become inflamed and then damaged.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Drugs that cause the immune system to mistakenly attack and destroy healthy body tissue, such as drug-induced lupus erythematosus
Drug-induced lupus erythematosus
Drug-induced lupus erythematosus is an autoimmune disorder that is triggered by a reaction to a medicine.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Granulomatous lung disease -- a type of inflammation in the lungs
- Inflammation of the lung air sacs (pneumonitis or infiltration)
- Lung vasculitis (inflammation of lung blood vessels)
-
Lymph node swelling
Lymph node swelling
Lymph nodes are present throughout your body. They are an important part of your immune system. Lymph nodes help your body recognize and fight germ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Swelling and irritation (inflammation) of the chest area between the lungs (mediastinitis)
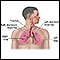
Mediastinitis
Mediastinitis is swelling and irritation (inflammation) of the chest area between the lungs (mediastinum). This area contains the heart, large blood...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Abnormal buildup of fluid in the lungs (pulmonary edema)
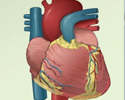
Pulmonary edema
Pulmonary edema is an abnormal buildup of fluid in the lungs. This buildup of fluid leads to shortness of breath.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Buildup of fluid between the layers of tissue that line the lungs and chest cavity (pleural effusion)
Pleural effusion
A pleural effusion is a buildup of fluid between the layers of tissue that line the lungs and chest cavity.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Abnormal pressure of the arteries that bring blood to the lungs (pulmonary hypertension)
Many medicines and substances are known to cause lung disease in some people. These include:
- Antibiotics, such as nitrofurantoin and sulfa drugs
- Heart medicines, such as amiodarone
-
Chemotherapy drugs such as bleomycin, cyclophosphamide, and methotrexate
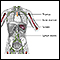
Chemotherapy
The term chemotherapy is used to describe cancer-killing drugs. Chemotherapy may be used to:Cure the cancerShrink the cancerPrevent the cancer from ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Immunotherapy drugs that are used to treat cancer
- Street drugs
Symptoms
Symptoms may include any of the following:
-
Bloody sputum
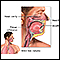
Bloody sputum
Coughing up blood is the spitting up of blood or bloody mucus from the lungs and throat (respiratory tract). Hemoptysis is the medical term for cough...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Chest pain
Chest pain
Chest pain is discomfort or pain that you feel anywhere along the front of your body between your neck and upper abdomen.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Cough
Cough
Coughing is an important way to keep your throat and airways clear. But too much coughing may mean you have a disease or disorder. Some coughs are d...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Fever
Fever
Fever is the temporary increase in the body's temperature in response to a disease or illness. A child has a fever when the temperature is at or abov...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Shortness of breath
Shortness of breath
Breathing difficulty may involve:Difficult breathing Uncomfortable breathingFeeling like you are not getting enough air
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Wheezing
Wheezing
Wheezing is a high-pitched whistling sound during breathing. It occurs when air moves through narrowed breathing tubes in the lungs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Exams and Tests
The health care provider will perform a physical exam and listen to your chest and lungs with a stethoscope. Abnormal breath sounds may be heard.
Tests that may be done include:
-
Arterial blood gases
Arterial blood gases
Blood gases are a measurement of how much oxygen and carbon dioxide are in your blood. They also determine the acidity (pH) of your blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Blood test to check for an autoimmune disorder
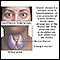
Autoimmune
An autoimmune disorder occurs when the body's immune system attacks and destroys healthy body tissue by mistake. There are more than 80 autoimmune d...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Blood chemistry
-
Bronchoscopy
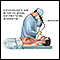
Bronchoscopy
Bronchoscopy is a test to view the airways and diagnose lung disease. It may also be used during the treatment of some lung conditions.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Complete blood count with blood differential
Complete blood count
A complete blood count (CBC) test measures the following:The number of white blood cells (WBC count)The number of red blood cells (RBC count)The numb...
 ImageRead Article Now Book Mark Article
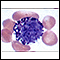
ImageRead Article Now Book Mark ArticleBlood differential
The blood differential test measures the percentage of each type of white blood cell (WBC) that you have in your blood. It also reveals if there are...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Chest CT scan
Chest CT scan
A chest CT (computed tomography) scan is an imaging method that uses x-rays to create cross-sectional pictures of the chest and upper abdomen....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Chest x-ray
Chest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
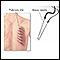
Lung biopsy (in rare cases)
Lung biopsy
A lung needle biopsy is a method to remove a piece of lung tissue for examination. If it is done through the wall of your chest, it is called a tran...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Lung function tests
Lung function tests
Pulmonary function tests are a group of tests that measure breathing and how well the lungs are functioning.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Thoracentesis (if pleural effusion is present)
Thoracentesis
Thoracentesis is a procedure to remove fluid from the space between the lining of the outside of the lungs (pleura) and the wall of the chest....
Read Article Now Book Mark Article
Treatment
The first step is to stop the medicine that is causing the problem. Other treatments depend on your specific symptoms. For example, you may need oxygen until the drug-induced lung disease improves. Anti-inflammatory medicines called corticosteroids are most often used to quickly reverse the lung inflammation.
Outlook (Prognosis)
Acute episodes usually go away within 48 to 72 hours after the medicine has been stopped. Chronic symptoms may take longer to improve.
Acute
Acute means sudden. Acute symptoms appear, change, or worsen rapidly. It is the opposite of chronic.
Chronic
Chronic refers to something that continues over an extended period of time. A chronic condition is usually long-lasting and does not easily or quick...

Some drug-induced lung diseases, such as pulmonary fibrosis, may never go away and can worsen, even after the medicine or substance is stopped and can lead to severe lung disease and death.
Possible Complications
Complications that may develop include:
-
Diffuse interstitial pulmonary fibrosis
Diffuse interstitial pulmonary fibrosis
Interstitial lung disease (ILD) is a group of lung disorders in which the lung tissues become inflamed and then damaged.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Hypoxemia (low blood oxygen)
-
Respiratory failure
Respiratory failure
Respiratory acidosis is a condition that occurs when your lungs can't remove all of the carbon dioxide produced by your body. This causes the blood ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
When to Contact a Medical Professional
Contact your provider if you develop symptoms of this disorder.
Prevention
Note any past reaction you have had to a medicine, so that you can avoid the medicine in the future. Wear a medical alert bracelet if you have known drug reactions. Stay away from street drugs.
References
Kurian ST, Walker CM, Chung JH. Drug-induced lung disease. In: Walker CM, Chung JH, eds. Muller's Imaging of the Chest. 2nd ed. Philadelphia, PA: Elsevier; 2019:chap 65.
Limper AH. Drug-induced pulmonary disease. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 99.
-
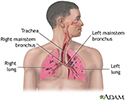
Respiratory system - illustration
Air is breathed in through the nasal passageways, travels through the trachea and bronchi to the lungs.
Respiratory system
illustration
-
Scleroderma - InDepth
(In-Depth)
-
Gastroesophageal reflux disease
(Alt. Medicine)
-
Systemic lupus erythematosus - InDepth
(In-Depth)
-
Gastroesophageal reflux disease and heartburn - InDepth
(In-Depth)
-
Restless legs syndrome and related disorders - InDepth
(In-Depth)
-
Asthma in adults - InDepth
(In-Depth)
-
Depression - InDepth
(In-Depth)
-
Asthma in children and adolescents - InDepth
(In-Depth)
-
Colorectal cancer
(Alt. Medicine)
-
Peptic ulcer
(Alt. Medicine)
Review Date: 5/3/2023
Reviewed By: Denis Hadjiliadis, MD, MHS, Paul F. Harron, Jr. Professor of Medicine, Pulmonary, Allergy, and Critical Care, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.