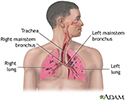
Primary alveolar hypoventilation
Ondine's curse; Ventilatory failure; Diminished hypoxic ventilator drive; Diminished hypercapnic ventilator drivePrimary alveolar hypoventilation is a rare disorder in which a person does not take enough breaths per minute. The lungs and airways are normal.
Causes
Normally, when the oxygen level in the blood is low or the carbon dioxide level is high, there is a signal from the brain to breathe more deeply or quickly. In people with primary alveolar hypoventilation, this change in breathing does not happen.
The cause of this condition is unknown. Some people have a specific genetic defect.
The disease mainly affects men 20 to 50 years old. It may also occur in children.
Symptoms
Symptoms are usually worse during sleep. Episodes of stopped breathing (apnea) often occur while sleeping. Often there is no shortness of breath during the day.
Apnea
Breathing that stops from any cause is called apnea. Slowed breathing is called bradypnea. Labored or difficult breathing is known as dyspnea....
Read Article Now Book Mark ArticleSymptoms include:
-
Bluish coloration of the skin caused by lack of oxygen (cyanosis)
Bluish coloration of the skin
A bluish color to the skin or mucous membrane is usually due to a lack of oxygen in the blood. The medical term is cyanosis.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleCyanosis
A bluish color to the skin or mucous membrane is usually due to a lack of oxygen in the blood. The medical term is cyanosis.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Daytime drowsiness
-
Fatigue
Fatigue
Fatigue is a feeling of weariness, tiredness, or lack of energy.
Read Article Now Book Mark Article - Morning headaches
- Swelling of the ankles
- Waking up from sleep unrested
- Waking up many times at night
People with this disease are very sensitive to even small doses of sedatives or narcotics. These drugs can make their breathing problem much worse.
Exams and Tests
The health care provider will perform a physical exam and ask about symptoms.
Tests will be done to rule out other causes. For example, muscular dystrophy can make the rib muscles weak, and chronic obstructive pulmonary disease (COPD) damages the lung tissue itself. A small stroke can affect the breathing center in the brain.
Tests that may be done include:
- Measuring levels of oxygen and carbon dioxide in the blood (arterial blood gases)
Arterial blood gases
Blood gases are a measurement of how much oxygen and carbon dioxide are in your blood. They also determine the acidity (pH) of your blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Chest x-ray or CT scan
Chest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Hematocrit and hemoglobin blood tests to check oxygen carrying ability of red blood cells
Hematocrit
Hematocrit is a blood test that measures how much of a person's blood is made up of red blood cells. This measurement depends on the number of and s...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleHemoglobin
Hemoglobin is a protein in red blood cells that carries oxygen. The hemoglobin test measures how much hemoglobin is in your blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Lung function tests
Lung function tests
Pulmonary function tests are a group of tests that measure breathing and how well the lungs are functioning.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Overnight oxygen level measurements (oximetry)
- Sleep study (polysomnography)
Polysomnography
Polysomnography is a sleep study. This test records certain body functions as you sleep, or try to sleep. Polysomnography is used to diagnose sleep...
Read Article Now Book Mark Article
Treatment
Medicines that stimulate the respiratory system may be used but do not always work. Mechanical devices that assist breathing, particularly at night, may be helpful in some people. Oxygen therapy may help in a few people, but may worsen night symptoms in others.
Respiratory
The words "respiratory" and "respiration" refer to the lungs and breathing.

Outlook (Prognosis)
Response to treatment varies.
Possible Complications
Low blood oxygen level can cause high blood pressure in the lung blood vessels. This can lead to cor pulmonale (right-sided heart failure).
Cor pulmonale
Cor pulmonale is a condition that causes the right side of the heart to fail. Long-term high blood pressure in the arteries of the lung and right ve...
When to Contact a Medical Professional
Contact your provider if you have symptoms of this disorder. Seek medical care right away if bluish skin occurs.
Prevention
There is no known prevention. You should avoid using sleep medicines or other drugs that can cause drowsiness.
References
Lumb A, Thomas C. Control of breathing. In: Lumb A, Thomas C, eds. Nunn and Lumb's Applied Respiratory Physiology. 9th ed. Philadelphia, PA: Elsevier; 2021:chap 4.
Malhotra A, Powell F. Disorders of ventilatory control. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 80.
Weinberger SE, Cockrill BA, Mandel J. Disorders of ventilatory control. In: Weinberger SE, Cockrill BA, Mandel J, eds. Principles of Pulmonary Medicine. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 18.
-
Respiratory system - illustration
Air is breathed in through the nasal passageways, travels through the trachea and bronchi to the lungs.
Respiratory system
illustration
Review Date: 7/31/2022
Reviewed By: Denis Hadjiliadis, MD, MHS, Paul F. Harron Jr. Professor of Medicine, Pulmonary, Allergy, and Critical Care, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.