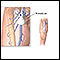
Deep vein thrombosis
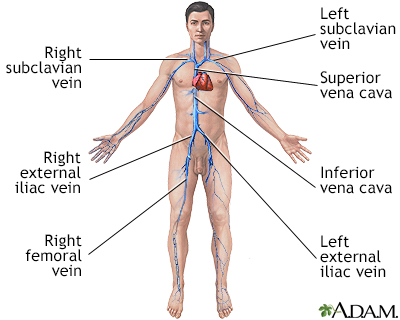
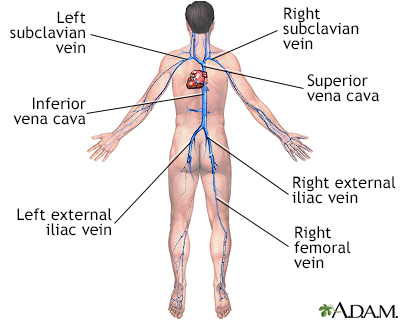
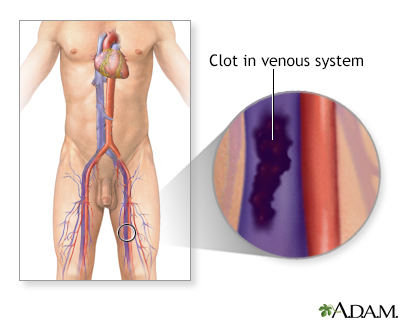
Deep vein thrombosis (DVT) is a condition that occurs when a blood clot forms in a vein deep inside a part of the body. DVT mainly affects the large veins in the lower leg and thigh, but can occur in other deep veins, such as in the arms and pelvis. DVT most often affects only one side of the body.
Causes
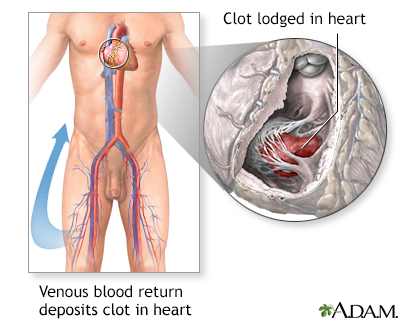
DVT is most common in adults over age 60. But it can occur at any age. When a clot breaks off and moves through the bloodstream, it is called an embolism. An embolism can get stuck in the blood vessels in the brain, lungs, heart, or another area, leading to severe damage.
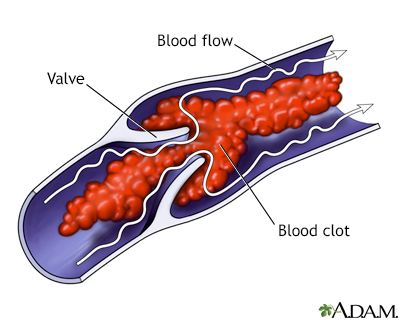
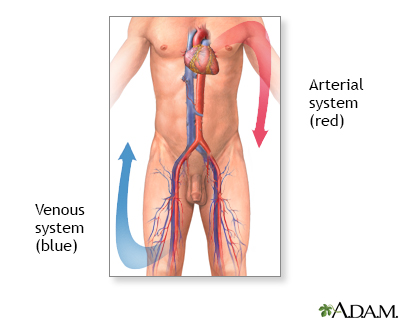
Blood clots may form when something slows or changes the flow of blood in the veins.
Blood clots
Blood clots are clumps that occur when blood hardens from a liquid to a solid. A blood clot that forms inside one of your veins or arteries is calle...
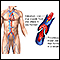
Risk factors include:
- A pacemaker catheter that has been passed through a vein in the groin
- Bed rest or sitting in one position for too long, such as plane or car travel
- Family history of blood clots
- Fractures in the pelvis or legs
- Giving birth within the last 6 months
- Pregnancy
- Obesity
Obesity
Obesity means weighing more than what is healthy for a given height. Obesity is a serious, chronic disease. It can lead to other health problems, i...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Recent surgery (most commonly hip, knee, or female pelvic surgery)
- Too many blood cells being made by the bone marrow, causing the blood to be thicker than normal (polycythemia vera)
Polycythemia vera
Polycythemia vera (PV) is a bone marrow disease that leads to an abnormal increase in the number of blood cells. The red blood cells are the most af...
Read Article Now Book Mark Article - Having an indwelling (long-term) catheter in a blood vessel
- Age greater than 60
Blood is more likely to clot in someone who has certain problems or disorders, such as:
- Cancer
- Certain autoimmune disorders, such as lupus
Autoimmune disorders
An autoimmune disorder occurs when the body's immune system attacks and destroys healthy body tissue by mistake. There are more than 80 autoimmune d...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleLupus
Systemic lupus erythematosus (SLE) is an autoimmune disease. In this disease, the immune system of the body mistakenly attacks healthy tissue. It c...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Cigarette smoking
- Conditions that make it more likely to develop blood clots
- Taking estrogens or birth control pills (this risk is even higher with smoking)
Sitting for long periods when traveling can increase the risk for DVT. This is most likely when you also have one or more of the risk factors listed above.
Symptoms
DVT mainly affects the large veins in the lower leg and thigh, most often on one side of the body. The clot can block blood flow and cause:
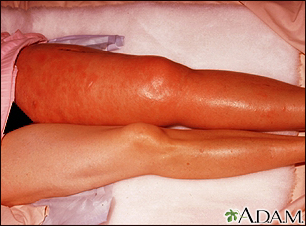
- Redness of the skin
- Skin that feels warm to the touch
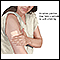
- Swelling (edema) of a leg or arm
- Pain or tenderness in a leg or arm
Exams and Tests
Your health care provider will perform a physical exam. The exam may show a red, swollen, or tender leg.
Tests that are often done to diagnose a DVT are:
- D-dimer blood test
D-dimer blood test
D-dimer tests are used to check for blood clotting problems. Blood clots can cause health problems, such as:Deep vein thrombosis (DVT)Disseminated i...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Doppler ultrasound exam of the area of concern
Doppler ultrasound exam
This test uses ultrasound to look at the blood flow in the large arteries and veins in the arms or legs.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - A pelvic or abdominal MRI or CT
Blood tests may be done to check if you have an increased chance of blood clotting, including:
- Activated protein C resistance (checks for the Factor V Leiden mutation)
- Genetic testing for other mutations, such as the prothrombin G20210A mutation
- Antithrombin III levels
- Antiphospholipid antibodies
- Complete blood count (CBC)
Complete blood count
A complete blood count (CBC) test measures the following:The number of white blood cells (WBC count)The number of red blood cells (RBC count)The numb...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Lupus anticoagulant
- Protein C and protein S levels
Protein C
Protein C is a normal substance in the body that prevents blood clotting. A blood test can be done to see how much of this protein you have in your ...
Read Article Now Book Mark ArticleProtein S
Protein S is a normal substance in your body that prevents blood clotting. A blood test can be done to see how much of this protein you have in your...
Read Article Now Book Mark Article
Treatment
Your provider will give you medicine to thin your blood (called an anticoagulant). This will keep more clots from forming or old ones from getting bigger.
Heparin is often the first medicine you will receive.
- If heparin is given through a vein (IV), you must stay in the hospital. However, most people can be treated without staying in the hospital.
- Low molecular weight heparin can be given by injection under your skin once or twice a day. You may not need to stay in the hospital as long, or at all, if you are prescribed this type of heparin.
One type of blood-thinning medicine called warfarin (Coumadin or Jantoven) may be started along with heparin. Warfarin is taken by mouth. It takes several days to fully work.
Another class of blood thinners are called direct oral anticoagulants (DOAC), including:
- Rivaroxaban (Xarelto)
- Apixaban (Eliquis)
- Dabigatran (Pradaxa)
- Edoxaban (Savaysa)
These medicines work in a similar way to heparin and can be used right away in place of heparin. Your provider will decide which medicine is right for you.
You will most likely take a blood thinner for at least 3 months. Some people take it longer, or even for the rest of their lives, depending on their risk for another clot.
When you are taking a blood thinning medicine, you are more likely to bleed, even from activities you have always done. If you are taking a blood thinner at home:
If you are taking a blood thinner at ho...
Warfarin is a medicine that makes your blood less likely to form clots. It is important that you take warfarin exactly as you have been told. Chang...
Read Article Now Book Mark Article- Take the medicine just the way your provider prescribed it.
- Ask your provider what to do if you miss a dose.
- Ask your provider if you need to take an oral medicine on an empty stomach.
- Get blood tests as advised by your provider to make sure you are taking the right dose. These tests are usually needed with people who are taking warfarin.
- Find out how to watch for problems caused by the medicine.
In rare cases, you may need a procedure instead of or in addition to anticoagulants. These may involve:
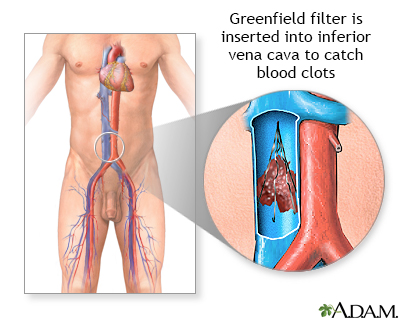
- Placing a filter in the body's largest vein to prevent blood clots from traveling to the lungs
- Removing a large blood clot from the vein or injecting clot-busting medicines
Follow any other instructions you are given to treat your DVT.
Instructions
You were treated for deep vein thrombosis (DVT). This is a condition in which a blood clot forms in a vein that is not on or near the surface of the...
Outlook (Prognosis)
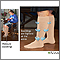
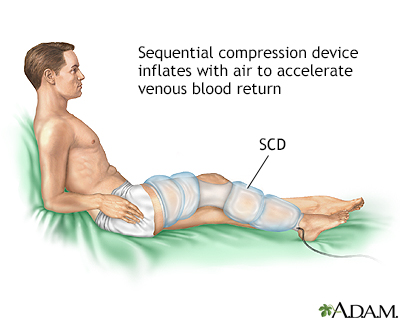
DVT often goes away without a problem, but the condition can return. The symptoms can appear right away or you may not develop them for one or more years afterward. Wearing compression stockings during and after the DVT may help prevent this problem.
Possible Complications
Complications of DVT may include:
- Pulmonary embolism (which may be fatal)
- Constant or intermittent pain and swelling (post-phlebitic or post-thrombotic syndrome)
- Varicose veins
- Non-healing skin ulcers (less common)
- Changes in skin color
When to Contact a Medical Professional
Contact your provider if you have symptoms of DVT.
Go to the emergency room or call the local emergency number (such as 911) if you have DVT and you develop:
- Chest pain
Chest pain
Chest pain is discomfort or pain that you feel anywhere along the front of your body between your neck and upper abdomen.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Coughing up blood
- Difficulty breathing
Difficulty breathing
Breathing difficulty may involve:Difficult breathing Uncomfortable breathingFeeling like you are not getting enough air
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Fainting
Fainting
Fainting is a brief loss of consciousness due to a drop in blood flow to the brain. The episode most often lasts less than a couple of minutes and y...
Read Article Now Book Mark Article - Loss of consciousness
Loss of consciousness
Decreased alertness is a state of reduced awareness and is often a serious condition. A coma is the most severe state of decreased alertness from whi...
Read Article Now Book Mark Article - Other severe symptoms
Prevention
To prevent DVT:
- Move your legs often during long plane trips, car trips, and other situations in which you are sitting or lying down for long periods.
- Take blood-thinning medicines your provider prescribes.
- Do not smoke. Smoking increases the risk for blood clots. Talk to your provider if you need help quitting.
Quitting
There are many ways to quit smoking. There are also resources to help you. Family members, friends, and co-workers may be supportive. But to be su...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Reviewed By
John Roberts, MD, Professor of Internal Medicine (Medical Oncology), Yale Cancer Center, New Haven, CT. He is board certified in Internal Medicine, Medical Oncology, Pediatrics, Hospice and Palliative Medicine. Review provided by VeriMed Healthcare Network. Internal review and update on 02/03/2024 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Aziz MU, Zahid M, Weber TM, Robbin ML. Peripheral viens. In: Rumack CM, Levine D, eds. Diagnostic Ultrasound. 6th ed. Philadelphia, PA: Elsevier; 2024:chap 26.
Chan NC, Weitz JI. Venous thromboembolism. In: Hoffman R, Benz EJ, Silberstein LE, et al, eds. Hematology: Basic Principles and Practice. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 140.
Kabrhel C. Pulmonary embolism and deep vein thrombosis. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 74.
Stevens SM, Woller SC, Kreuziger LB, et al. Antithrombotic therapy for VTE disease: second update of the CHEST guideline and expert panel report. Chest. 2021;160(6):e545-e608. PMID: 34352278 pubmed.ncbi.nlm.nih.gov/34352278/.
Weitz JI, Eikelboom JW. Venous thrombosis and embolism. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 68.

 All rights reserved.
All rights reserved.